Several zoonotic outbreaks have distressed the human population over the past few decades, including the severe acute respiratory syndrome (SARS), and the Middle East Respiratory Syndrome (MERS). The current COVID-19 pandemic began in December 2019, and presents as a pneumonic illness with initial symptoms resembling a cold, but often causing overt and acute respiratory failure. The overall death rate is still unknown but is relatively high among immunocompromised and older adults.
SARS-CoV-2 is a betacoronavirus with a large genome that shares 88% identity with the bat coronavirus. It has a trimeric spike protein on the surface, which has numerous glucose residues. The spike or S protein is responsible for the entry of the virus into the host cell.
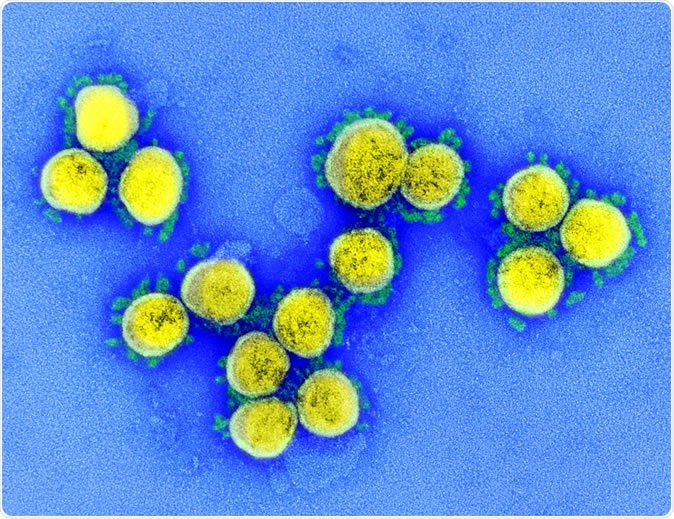
SARS-CoV-2 - Transmission electron micrograph of SARS-CoV-2 virus particles, isolated from a patient. Image captured and color-enhanced at the NIAID Integrated Research Facility (IRF) in Fort Detrick, Maryland. Credit: NIAID
The Spike Protein
The S protein is a large glycoprotein that spans the membrane, synthesized initially as a single protein. It is then subjected to proteolysis by the proteases on the host cell, yielding an S1 and S2 subunit.
The S protein is a key target for vaccine and immunotherapy development.
The S protein is first found in a prefusion state, where the S1 domain hides the upper part of the virus spike like a mantle. The tip of the protein holds the receptor-binding domain (RBD), mostly in the ‘down’ state, with no access to the binding site, but has a flip-up state where it presents the binding site for the ACE2 receptor on the host cell for a short time.
If the virus binds to the receptor, the RBD is locked in the ‘up’ position, which makes the S1 mantle unstable. This could favor its change from the prefusion to the post-fusion form.
With fusion, a significant conformational change occurs, and the S2 subunit pushes up the fusion domain to come into close contact with the host cell membrane. S1 is jettisoned in the process.
Scientists who have studied the structure of the RBD say that polar interactions mediate its recognition by the peptidase domain (PD) of the ACE2 receptor, outside the cell.
Several human monoclonal antibodies have been found that bind to the RBD of SARS-CoV at nanomolar concentrations. They prevent its attachment to the ACE2 receptor and in vitro viral replication.
.jpg)
Novel Coronavirus SARS-CoV-2: This scanning electron microscope image shows SARS-CoV-2 (round gold objects) emerging from the surface of cells cultured in the lab. SARS-CoV-2, also known as 2019-nCoV, is the virus that causes COVID-19. The virus shown was isolated from a patient in the U.S. Credit: NIAID-RML
Enter CR3022
These have not been found to bind to the SARS-CoV-2 RBD, however, even though both viruses have a common receptor. The researchers thus turned to another molecule, CR3022, which is a monoclonal antibody directed explicitly against SARS-CoV but which strongly cross-reacts with the RBD of SARS-CoV-2 as well, but does not block ACE2 binding. It is also not mapped as yet because escape mutations could not be generated for it. A natural mutation has been detected in the part that binds ACE2.
Lastly, both CR3022 and another antibody, CR3014, act in an additive manner to result in very potent neutralization of SARS-CoV.
A very recent paper describing the structure of the RBD-CR3022 complex reported that CR3022 does not neutralize SARS-CoV. However, the current study generates a still more detailed study of the same structure, and reports using a different mechanism, that escaped detection by the earlier report, it does result in virus neutralization.
The researchers used cryo-EM techniques to analyze the way CR3022 interacts with the complete extracellular domain of the S protein, and confirm the mechanism of action.
How Does CR3022 Bind the Receptor?
The findings show that the CR3022-RBD binding is tight and allosterically blocks viral binding to the ACE2 molecule and hence inhibits cell entry. In fact, in the presence of ACE2, the RBD-CR3022 binding is slowed down, while it breaks apart faster. Conversely, the release of ACE2 from RBD is sped up in the presence of CR3022.
CR3022 neutralizes SARS-CoV-2, as shown by a plaque reduction assay using MERS convalescent serum as a control, at a concentration similar to the neutralizing concentration for SARS-CoV in earlier studies.
Structure Determination of CR3022
The crystal structure of the SARS-CoV-2-RBD-CR3033 complex was determined by crystallization when two forms of crystal were found within the same drop. One was unexpectedly rich in solvent content at about 87%, and the crystal lattice contained large solvent channels that allowed constant exposure to the ACE2 binding site.
Using a novel algorithm to optimize the phases, a high-quality map was obtained to ensure that the structure was reliably determined.
The second crystal diffracted to a higher resolution, which helped understand the details of the interaction between the RBD and the CR3022, to generate a refined structure of this crystal form.
The binding site of CR3022 is not readily subject to mutation and cannot be bound by the S protein before fusion. This molecule binds to the RBD surface at right angles to the receptor binding site, with no overlap between the two binding epitopes. This independent ACE2 binding has been reported to happen with another neutralizing SARS-CoV-2 antibody.
CR3022 Doesn’t Block the RBD But Neutralizes the Virus
This suggests the unusual value of CR3022 because it is non-competitive with the ACE2 receptor site, which confers high resistance to virus escape. This may mean that it is of immediate use. On the other hand, viruses rapidly develop resistance to competitive antibodies.
In the pre-fusion state of the S protein, the CR3022 epitope is quite inaccessible, entirely so when the RBD flap is ‘down’ and even largely so when it is ‘up.’ When anti-ACE2 antibodies block the receptor, they block the ‘up’ state, causing the prefusion form to become unstable. The binding of CR3022 makes it even more unstable, causing it to cleave and convert to the post-fusion state.
CR3022 thus destabilizes the conformation of the spike protein before fusion, as it cleaves and throws off the S1 subunit, causing virus inactivation. When both the sites are blocked independently, both trigger the conformational change to ‘up.’ This may be why this combination of binding at both sites is synergistic.
After incubating the mixture for 3 hours, no intact S protein was found, but there was a diverse range of oligomers that are probably part of the dissociated S1 assembly. In the living body, these events will probably occur much faster, since the temperature is higher and the mutations introduced into the artificial setting here to stabilize the prefusion S protein will be absent.
The reason why the earlier study failed to note the neutralization effect could be due to the failure to incubate the antibody-bound virus before the cytopathic effect was developed. The same issue occurred with neutralizing antibodies to the influenza virus that did not block the receptor site on the head of the hemagglutinin molecule but bound to its stem. These were not detected by the standard WHO assay for neutralization. Still, neutralization was observed when the antibodies were left to produce a cytopathic effect in the assay during the incubation period.
Applications and Advantages of CR3022
The detailed structure of the binding epitope may make it possible to build another version of CR3022 with a higher affinity or to find a more robust alternative monoclonal for the same site. Moreover, a combination therapy comprising antibodies to both the RBD and the CR3022 binding site could be synergistic, as has been described earlier for the SARS virus.
This type of binding could also prevent antibody-dependent enhancement (ADE) effects since it promotes the conversion of the S protein to the post-fusion state before attachment to the RBD. A vaccine directed against the RBD could also narrow down the range of immune responses and so perhaps dampen the immune pathology seen in COVID-19 illness.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Huo, J., et al. (2020). Neutralization of SARS-CoV-2 by Destruction of The Prefusion Spike. bioRxiv preprint. doi: https://doi.org/10.1101/2020.05.05.079202. https://www.biorxiv.org/content/10.1101/2020.05.05.079202v1
- Peer reviewed and published scientific report.
Huo, Jiandong, Yuguang Zhao, Jingshan Ren, Daming Zhou, Helen M. E. Duyvesteyn, Helen M. Ginn, Loic Carrique, et al. 2020. “Neutralization of SARS-CoV-2 by Destruction of the Prefusion Spike.” Cell Host & Microbe, June. https://doi.org/10.1016/j.chom.2020.06.010. https://www.cell.com/cell-host-microbe/fulltext/S1931-3128(20)30351-6