The current COVID-19 pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is primarily a respiratory infection, though the majority of cases are asymptomatic or mild disease. However, other manifestations are also being reported, such as gastrointestinal features, neurological signs, and skin symptoms. A new study published online in the journal JAMA Dermatology in June 2020 examines the possibility that chilblains could be a manifestation of COVID-19.
Many cases of chilblains have been reported over the last few months, as purplish-red lesions of the hands or feet, leading to a suspected association with mild or asymptomatic COVID-19. The current study was a prospective observational study aimed at identifying a possible link between chilblains and COVID-19.
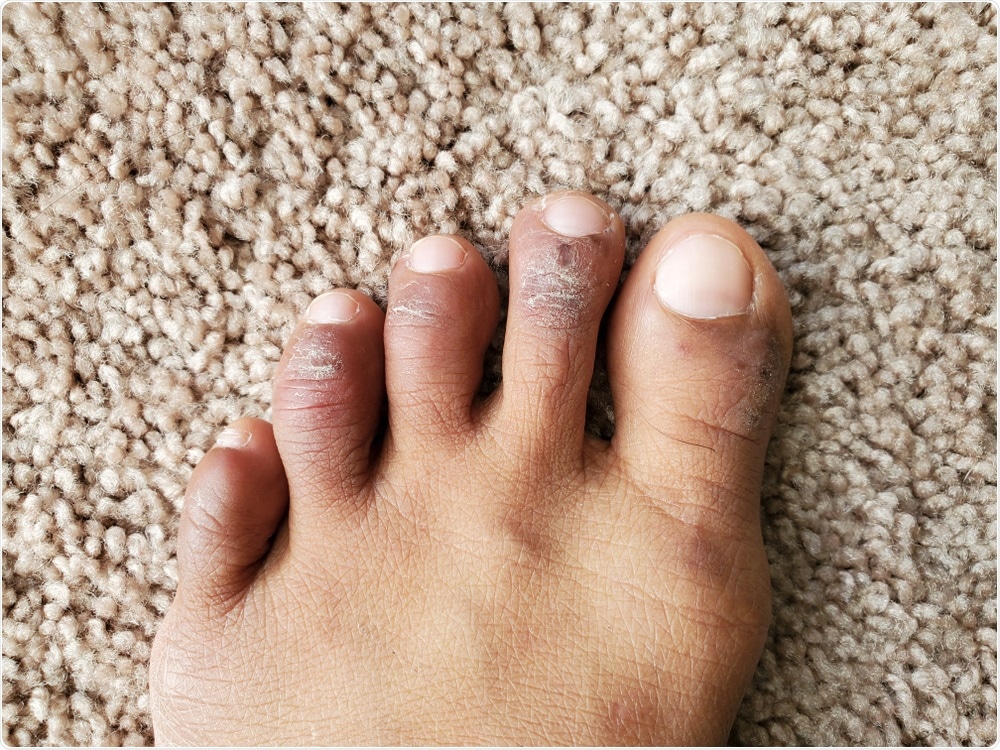
Chilblains on the toes. Image Credit: Ms.Giggles / Shutterstock
The Study: Tracking Chilblains and COVID-19
The researchers looked at 31 patients who presented at a single center in Brussels, Belgium, between April 10 and April 17, 2020, all with chilblain-like purplish-red lesions on the fingers, or toes, or both. These had appeared from 1 to 30 days before the patient came in for a consultation.
There were 11 teenagers, 19 were female, and the median body mass index was 19. Most patients had lesions on the feet, with only 3 patients showing hand lesions. The skin appeared to be reddish or purplish, while sometimes the central part was blistered or dead. The patients also described sensations of itching, pain, burning, and the like.
About two-thirds of the patients had symptoms that could correspond to mild COVID-19, but only 10% said they had come into contact with a COVID-19 case. About a third had had chilblains once or more in the past, while 13% had Raynaud syndrome.
A very few of them were on antihypertensive treatment with beta-blocker drugs, and one was a smoker.
Looking for Evidence of COVID-19
The patients were tested for COVID-19 by reverse transcriptase-polymerase chain reaction (RT-PCR) performed on nasopharyngeal swabs. Blood tests were also carried out for liver and kidney function, autoimmune vasculitis, other abnormal proteins, and coagulation parameters.
The patients were also tested for specific IgM and IgG antibodies. Some also had skin biopsies, histologic and immunofluorescence tests, and RT-PCR of the skin samples.
The diagnosis of chilblains was confirmed in 22 patients on histopathology, but the other tests were either negative or not useful. In seven patients, vasculitic changes were seen in the small blood vessels of the skin underlying the lesions, with deposits of IgM, IgA, and complement.
None of the patients were positive for the virus on SARS-CoV-2 on RT-PCR of the nasopharyngeal swabs, or in the skin samples. Neither were the antibody tests positive for either IgM or IgG. Blood tests were mostly normal. Autoimmune antibodies were present at low levels in seven patients, with significant concentrations being found in one patient with a history of chilblains.
Chilblains Due to Lockdown Lifestyle?
The current study was conducted because of the occurrence of ischemic lesions on the extremities of the body in both adults with severe COVID-19 and children without any health condition. In the former, cyanotic skin lesions are observed, and are suspected to be due to systemic injury to the blood vessels, especially clotting induced by viral injury.
However, none of the skin samples in this study showed other than typical chilblain lesions, with vasculitis or microthrombi in a few cases, and sometimes IgM and/or complement deposits that could suggest vasculitis of the small vessels.
To rule out the possibility of the chilblains being a late manifestation of the disease, serologic testing was also done, and this also turned out to be negative, with tests that were 100% sensitive and specific at 15 days from the symptoms.
The researchers, therefore, conclude that these patients were not infected with COVID-19. Instead, the two events may be linked in some other way. For instance, the lockdown may have led to lifestyle changes that may have increased the risk of chilblains, such as not going to work and increased sedentary lifestyle activities.
About two-thirds of the patients said they had spent less time in physical activity and much more time sitting than before the lockdown. Most of them said they wore only socks or remained barefoot throughout the day. The low BMI also offers a hint that thin people may be at higher risk for this complication if inadequately protected against the cold.
Thus, these skin lesions are likely to be due to lifestyle changes secondary to the lockdown. It is important not to jump to conclusions about unusual manifestations of disease during this pandemic season, relating them to the viral infection unless otherwise proved by careful testing.