Every year about 15 million babies are born preterm, and 1 in 15 die before their first birthday. But this is not the whole picture. The truth is that inequity looms large in healthcare. About half of all babies born at or before 32 weeks die in primitive settings in sharp contrast to an almost 100% survival rate in more advanced countries.
The new device
The sensors were developed last year and tested in Chicago, on newborns in two hospitals. They are now undergoing testing in 42 newborn babies in Kenya, alongside the best conventional monitoring systems, so they can find out exactly where they stand in terms of performance standards. They are also being tested in pregnant mothers in Zambia, with Ghana and India additionally on the testing list. The new platform harnesses the power of batteries and sensing technology to monitor a whole range of infant behavior and signals. These include vital signs, of course, but also crying, movement, body habitus, and heart sounds. The sensors are soft and flexible, minimizing damage to the newborn's skin. The wireless design means it is capable of increased contact with the skin of the patient without being plucked off.
The technology is thus far safer and reliable for use in premature babies. It can also monitor the health of the fetus during preterm labor to make sure that the baby is born healthy and safe while reducing the odds of unnecessary intervention that could jeopardize the life of the mother. Keeping tabs on the health of those babies and mothers, which are at high risk for an unfavorable outcome could potentially help intervene on time, before the onset of serious illness.
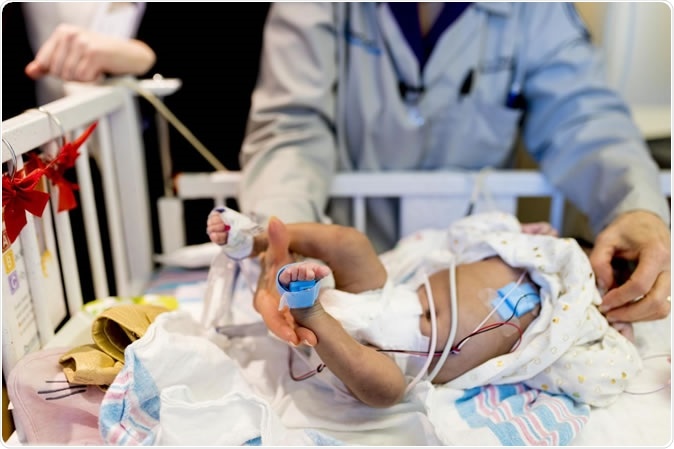
A neonate at Prentice Women's Hospital in Chicago wears the wireless sensors (in blue) alongside traditional, wired sensors so the researchers can test and evaluate the sensors side-by-side. Image Credit: Northwestern University
The concept
The researchers led by Northwestern's John A. Rogers had already studied the performance of a pair of wireless flexible sensors on premature babies, proving them to be dependable and accurate, just like the more cumbersome devices currently used that don't allow parents to bond with their infants and to cuddle or hold them fearlessly.
However, to adapt them to resource-poor settings, they then added in a slim battery for power, one that could be recharged, so that the device would always be able to operate in rural settings. It was also important that the range of wireless operation be improved. In addition, the team incorporated more sensors to detect infant crying, movement, and heart sounds.
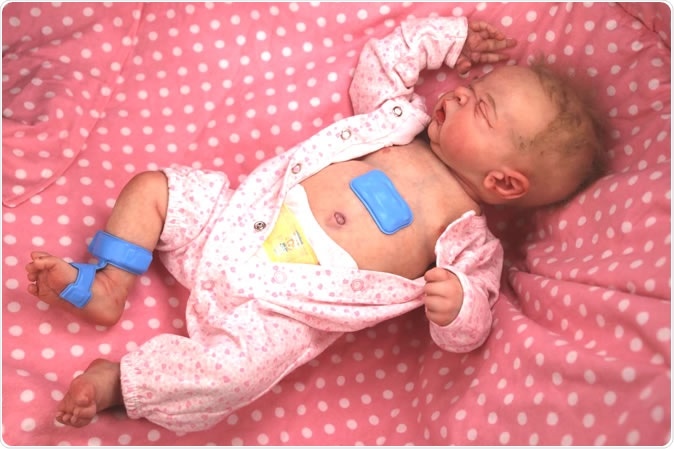
The wireless sensors (in blue) displayed on a model neonate in the lab. Image Credit: Northwestern University
The constant pressure was to develop the most practical, clinically valuable, and easy to use. Explains Rogers, "We couldn't just drop our existing technology into other countries and different settings without taking their specific needs into account. We knew that we needed to build the foundations for highly robust, reusable devices, applicable in regions with limited facilities and resources."
The current project is based on the use of bio-integrated electronics and is all about making healthcare more equitable, in part, at least. In the words of researcher John A. Rogers, "We designed our technology to offer affordable, clinical-grade monitoring capabilities for use anywhere in the world -- from the hospital to the home to the field. Using advanced concepts in soft electronics, we achieved devices that are safe, easy to use, and patient-centric."
The scientist emphasizes that one of the focus points in their research was to make sure the device could be used in "low-resource settings in the developing world, where this type of technology has the greatest potential to improve and possibly save lives."
Co-researcher Debra Weese-Mayer goes on to explain that their labor was not about making things more convenient and technologically advanced. Instead, their aim was health-centered; they wanted to incorporate the sensor parameters and sensing variables that would make more sense in terms of the baby's health and stable device performance.
Sensors to displays
The devices are designed with sensors that send data to mobile devices or to nurses' station displays, via radiofrequency. This means that neither accuracy nor simplicity of operation is compromised. Xu comments that its accuracy may be comparable to that of the most sophisticated hospital systems in current use. In his words, "You don't need expensive equipment that requires a specialized bioengineer and IT department to install. You pull out your mobile device, connect to our sensors, and you're taking care of patients."
The plan involves testing the sensors on 15,000 pregnant women and 500 newborns by the middle of 2021, in what Xu describes as "a collaborative team effort," to deal with actual problems. Some instances are limited power availability, daily blackouts, and poor access to the internet.
To address these, the scientists focused on cost and practicability. They listened to doctors and other health team members, to find out what they actually wanted, and then designed a solution that actually solves the everyday problems of health professionals in developing countries, in what researcher Shiai Xu describes as an "incredibly rewarding" experience and a "bi-directional information flow."
For instance, when early sensors were thought to be too large for the thin and tiny chest of a newborn baby, the researchers instantly changed tracks to come out with a smaller and slimmer version that won the favor of the nurses.
Again, nurses initially found it challenging to ensure that the foot component of the chest-foot sensor pair was in perfect alignment, which is necessary for data accuracy. Rogers describes the innovative response: "We designed a system that lights up as red, yellow or green -- incorrect, close or in the right place -- depending on the accuracy of the alignment, to provide feedback to the caregiver."
And the result has been awe-inspiring. Rogers says, "These latest platforms are giving us great data. When we put the sensor on the baby, it starts working immediately, in nearly any setting or location."
And parents love the system too because it allows kangaroo care, or skin-to-skin interaction, which enhances physical bonding, better sleep, and lower stress.
The future – AI-enabled devices
The researchers have started up Sibei Health, aiming at FDA approval for the device in terms of improving the health of the fetus and newborn, as well as the mother. It is now in partnership with Drager, a prominent medical technology firm that specializes in lifesaving products. The next step will be to integrate artificial intelligence (AI) into the sensors to glean patterns and explanations from the data a well as to help health professionals decide on their course of action.
These devices yield a fantastic amount of data - half a gigabyte per day per patient. The AI will help to milk this data to the maximum. Xu says, "We'd like to use clinically validated algorithms that could, for example, tell us if a baby is likely to develop sepsis within the next 24 hours based on their vital signals. Then we could have ventilators and antibiotics ready to escalate care almost proactively. For pregnant women, we're working to identify danger signals in low-resource settings more quickly."
The researchers are optimistic that these sensors could be in use in US hospitals in the next year. Also, the team looks forward to the appearance of these sensors in hospitals around the world, hoping to send out more as part of the strategy to achieve cost-effective monitoring in health care.
The researchers sum up: "We believe that our technology could significantly enhance the quality of neonatal care around the world. We think in terms of a 'NICU of the future,' available anywhere. (Rogers). "Xu adds, "We want to see these sensors in every country, monitoring the first heartbeat to the last in our most vulnerable patients."
Journal reference:
Chung, H.U., Rwei, A.Y., Hourlier-Fargette, A. et al. Skin-interfaced biosensors for advanced wireless physiological monitoring in neonatal and pediatric intensive-care units. Nat Med 26, 418–429 (2020). https://doi.org/10.1038/s41591-020-0792-9