Scientists around the world are racing to study the novel coronavirus strain severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Now, it appears that there are eight strains of SARS-CoV-2 circulating the globe. The good news is that according to infectious disease physician and clinical microbiologist Charles Chiu, “The virus mutates so slowly that the virus strains are fundamentally very similar to each other.”
Using advanced technology to rapidly sequence the virus from test samples, the researchers show that there are only very minute differences between the different strains, and none of them enhances viral virulence. Moreover, say the scientists, no strains are becoming more dangerous with continuing mutational change.
Scientists studying the virus have shared their knowledge to compile a genetic sequence map at NextStrain.org, an open-access website that shows how the various strains have traveled to different regions and countries. This finding is based on over 2,000 sequences of the viral genome that have been shared with the researchers so far. Samples have come in from all continents except Antarctica.
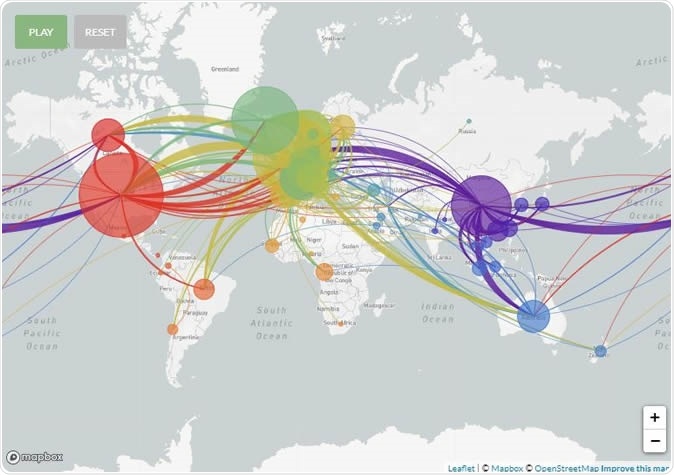
Genomic epidemiology of novel coronavirus. Image Credit: Nextstrain
Referring to the transmission of the virus as trackable, Chiu also says, “We have the ability to do genomic sequencing almost in real-time to see what strains or lineages are circulating.”
Why is genetic tracking important?
The disease is asymptomatic or mild in up to 80% of people but causes pneumonia, respiratory failure, and death in up to 5% to 6% of cases overall if not treated. If the virus were to mutate, on the other hand, and become more lethal, it would make it all the more difficult for researchers to develop an effective vaccine based on viral antigens.
For instance, the seasonal flu has a vaccine – but it has to be updated every single year because of the many and rapid mutations that have led to the emergence of several different strains of the influenza virus. Each year, the scientists must decipher which of these strains are floating around most commonly and ensure the vaccine contains those strains.
In contrast, viruses such as varicella and measles viruses mutate slowly, and hence immunizing shots against them offer immunity for many years, perhaps lifelong. In this single respect, the SARS-CoV-2 appears to be more like them than like the flu virus. Even though the study shows that the virus is mutating only once every 15 days or so, the mutations are “completely benign and useful as a puzzle piece to uncover how the virus is spreading,” according to NextStrain founder Trevor Bedford.
Is the coronavirus mutating?
The first step in genetic research of SARS-CoV-2 was taken by China when geneticists first brought out the sequence of the viral genome. This information, says researcher Peter Thielen, shows a closer similarity with the behavior of varicella and measles. Moreover, the early availability of the viral genetic sequence helped with the work of vaccine development.
At present, says Thielen, they are exploring whether the virus genome is changing from that initially published genome, and how rapidly this process is occurring. The experiments being carried out so far focus on the mutations and have helped them arrive at a tentative mutation rate. Moreover, it will help tell how well lockdown measures are working to contain the viral spread, as the type of virus being transmitted will be obvious on genetic sequencing.
If there is widespread community transmission within a region, it will show that lockdown orders have been breached routinely. On the other hand, a significant reduction in transmission would allow the lockdown to be eased.
The report, published online on March 27, is in the form of a genetic tracking map based on this data.
The findings
The study showed that the virus first reached the UK from Wuhan, China, traveling to Singapore and South Korea. The next step was to spread via flight passengers to London. From there, the large city airport was the hub from where the virus spread to the rest of Europe and the USA.
At present, say the scientists, there is still “strong mixing of samples across Europe, suggesting that the virus has continued to move across borders in the last 3-5 weeks.” Once the lockdown measures begin to show more effect, say the investigators, the outcome will be clusters of transmission of each type or strain of the virus in different countries.
In the US, however, the viral samples from opposite sides of the country are almost identical. For instance, in the state of Washington, the virus has been introduced two times, and perhaps more. The origin is thought to either be China or Europe. The effect is visible as two separate chains of viral spread.
However, in California and several other states, the virus is seen to be probably spreading within the community rather than being introduced from outside, say the scientists. This is because many of the cases on the West Coast are very similar to a Washington strain, which in turn is only three mutations away from the first strain of the virus to be found, say the investigators.
In central and South America, the pattern is not clear as only a few samples have been taken. The new sequences already received have been incorporated into the map, but the viral activity could be more intense than shown.
When it comes to Asia, the researchers insist that it looks like some cases came from Iran recently.
In Africa, the genetic tracking suggests that the virus is being transmitted locally within Kinshasa, a large city in the Democratic Republic of the Congo, for over 11 days now. Here too, the number of samples is low, and the picture showing little COVID-19 activity is likely to be misleading.
In Oceania, local viral spread is occurring in New South Wales, Australia, according to the study.
What does this mean?
Based on these studies, says Thielen, they have come to the preliminary conclusion that “this would likely be a single vaccine rather than one that needs to be updated each year, like the flu shot.” The first vaccine will likely be available all over the world in a year or 18 months.
Cautions Kristian Anderson, who also researches the pattern of transmission, “We have half a million described cases right now but maybe 1,000 genomes sequenced. So there are a lot of lineages we’re missing.”