Nov 21 2017
People with potentially fatal chronic lung diseases are not in control of their condition,new research by Chiesi reveals today. This could be leading to costly A&E visits and hospital stays which may be dramatically reduced if they were being treated adequately.
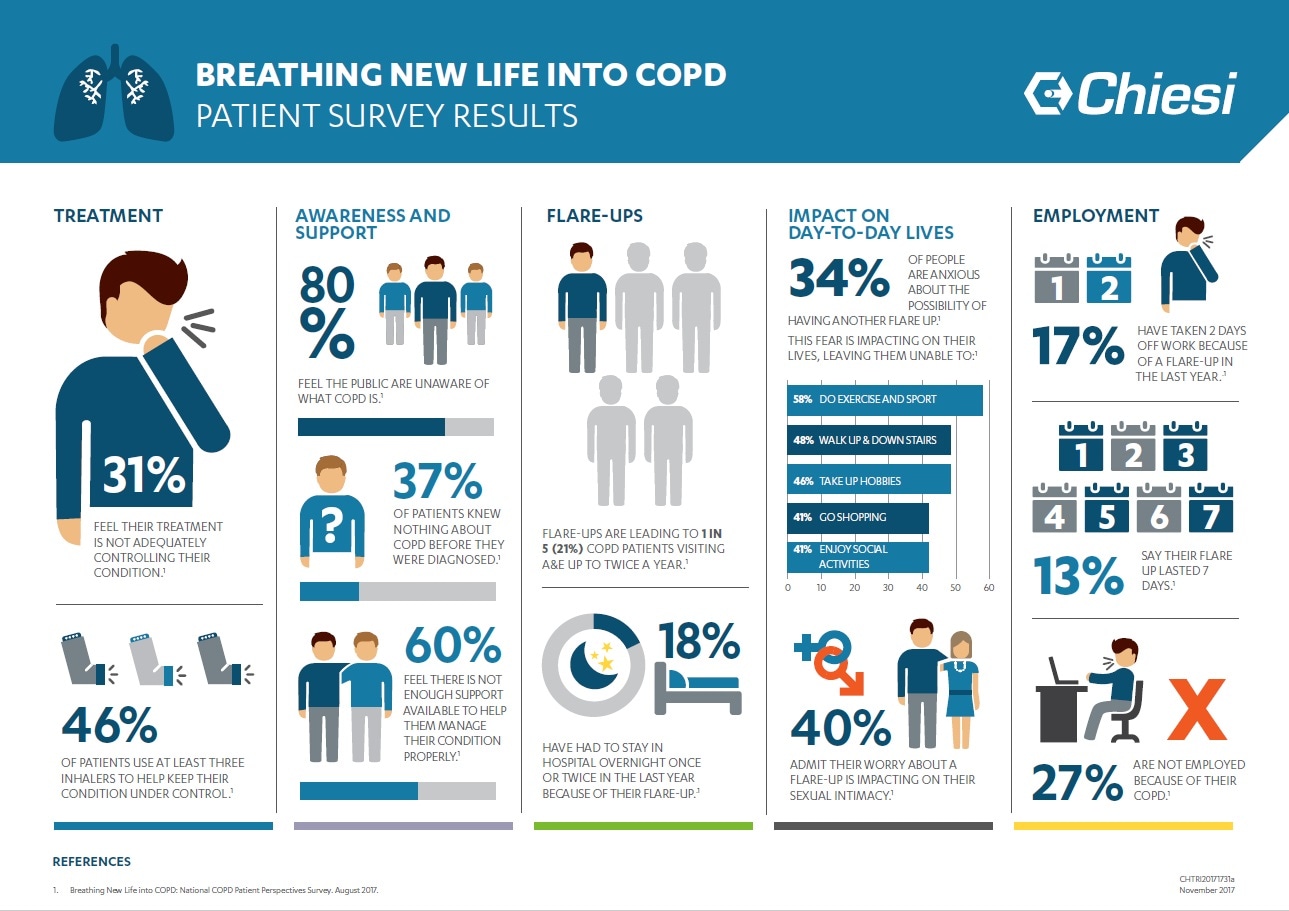
The‘Breathing New Life into COPD’ survey of 500 people across Britain diagnosed with chronic obstructive pulmonary disease (COPD) - the collective term for conditions such as chronic bronchitis and emphysema – found that almost a third (31 per cent) feel their treatment was not adequately controlling their condition.60 per cent feel there is not enough support available to help them manage it properly.
This is despite the nationwide survey revealing that almost half (46 per cent) of patients use at least three inhalers to help keep their condition under control.Yet they are still being struck by flare-ups where their condition suddenly worsens, making breathing even more difficult than usual.These flare-ups can be caused by an infection such as a cold or for an unknown reason.
According to the survey, carried out by Opinion Health on behalf of the pharmaceutical company Chiesi in August 2017, flare-ups are leading to one in five (21 per cent) COPD patients visiting A&E up to twice a year. Some patients (4 per cent/18 patients) have rushed to the emergency department three or more times in a year because of a flare-up. And 18 per cent of those questioned have had to stay in hospital overnight once or twice in the last year because of their flare-up. A single visit to A&E can cost £124 just to be seen, whilst an NHS hospital stay is estimated to be£400 a day. COPD accounts for over 140,000 hospital admissions and over a million bed days each year across the UK, which is 1.7 per cent of all hospital admissions and bed days. 97 per cent of these admissions are for emergency care.
Dr Richard Russell, consultant respiratory physician at Southern Health NHS Foundation Trust and Clinical Director of the West Hampshire Integrated Respiratory Service said:
This is an important and large survey of 500 UK patients with COPD. The findings demonstrate there is much more to be done to improve the care of these patients. We are often treating patients with three or more inhalers and yet the results of this survey show that 17 per cent of patients have not had their inhaler technique checked by their doctor. Patients are still suffering from poorly controlled disease, especially from acute lung attacks or exacerbations, which is impacting on all aspects of their lives and leading to significant mortality, morbidity and cost to society.
COPD is an incurable condition because it causes permanent lung damage.It affects at least 1.2 million people in the UK, usually over the age of 40. Experts believe there are also more than two million undiagnosed cases. The condition kills over 30,000 people each year and is estimated to cost the NHS more than £800m a year and the overall economy some £3.8bn in lost productivity. The main cause is smoking, but it can also be caused by workplace exposure, genetic make-up and general environmental pollution.
The survey also revealed a lack of awareness of the condition, with 37 per cent of patients knowing nothing about it before they were diagnosed. massive 80 per cent of sufferers felt the public are unaware of what COPD is and how it can impact patients’ lives.
Impact on day-to-day lives
COPD is also having a negative impact on the personal lives of sufferers.The survey found that 34 per cent are anxious about the possibility of having another flare up.1 This fear is impacting on their day-to-day lives, leaving them unable to:
- do exercise and sport (58 per cent),
- walk up and down stairs (48 per cent),
- take up hobbies (46 per cent),
- go shopping (41 per cent)
- enjoy social activities (41 per cent).
Almost 40% admit their worry about a potential flare-up is impacting on their sexual intimacy.
17 percent admit that they had to take 2 days off work because of a flare up in the last year and 13 percent say their flare up lasted 7 days. It is then no surprise that 27 percent of those questioned were not employed because of their COPD.
Dr Penny Woods, Chief Executive of the British Lung Foundation said:
It’s vital that healthcare professionals are supporting patients by helping them to effectively manage their condition at home. Providing patients with information about treatments, services, and support beyond the clinic or hospital will play a big part in helping them to adapt to their condition, and, will ultimately reduce pressure on already stretched hospital services.