The current COVID-19 pandemic has stimulated intensive research into the pathogenesis of the disease, especially since, in the most critical cases, hyper-inflammation secondary to immune activation appears to play a crucial role.
A recent study by researchers at the University of North Carolina at Chapel Hill and The Rockefeller University and published on the preprint server bioRxiv* in September 2020 shows that a combination of neutralizing antibodies with intact Fc effector function can effectively reduce the viral load and prevent infection.
HumAbs in COVID-19
Coronaviruses (CoV) are known to jump across species barriers, which underlies the current human outbreak, just like the last two, namely, the SARS and MERS epidemics. The lethality of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) in elderly and sick patients has made the requirement of effective antivirals and vaccines a necessity.
Preclinical studies of human monoclonal antibodies (huMabs) in monkeys and hamsters have shown some promise, but the difficulty of these experiments, when performed in BSL3 conditions, has discouraged further examination of their effector function, ability to neutralize the virus and optimal combinations in preventing and treating COVID-19.
Antibodies bind via their Fc fragment to activate effector functions such as antibody-dependent cellular cytotoxicity and phagocytosis. Fc binding as well as interactions between Fc and cellular Fc receptors, also trigger other innate and adaptive immune responses like antigen presentation and B cell activation. The effector functions mediated by the Fc antibody fragment may affect the adaptive immune response in many different ways.
The current study reports on combinations of humAbs, directed against epitopes in the receptor-binding domain (RBD) of the SARS-CoV-2 spike (S) protein. The researchers used a mouse model with a remodeled spike RBD since the mouse angiotensin-converting enzyme 2 (mACE2) is not bound by the RBD of SARS-CoV-2 spike protein. This recombinant virus, SARS-CoV-2 MA, can infect and replicate efficiently in the mouse lung and is used for many vaccine and therapeutic tests.
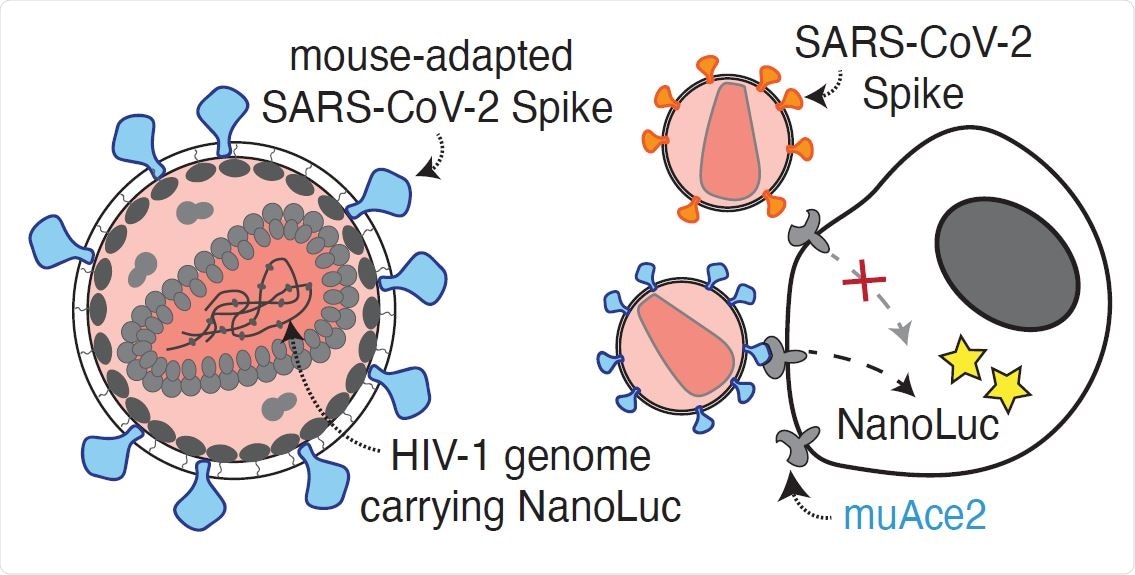
Antibody potency against the mouse adapted SARS-CoV-2 spike. A. Diagram of the mouse-adapted (MA) SARS-CoV-2 pseudovirus luciferase assay. SARS-CoV- 2 mouse-adapted spike (SARS-CoV-2 S-MA) pseudotyped HIV-1 particles carrying the nanoluc gene are used to infect murine (mu) Ace2-expressing HT1080 cells, which will express nanoluc luciferase upon infection, while SARS-CoV-2 spike (wtS) pseudotyped particles are unable to infect muAce-expressing cells.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Mutations Leave Neutralization Capacity Intact
Using a pseudovirus, the researchers first looked at whether the mutation in the RBD would leave neutralization capacity intact. They tested the S-MA pseudovirus against 8 distinct IgG1 humAbs covering a range of potencies, with IC50 starting from 4.4 ng/mL to 26/140 ng/mL. They found that except for one, all of them had similar antibody neutralization titers with both the wild-type and recombinant SARS-CoV-2 viruses.
The exception was with one (C119), which was directed against an epitope that overlapped the mutations introduced in order to adapt to the mouse.
However, in vitro effects are not always reliable as a predictor of in vivo potency. Therefore, the investigators looked at how effectively these antibodies worked in BALB/c older mice. They found that C119 did not prevent S-MA infection in these mice, but the others produced partial or full protection.
Protection via antibody Fc-effector function
One factor that could be important in this respect is the Fc-white cell Fc receptor interactions, which have been demonstrated to be essential to viral clearance and killing of infected host cells in vivo, in HIV-1, Ebola, and Influenza infections. The researchers suggest that the angle at which the RBD and ACE2 interact in vivo determines antibody potency to a large extent, by altering how well the antibody Fc receptor can bind to its receptor on effector immune cells.
Further work showed that the Fc receptor-mediated protection is required for the highest level of infection prevention by the recombinant virus in vivo. The recombinant mouse and wild-type human C104 IgG2 and IgG1, respectively, had similar protective efficacy because these are activating Fc receptors. Not so the mouse antibodies C104-IgG1 and C104-IgGD265A, which demonstrated a recognizable lack of activity since they bind to inhibitory Fc receptors.
Combinations of antibodies
The researchers point out that combining antibodies targeting non-overlapping epitopes is likely to prevent escape mutations, and they examined antibody mixtures that target the RBD. They compared a mixture of varying low doses of each antibody with a moderate dose of each antibody alone. They found two combinations of two different antibodies performed with similar sterilizing or near-sterilizing efficacy, respectively, at a total dose of either 16mg/kg or 5.3 mg/kg.
The study also shows that one of these antibodies, namely, C144, not only blocks the interaction between the RBD and ACE2 but also locks the RBD in the ‘down’ conformation, so that it is no longer accessible to the host ACE2. Another set of three neutralizing antibodies also prevents RBD-ACE2 interactions but bind at other angles and through varying mechanisms. It is noteworthy that among them, the least potent neutralizing activity in vitro is shown by the C104 antibody, which shows the greatest efficacy in vivo.
In Vivo Testing Required to Validate In Vitro Results
The in vitro neutralization capacity does not involve antibody Fc effector functions that determine in vivo antiviral efficacy. To study the latter, the researchers, therefore, made use of a mutation to prevent Fc receptor interaction in three selected anti-RBD antibodies, C002, C104, and C110.
As posited, in vitro studies failed to show any difference between the inhibitory activity of these mutants and the wild-type humAb against S-MA. However, in vivo, the least potent of the three mutants continued to show the same level of inhibition as the wild-type antibody, but not the other two, which suffered a 14- and 6-fold loss of efficacy with the loss of Fc effector function.
They also found that interactions with activating Fc receptors are necessary for high levels of neutralizing activity, in vivo but not in vitro, underscoring the differences in readings acquired by in vivo and in vitro experiments on neutralizing antibodies. In vitro results are not linearly correlated to in vivo activity.The study draws attention to the need for in vivo testing of the neutralizing activity of SARS-CoV-2 antibodies, using pseudovirus and microneutralization assays, and relating these to the in vitro results.
Implications
The results suggest that neutralizing antibodies act via the “engagement of activating Fc receptors and that some antibody combinations can enhance the efficacy of anti-SARS-CoV-2 antibodies in vivo.’ The researchers also point out, “Our experiments indicate that Fc receptors are also essential for optimal antibody-mediated protection against SARS-CoV-2.”
Following the induction of passive immunity by transferring humAbs, there is little risk of antibody-dependent enhancement (ADE) of infection driven by Fc receptor engagement in the case of SARS-CoV-2, which targets human lung epithelium, unlike in Dengue, where immune white cells carrying Fc receptors are the primary focus of the virus.
Finally, in vitro tests show that antibodies can target escape mutations, and the use of combinations of antibodies that target completely distinctive sites can prevent this possibility very effectively. Synergistic activity is also possible but has not been observed in vitro. However, it is clear that antibodies, in combination, are far more potent in preventing infection with the virus.
The study concludes, therefore, “The data supports the idea that specific combinations of antibodies with intact Fc effector function and should be developed for optimal protection against SARS-CoV-2.’

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Schaefer, A. et al. (2020). Antibody Potency, Effector Function and Combinations In Protection From Sars-Cov-2 Infection In Vivo. bioRxiv preprint. doi: https://doi.org/10.1101/2020.09.15.298067. https://www.biorxiv.org/content/10.1101/2020.09.15.298067v1
- Peer reviewed and published scientific report.
Schäfer, Alexandra, Frauke Muecksch, Julio C.C. Lorenzi, Sarah R. Leist, Melissa Cipolla, Stylianos Bournazos, Fabian Schmidt, et al. 2020. “Antibody Potency, Effector Function, and Combinations in Protection and Therapy for SARS-CoV-2 Infection in Vivo.” Journal of Experimental Medicine 218 (3). https://doi.org/10.1084/jem.20201993. https://rupress.org/jem/article/218/3/e20201993/211549/.