Osteoclasts are specialized, multinucleated cells that play a vital role in bone development and regeneration.
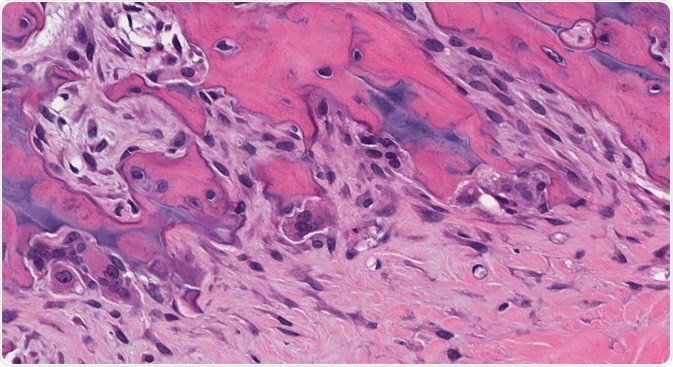 Credit: vetpathologist/Shutterstock.com
Credit: vetpathologist/Shutterstock.com
The skeleton is an essential part of the vertebrate body. It provides support for organs and the overall integrity of the entire organic system, allowing for movement and other functions of a healthy organism.
Bones are constantly remodeled over the lifetime of an organism, due to factors such as response to stress, damage, and the need for constant regulation of calcium content. There are specific mechanisms in place to carry out this function. Two specialized types of cells are responsible for the synchronized process of bone remodeling: Osteoblasts (bone-forming cells) and osteoclasts.
What are osteoclasts?
Osteoclasts are large multinucleated cells with a myeloid lineage, which have the function of clearing away mineralized and calcified constituents of the bone matrix which are aged or damaged. They have 2-12 nuclei (typically 5) and are 150-200µm in diameter. They are strongly acid-phosphatase-positive.
There are two distinct features of an osteoclast: a ruffled border and a sealing zone. The ruffled border is composed of a convoluted membrane that develops by the merging of secretory lysosomes with the plasma membrane. The sealing zone contains an actin filament ring which surrounds the ruffled border, isolating the acidified microenvironment inside the cell from the general extracellular space.
Osteoclasts have several functions. They indirectly respond to calcium-regulating hormones such as parathyroid hormone and incorporate growth factors such as IGF-1 (insulin-like growth factor-1) into the bone matrix, which affects the coupling of bone resorption to bone formation (this also potentially targets other cells such as metastatic tumors.) Finally, osteoclasts retain features of other myeloid cells, including cytokine production and antigen regulation. This ability gives osteoclasts the potential to affect the immune response to several conditions.
Osteoclast formation and differentiation
Osteoclasts originate from hematopoietic stem cells (HSC), which are contained in the bone marrow. These are the same stem cells which produce all other types of blood cell, including red blood cells and the mononuclear phagocyte system from which osteoclasts arise. They are formed under the presence of macrophage colony-stimulating factor and the receptor activator of the NF-KB ligand.
A common myeloid progenitor cell is produced from the HSC, which differentiates into granulocyte/macrophage progenitor under the influence of granulocyte/macrophage colony-stimulating factor.
Whilst studies have made it clear that HSCs are osteoclast precursors, the initial steps in lineage development are not fully understood. The earliest precursor that can be isolated and manipulated in vitro is the bone marrow macrophage or its splenic counterpart. Incompletely understood signaling pathways are involved in the formation of osteoclasts and differentiation from other types of macrophage.
Function in bone resorption
There are a few factors that initiate the process of bone resorption. The main determining factor is the body’s calcium level. When the blood calcium levels decrease, the parathyroid gland (located in the neck) initiates the secretion of parathyroid hormone (PTH.) PTH accelerated the resorption process to replenish the blood’s calcium levels. Other initiating factors include conditions such as psoriatic arthritis, disuse, lack of stimuli, and old age.
The bone resorption process begins with the polarization of osteoclasts, which leads to the formation of the bone-apposed ruffled membrane. The osteoclast then attaches itself to the surface of the bone, with the sealing zone forming an isolated microenvironment.
The ruffled membrane then secretes hydrochloric acid to dissolve the bone material, and the demineralized bone matrix is broken down by enzymes cathepsin K and matrix metalloprotease. Calcium and phosphate are produced in this process, and they find their way into the blood.
In order to regulate this process, the parathyroid gland reduces the amount of parathyroid hormone when it detects that the calcium levels in the blood are too high, leading to the inactivation of osteoclasts.
Pathological conditions
Healthy bone remodeling involves firmly coupling resorption to formation to ensure correct maintenance of bone mass and quality. When this coupling process is perturbed, or osteoclast function is dysregulated, several degenerative bone conditions can occur.
These include:
- Osteoporosis – This is the most common pathological condition which affects healthy bone material regulation. It is characterized by an abnormal increase in osteoclast activity. It leads to decreased bone material integrity, which leads to more common fractures. It is most commonly caused by aging, but factors such as hormonal imbalance and reduction of estrogen in post-menopausal women can also increase osteoclast activity.
- Paget’s disease – This is a deforming bone disorder characterized by an increase in osteoclast number and size. It leads to localized bone destruction and compensatory activity by osteoblasts. Mutations in genes responsible for regulating osteoclast production are the cause of this condition.
- Rheumatoid arthritis – Activation of pathological osteoclasts in the late stages of the disease results in painful and erosive lesions.
Summary
In a healthy organism, osteoclast activity is regulated in an efficient manner after being produced by hematopoietic stem cells, which comes about via processes that are still not fully understood. Abnormal regulation due to conditions such as disease, aging, and hormonal imbalance can lead to various degenerative conditions. Understanding the process of osteoclast formation and regulation is crucial to the effective treatment of these conditions.
Osteoblasts and Osteoclasts
Sources:
-
Feng, X and Teitelbaum, S.L (2013) Osteoclasts: New Insights Bone Research 1 pgs. 11-26. https://www.nature.com/articles/boneres20133.pdf?origin=ppub
-
Novack, D.V and Mbalaviele, G (2015) Osteoclasts, key players in skeletal health and disease Microbiol Spectr. Vol. 4 Issue 3 https://www.ncbi.nlm.nih.gov/pubmed/27337470
-
Henricksen, K et al. (2011) Osteoclast activity and subtypes as a function of physiology and pathology - implications for future treatments of osteoporosis Endocr Rev. Vol. 32 Issue 1 pgs. 31-63 https://www.ncbi.nlm.nih.gov/pubmed/20851921
-
Rubin J., Greenfield E.M. (2005) Osteoclast: Origin and Differentiation. In: Bronner F., Farach-Carson M.C., Rubin J. (eds) Bone Resorption. Topics in Bone Biology, vol 2. Springer, London https://doi.org/10.1007/1-84628-016-8_1
Further Reading
Last Updated: Nov 27, 2019