The Centers for Disease Control and Prevention (CDC) has released fresh clinical recommendations for health care personnel for treatment of children suffering from concussion or mild traumatic brain injury (mTBI).
The recommendations titled “CDC Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children,” was released today in the latest issue of the JAMA Pediatrics. Pediatric concussion management experience from 25 years has been collated in this new guideline to determine the best possible way to deal with mTBI in children.
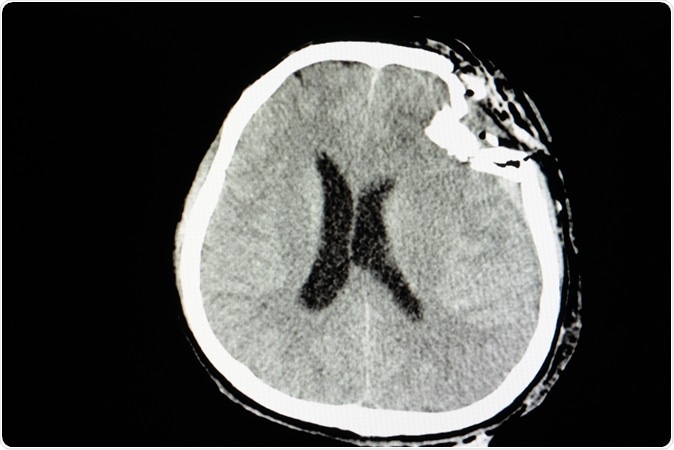
CT skull film of a patient with traumatic brain injury showing compression depression fractures of left temporoparietal bone. Image Credit: Sopone / Shutterstock
Deb Houry, MD, MPH, director of CDC’s National Center for Injury Prevention and Control in a statement said, “More than 800,000 children seek care for TBI in U.S. emergency departments each year, and until today, there was no evidence-based guideline in the United States on pediatric mTBI—inclusive of all causes. Healthcare providers will now be equipped with the knowledge and tools they need to ensure the best outcomes for their young patients who sustain an mTBI.”
The clinical guidelines outline 19 recommendations that include the optimized ways to diagnose, manage and treat mTBI in children and also helps predict the possible outcomes of such events. It is to be applied in all healthcare settings. CDC Pediatric mTBI Guideline provides a specific protocol in management of these cases.
The main changes in the guidelines from previous recommendations include;
- All pediatric patients with mTBI do not require routine imaging studies
- Validated, age appropriate symptom scales and scoring systems are to be used to diagnose an mTBI
- Other risk factors that mean prolonged recovery time should be assessed. This includes other brain injuries in the past, history of mTBI, severe symptom score immediately after the injury, learning difficulties and other characteristics in the child, family factors such as family stressors or social factors etc.
- Patients and their parents or caregivers are to be provided with instructions when they return to their daily activities according to their symptom scores and severity.
- Parents and caregivers are to return gradually to their non-sports activities after 2 to 3 days of rest.
Houry explained that there was a need for a standard guidelines that would be “consistent, current, and evidence-based” and could help healthcare providers in diagnosis and management of mTBI. This guideline is an answer she said. Houry said the guideline is also directed towards “supporting families, sports coaches, and schools—who are all integral to keeping children safe and healthy.” She added, “The hope is that this Guideline will lead to future studies and guidelines that further advance the care of patients of all ages with mTBI and other serious brain injuries.” In addition to the guidelines are supporting tools and materials that can help screen patients for discharge and plan their recovery. The tools are available at www.cdc.gov/HEADSUP.
The new guidelines were lauded by Michael McCrea, a professor of neurosurgery and neurology at the Medical College of Wisconsin, and Dr. Geoff Manley, vice chairman of neurological surgery at the University of California, San Francisco in an accompanying editorial. The write, “We applaud the CDC guideline's recommendation for clinicians to counsel children and their parents as to the known acute effects of injury, expected course of recovery, and factors that may positively or negatively affect recovery and outcome after mTBI.” Next major challenge they add is adoption of these guidelines by doctors on the frontlines treating patients. Yet, they write, this is a “solid step toward achieving this comprehensive, personalized approach to state-of-the art care.”