Endometrial hyperplasia (EH) is a condition in which the uterine lining is thicker than normal. It may have many causes, but the most important association is with endometrial malignancy. For this reason, it is mandatory to distinguish between different types of EH, namely, those which are benign and those which are precancerous.
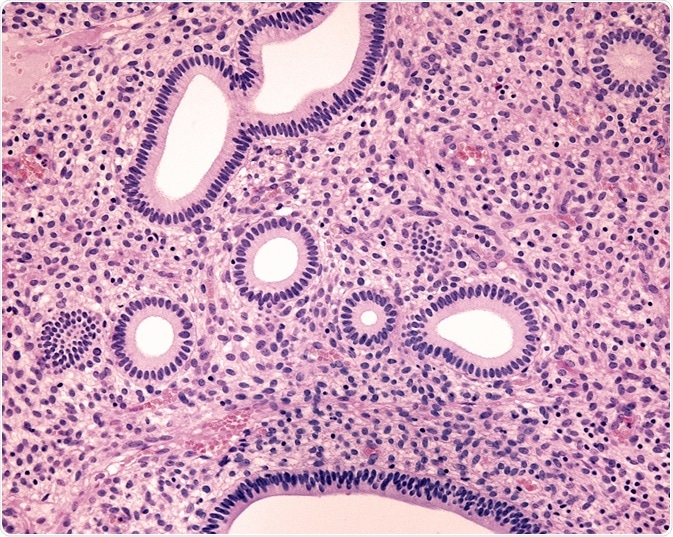
Credit: Jose Luis Calvo/ Shutterstock.com
Classification of EH
The most useful systems of classification based on microscopic appearances categorize EH as:
- EH/ benign EH/ EH without atypia (based on the European study group/ Mutter et al/ WHO 2014 classifications respectively)
- Endometrioid neoplasia (EN)/ endometrial intraepithelial neoplasia (EIN)/ Atypical EH – as per the above systems respectively
The first category is a response to abnormal estrogen stimulation of the endometrium, and regresses once the exposure ceases and adequate progesterone exposure is initiated. The cells are normal in appearance and there are no mutations associated with malignancy
On the other hand, the second type of lesion is premalignant, with genetic changes linked to malignant transformation, and is associated strongly with coexistent endometrioid cancer (in 36%), or a high risk of developing it within a few years.
Treatment
The management of EH depends on the etiology and direction of the lesion, thus factors which determine the choice of treatment include:
- The histopathologic diagnosis
- Whether the woman wants to conceive again
- Whether she is exposed to estrogens currently
- Severity of symptoms
- General health
Treatment of EH without atypia
In most cases, benign EH is treated conservatively. Attention is given to identifying and removing sources of estrogen, whether exogenous or endogenous. Modifiable risk factors of this condition include:
- Sedentary lifestyle with lack of exercise
- Obesity in which peripheral fatty tissue containing the enzyme aromatase convert androgens to estrogens, promoting endometrial thickening
- Diabetes mellitus
- Unhealthy diet which promotes weight gain
- The use of estrogen-only hormone replacement therapy (HRT) in postmenopausal women, or other estrogen delivery systems, which should be replaced with combined cyclic or continuous HRT.
- Approximately 1% of patients who are on combined HRT develop benign EH. In such cases, the dose should be increased or they should be switched to 3 months of progestin-only therapy to encourage the regression of the hyperplastic endometrium.
Progestational treatment
In most cases, benign EH may be treated with progesterone, in various 14-day regimens, using formulations such as:
- Medroxy progesterone acetate (MPA) 10 mg by mouth daily
- Micronized progesterone 300 mg by mouth daily
Each 14-day cycle is followed by cyclic bleeding and the endometrium is reassessed by a biopsy after 3 or 4 months of this treatment.
Progestins inhibit cell division in the endometrium within 11 days of initiation of treatment. This is important in reversing the proliferative changes of EH. The typical features of a progesterone-stimulated endometrium include atrophy of the glandular epithelium, increased eosinophilic staining of the cytoplasm and changes in the stromal fluid retention. The response to progestins is determined mostly by the progestin receptor status of the abnormal endometrium.
Outcomes
- Patients showing complete regression of EH should:
- continue this therapy.
- use combined (estrogen plus progesterone) hormone replacement therapy if postmenopausal, either in cyclic or combined form
- If only a partial regression occurs, the doses of progesterone are increased and the 14-day regimen continued using:
- MPA 10 mg by mouth four times daily
- Megestrol acetate 80 mg daily by mouth
After 3 months the endometrium is reassessed by biopsy.
- If there is no response, or patients show breakthrough bleeding, the treatment of choice is a total transabdominal hysterectomy.
Treatment of EIN
In premenopausal patients, EIN is treated with high doses of progestational agents:
- MPA 100 mg by mouth daily
- Megestrol acetate 160 mg daily by mouth
- MPA injections 1 g intramuscularly per week for 12 weeks
- Levonorgestrel intrauterine device, LNG-IUS, which avoids systemic and gastric side-effects which releases 20 μg/day, and is left in place for a period of 6 months to 2 years in this condition
Postmenopausal women with EIN should undergo total hysterectomy because of the high risk of endometrial cancer, and because 80% will not respond to progestins.
Outcomes
In 25-90% of premenopausal women with EIN, it is reversed to a secretory type of endometrium. The outcome using an LNG-IUS is generally better with EH, up to 100%, compared to 67-88% in EIN. Once this reversal is seen, a biopsy should be repeated every 6 months until the endometrium is completely normal on several visits, which cover several years. Following the appearance of secretory changes in response to progesterone, the induction of ovulation is recommended to prevent unopposed estrogenic action from recurring in the endometrium.
However, the fact remains that a hysterectomy specimen remains the only definitive mode of confirmation of the presence or absence of an invasive lesion. In such a case, a cancer could well have been undertreated by progestin therapy.
In the percentage of patients with benign EH who do not respond to progestins by cessation of abnormal bleeding, a total hysterectomy is recommended with or without removal of the fallopian tubes and ovaries.
Uterus-sparing treatment of EH
Some patients with EIN are not suitable for surgical management or have not completed their family. In such a case, studies have shown that a trial of progestin therapy could be offered for 6 months followed by repeat endometrial biopsy. If this showed persistent atypia and abnormal gland architecture, total hysterectomy is the only option.
Minimally invasive surgical techniques in EH
Several newer techniques have been described in the management of benign EH. These include:
- Ablative methods such as cryosurgery, laser ablation and electrocoagulation, which uses liquid nitrogen or other freezing gases, laser energy or heat to remove the endometrium respectively
- Hystero-resection: In this technique, the whole of the endometrium is resected, including the basal layer, under direct hysteroscopic guidance. This is the preferred method when available as it provides a complete sample of tissue for microscopic examination, ensures good control of bleeding and provides control over the depth of tissue removed.
It could be said that some patients are not suitable for conservative techniques. Risk factors which help screen out these patients include:
- Torrential hemorrhage
- Tamoxifen use with repeated bleeding
- Obesity, diabetes mellitus and postmenopausal status which are all risk factors for endometrial cancer
This decision may in future become easier with the use of new diagnostic criteria such as the histomorphometric 4-class rule, which aims to predict the presence of frankly invasive cancer at the time of hysterectomy. It usES characteristics such as epithelial cell number, epithelial thickness, and nuclear pleomorphism as observed on endometrial biopsies. While early studies indicate that it can predict or rule out a myoinvasive outcome in patients with EH, it needs to be adapted to widespread use before its usefulness can be properly gauged.
Further Reading
Last Updated: Aug 23, 2018