Sickle cell disease (SCD), also known as sick cell anaemia, encompasses a group of genetic disorders characterized by abnormal haemoglobin in red blood cells.
The disease is not contagious but can be passed on from parents with a defected gene to a child, through in an autosomal recessive inheritance pattern. The abnormal haemoglobin is termed sickle haemoglobin or Haemoglobin S.
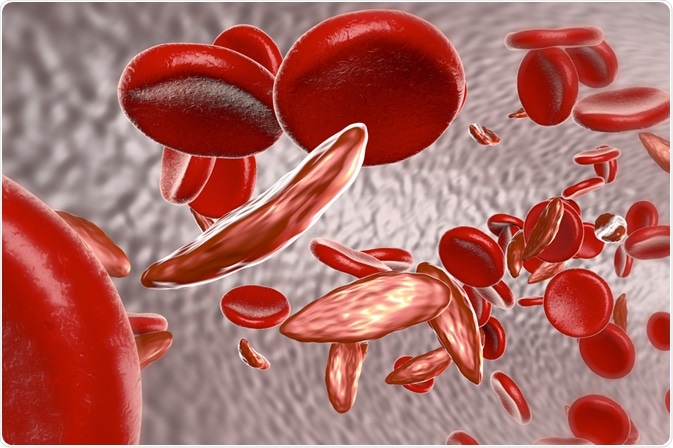
Image Credit: Kateryna Kon/Shutterstock.com
Genetic inheritance
Sickle cell disease is inherited in as autosomal recessive pattern. Autosomal means that the gene mutation does not exist on the sex chromosome and, therefore, affects male and females equally. Recessive means that both parents must carry a gene mutation, although they may not be symptomatic for the child to suffer from sickle cell disease.
For example, if each parent is an asymptomatic genetic carrier of sickle cell disease, each of their children will have the same risk of inheriting the gene mutations:
- 25% risk of inheriting two gene mutations and affected by SCD.
- 50% risk of inheriting one gene mutation and a genetic carrier of SCD.
- 25% risk of inheriting no gene mutation and unaffected by SCD
Signs and symptoms
Most individuals will begin to develop symptoms in early childhood, such as:
- Anemia
- Frequent infections
- Pain episodes
- Jaundice
- Fatigue
- Swollen hands and feet
The severity of these symptoms can vary significantly for each individual with the disease, according to the specific characteristics of their disease and general health.
Pathophysiology
The role of haemoglobin involves the supply of oxygen to cells throughout the body, which is essential for normal bodily functions. Sickle haemoglobin differs from normal haemoglobin because it forms a different rod-like shape and are not flexible, which can hemolyse and lead to blockages in the blood vessels to disrupt the blood flow.
This can cause tissues to lack a supply of oxygen, which can cause sudden and severe pain, known as a pain crisis, which commonly requires emergency medical care.
Most children affected by the disease do not usually suffer from significant pain between pain crises, although adults with the disease may experience chronic pain more frequently.
Over time, the effect of the sickle haemoglobin can lead to organ damage of the spleen, brain, eyes, lungs, liver, heart, kidneys, penis, joints, bones and skin.
Red blood cells in people affected by SCD do no last as long as cells with healthy haemoglobin, which can lead to a lower number of red blood cells than normal and resulting symptoms of anaemia, such as fatigue.
Types
There are several different types of sickle cell disease, according to the abnormality of the haemoglobin molecule. These include:
- Hemoglobin SS
- Hemoglobin SC
- Hemoglobin Sβ0 thalassemia
- Hemoglobin Sβ+ thalassemia
- Hemoglobin SD
- Hemoglobin SE
Prognosis
Patients with sickle cell disease are expected to suffer for the duration of their life, although the severity of the disease and symptoms can vary significantly. The average life expectancy in the 1970s was approximately 14 years, whereas today someone with sickle cell disease can expect to live until 40 to 60 years of age.
Treatments
The sole cure for sickle cell disease is currently hematopoietic stem cell transplantation (HSCT). However, this is not an option for many patients as there is no suitable donor or the patient is too old for the transplant to be successful.
For other patients, there are various treatment methods that can help to reduce symptoms and increase the expected lifespan of individuals.
References
Further Reading
Last Updated: Jan 17, 2022