Cell culture is a commonly used method to study cells when in vivo study is not possible. It involves growing cells outside of the body of an animal, in controlled settings.
These settings should be similar enough to the in vivo environment to allow for proliferation. However, since they are separate from a living organism, these cells are often more exposed to environmental dangers. One of the biggest and most difficult dangers facing cell cultures are mycoplasma.
These small bacteria can infect and destroy cell lines being kept in laboratory cell cultures, therefore making study difficult.
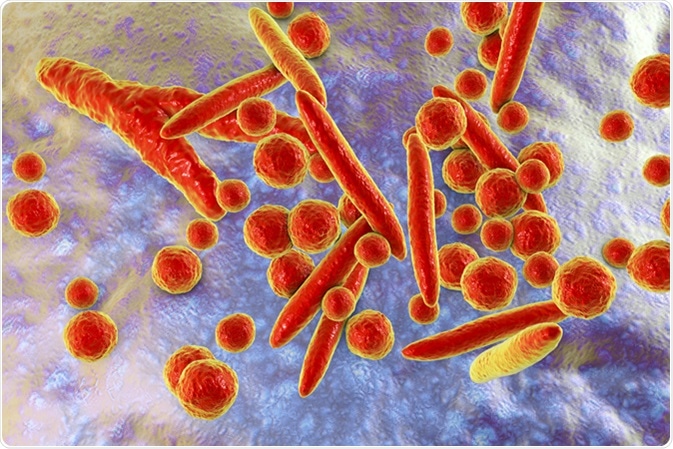
Mycoplasma bacteria, 3D illustration showing small polymorphic bacteria which cause pneumonia, genital and urinary infections. Image Credit: Kateryna Kon / Shutterstock
Discovery
Contamination of both unrelated cell lines and of bacteria pose the gravest threat to cell cultures. The original discovery of mycoplasma growth in cell cultures was in 1965. By then, cell cultures had been used for decades. This slow discovery of contamination was due to how difficult mycoplasma is to detect. Many bacterial infections cause turbidity in cell cultures which can be seen by laboratory staff. However, mycoplasma often does not exert any visible effects and can therefore not be easily detected.
Since cells in culture are isolated, they are more vulnerable to environmental disturbance. This means that they are ill equipped to stand up against bacterial infections, such as mycoplasma. In addition, mycoplasmas are commonly resistant to antibiotics because they lack a cell wall. This further complicates mycoplasma contamination, since it can be hard to eliminate if it is detected.
There are four primary sources of mycoplasma contamination in cell cultures; from original tissue isolate, culture reagents, laboratory staff, and cross contamination from already infected cultures. Contamination from original tissue is very uncommon, constituting only 1% of reported cases. The other three sources have more varied histories, with contamination shrinking as laboratories become more informed on how to prevent contamination.
Culture Serum
Bovine serum is cow-derived serum supplement often used in cell cultures. Fetal and newborn bovine serum are the more commonly contaminated reagents used in culture growth. Serums are often cleansed by passing them through filter membranes. This clears out larger objects, but given the small size and lack of membrane, mycoplasma can pass through these filters and remain in the finished serum product.
In the 70s, rates of mycoplasma-contaminated bovine serum provided by manufacturers were as high as 25-40%. Since then, manufacturers have made great steps in reducing cases of mycoplasma contamination, however, mycoplasma-free culture reagents can still not be guaranteed.
Laboratory Staff
The largest percentage of mycoplasmas found in contaminated cell cultures are from human sources. The most common mycoplasma species spread from humans to cell cultures are M. orale, M. fermentans and M. hominis. In humans these are found in the oropharyngeal tract.
Experiments have shown that laboratory staff are a formidable source of mycoplasma contamination. A study showed that 80% of staff were carriers of mycoplasma. The spread occurred through sneezing and talking, as well as by dirty clothes. Similarly, working without gloves proved to facilitate the spread of mycoplasma. Improperly cleaned laboratory equipment or previously used reagents can also spread mycoplasma. Therefore, many laboratories keep their cell cultures in spaces were only authorized, trained personnel are allowed.
Cross Contamination
Contamination from one cell culture to another is very common. Most laboratories with one cell culture infected will have most or all other cultures also become infected by the same species. Thus, the infected cell cultures themselves are the biggest source of contamination for other surrounding cultures. This is due to droplet generation when cultures are handled, the high mycoplasma concentration in infected cultures, and extended survival of mycoplasma when they are dried.
Contamination from one culture to another occurs mainly through particles in the air, which are made airborne during handling. The laboratory air should be draft-free, to ensure that the airborne particles settle. However, once someone enters, these particles are disturbed and can once again be carried by the air through the room.
Further Reading
Last Updated: Aug 23, 2018