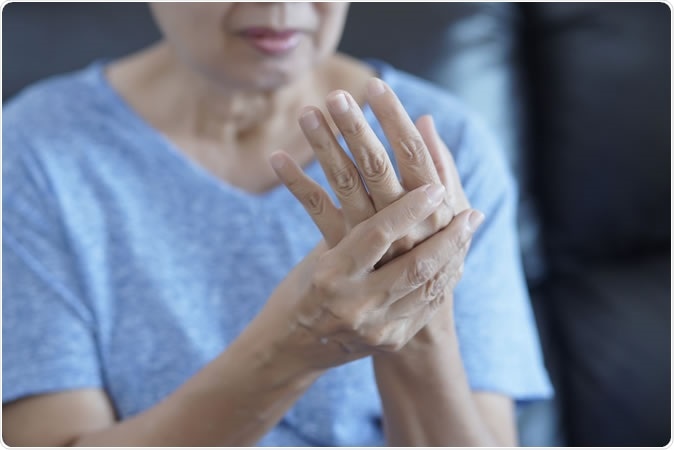
No studies have assessed the effect of methotrexate (MTX) in osteoarthritis of the hand (HOA). The purpose of this study was to examine the effect of MTX on pain and structural progression in symptomatic erosive HOA (EHOA). - Image Credit: one photo / Shutterstock
Osteoarthritis is a common disease of the joints that is found to affect middle-aged or elderly patients, as a result of age-related degeneration of the smooth cartilage that covers the ends of the bones involved in mobile or synovial joints, throughout the body. This is accompanied by changes in the bones themselves, such as bony spurs; tendon and ligament weakening, leading to reduced joint support; and inflammation of the smooth synovial membrane that lines the inside of the joint, and produces the lubricating fluid called synovial fluid that facilitates the movement of the bone over each other.
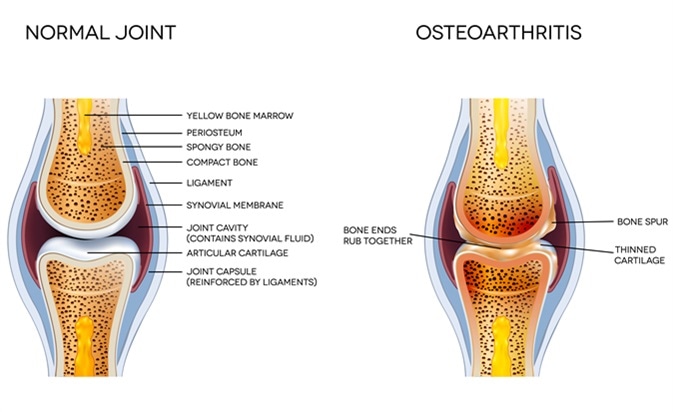
Osteoarthritis and normal joint anatomy. Image Credit: Tefi / Shutterstock
Treatment of this condition depends on the symptoms and severity of the disease, as well as the degree to which it affects the functioning of the patient. Pain-relieving and anti-inflammatory drugs are used.
So far, no effective treatment has been identified in terms of arresting joint damage in hand OA. In fact, the disease progresses in phases, with alternations of erosion and remodeling. According to researcher Christian Roux, “These rearrangements suggest the involvement of pro-inflammatory cytokine cascades known to cause cartilage degradation and bone resorption. “
He also points out that advanced imaging technology has made it possible to visualize the presence of inflammation at these joints in hand OA. Thus, both signs and symptoms point to the involvement of an inflammatory process in these joints, more similar to rheumatoid or psoriatic arthritis than to classical OA.
For some physicians, this has triggered the trial of disease modifying anti-rheumatic drugs (DMARDs) like methotrexate in hand OA. These drugs are used in autoimmune inflammatory arthritic conditions such as rheumatoid arthritis. They alter the course of the disease by regulating immune system overactivity. Though methotrexate is quite frequently used in such conditions, its activity in hand OA has not been systematically studied.
The present study was conducted over a year, in a randomized double-blinded design. It was a prospective trial carried out in one hospital. The aim was to find out how methotrexate affects pain and joint structure damage in patients who have hand OA producing severe symptoms, and X-ray evidence of bone breakdown, or joint erosion.
The trial was carried out in 64 patients with erosive hand OA. They were randomly assigned into 2 groups, one taking 10 mg methotrexate weekly and the other a placebo.
The researchers wanted to measure pain at 3 months. in addition, they also looked at the clinical signs and symptoms: pain assessed on a Visual Analog Scale (VAS), radiographic features, and magnetic resonance imaging (MRI) at 12 months.
The findings
At 3 months, both groups had equivalent amounts of pain as measured by the VAS, though in absolute terms there was a mean decrease of 17.5 points from the previous mean of 28.4 for the methotrexate group, and of 8.4 points from the previous 25 points in the placebo group. In other words, symptomatic improvement was modest and equivalent in both groups.
The difference was seen on imaging. Joint erosions changed to a remodeling phase in significantly more joints in the methotrexate group compared to the placebo group, at 27% to 15% respectively. joints in which the joint space already appeared to be narrowed, due to cartilage loss, showed significantly less erosion in the methotrexate group compared to the placebo group – 8% vs 29%.
These patients could be identified to be at higher chance of better erosion control by measuring baseline IL-6 levels and evaluating the degree of synovial inflammation, before beginning methotrexate.
To sum up: methotrexate did not show short-term control of pain and joint function at 3 months, nor later at 12 months, but did bring down the rate at which joint damage progresses, and apparently facilitates bone remodeling. The presence of inflammation as assessed by markers like IL-6 and synovitis in erosive hand OA may account for the failure to relieve pain, and predicts the risk of further joint damage.
Implications
Roux says, “It is possible that we have to treat earlier if we want to have an effect on pain. However, our results show a structural effect of the treatment that facilitates bone remodeling and seems to slow the erosive structural progression of digital osteoarthritis with a seemingly more pronounced effect in patients with early lesions.” He points out that for most people, the deformity produced by the hand OA is the prominent issue, and early treatment may prevent this. More research is called for to confirm the results of this study and determine appropriate treatment protocols.
Journal reference:
Ferrero S, Wittoek R, Allado E, Cruzel C, Breuil V, Euller Ziegler L, louille D, Roux C, and Kremer J. Methotrexate in patients with hand erosive osteoarthritis refractory to usual treatments: a randomized, double-blind, placebo-controlled trial [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/methotrexate-in-patients-with-hand-erosive-osteoarthritis-refractory-to-usual-treatments-a-randomized-double-blind-placebo-controlled-trial/. Accessed November 11, 2019.