Rotavirus infection is thought to be a risk factor for type 1 diabetes mellitus (T1DM). The role played by live attenuated rotavirus vaccination in the risk of this condition in children is, therefore, an area of active research. A new study published in the journal JAMA Pediatrics in March 2020 debunks this concern.
T1DM is an autoimmune condition with a genetic predisposition. In mouse experiments, rotavirus infection was shown to speed up the development of T1DM, with a marked antirotavirus antibody response among the vulnerable mice. Islet cell autoantibodies have also been found to increase. Some scientists have found a link between gut infection and T1DM in children up to 10 years old.
Two different types of vaccines have been licensed in the US. Earlier researchers have shown that this vaccine reduces the incidence of T1DM. The current study was aimed at finding out where these variables are associated.
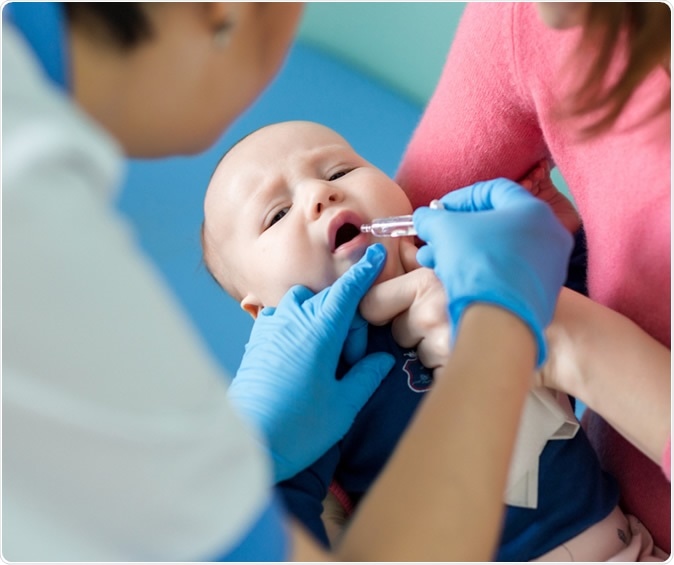
Oral vaccination against rotavirus infection. Image Credit: Gorlov-KV / Shutterstock
The study
The researchers examined almost 390 000 children in a retrospective study design. All the children were born between January 1, 2006, and December 31, 2014. The study was performed in 7 US healthcare organizations belonging to the Vaccine Safety Datalink, which uses electronic health record databases to examine the safety of different mice.
The rotavirus vaccination was given to all children between the age of 2 to 8 months. Boys and girls were equally represented.
The children were divided into three exposure groups. In essence, those who were fully immunized by eight months of age, those who were partially vaccinated by this age (received some but not all recommended doses), and the third were not exposed to rotavirus vaccination (received any doses of rotavirus vaccine).
The results
About 93%, 4%, and 3% were entirely, partially, and nonexposed to rotavirus immunization by eight months of age. The median period of follow-up was 5.4 years.
Rotavirus vaccination was associated with a 31% to 55% reduction in acute gastroenteritis, leading to hospital admission over the years 2008 to 2013, saving about $1.2 billion to the healthcare system. This would suggest the advisability of continuing to administer rotavirus vaccination to infants.
The incidence of type 1 diabetes mellitus among children aged eight months to 11 years, as identified by the International Classification of Diseases codes, was approximately 21/100 000 person-years. There were 464 cases in the total cohort. These children were aged 4.4 years at diagnosis, on average.
When analyzed by the group, the risk was virtually unchanged for children who were fully immunized, but it was 50% higher for children who were partially exposed. However, the full confidence limits rouse uncertainty as to the significance of these outcomes. The researchers found no significant risk for T1DM with the use of the vaccine.
The study was limited by the lack of follow up to the age of 14 years, which is the peak time for T1 DM to manifest. Secondly, the unexposed cohort was only about 3% of the whole group. It is estimated that the study was powered only for the detection of relative risk above 2.1.
Thirdly, some of the nonexposed cohort could have been vaccinated outside the vaccine safety department, leading to misclassification of these children. This could have shifted the result towards the zero point.
Implications
The lack of a significant association between rotavirus vaccination and the risk of type 1 diabetes contrasts with the findings of earlier studies, such as those carried out in Finland, in Australia, and a medical claims data-based study. These showed an inverse association between rotavirus vaccination and T1 DM in children.
The current study is far longer in follow-up duration, and the scientists also compensated for potentially confounding factors like race, gestational age at birth, birth weight, family history of T1 DM, and breastfeeding. No significant links were found between rotavirus vaccination and the detection of new cases of this condition in children, however.
The researchers conclude, “Our findings do not show an association between rotavirus vaccination and type 1 diabetes in children. Although rotavirus vaccination may not prevent type 1 diabetes, these results should provide additional reassurance to the public that rotavirus vaccination can be safely administered to infants.” They call for more research with more significant numbers of patients and enough time to detect this risk, if present.
Journal reference:
Glanz JM, Clarke CL, Xu S, et al. Association Between Rotavirus Vaccination and Type 1 Diabetes in Children. JAMA Pediatr. Published online March 09, 2020. doi:10.1001/jamapediatrics.2019.6324