Patients with the coronavirus disease (COVID-19) develop symptoms such as cough, fever, and difficulty of breathing. It has long been known that COVID-19 is a respiratory illness, but as the pandemic evolves, many clinicians report varying symptoms, hinting that the virus affects multiple organs, including the brain.
Nearly a third of hospitalized COVID-19 patients experienced some type of altered mental state and function, ranging from delirium to confusion, and in some cases, unresponsiveness, a new study has found.
A team of researchers at the Ken & Ruth Davee Department of Neurology, Northwestern University Feinberg School of Medicine, Chicago, Illinois, aimed to gain a better understanding and to characterize the neurological manifestations, risk factors, and associated outcomes in COVID-19 patients who are hospitalized.
They found that of the 509 patients who were studied, 82 percent had neurological manifestations during the course of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, including muscle pain, headaches, dizziness, alteration in mental function, and problems with their sense of smell and taste.
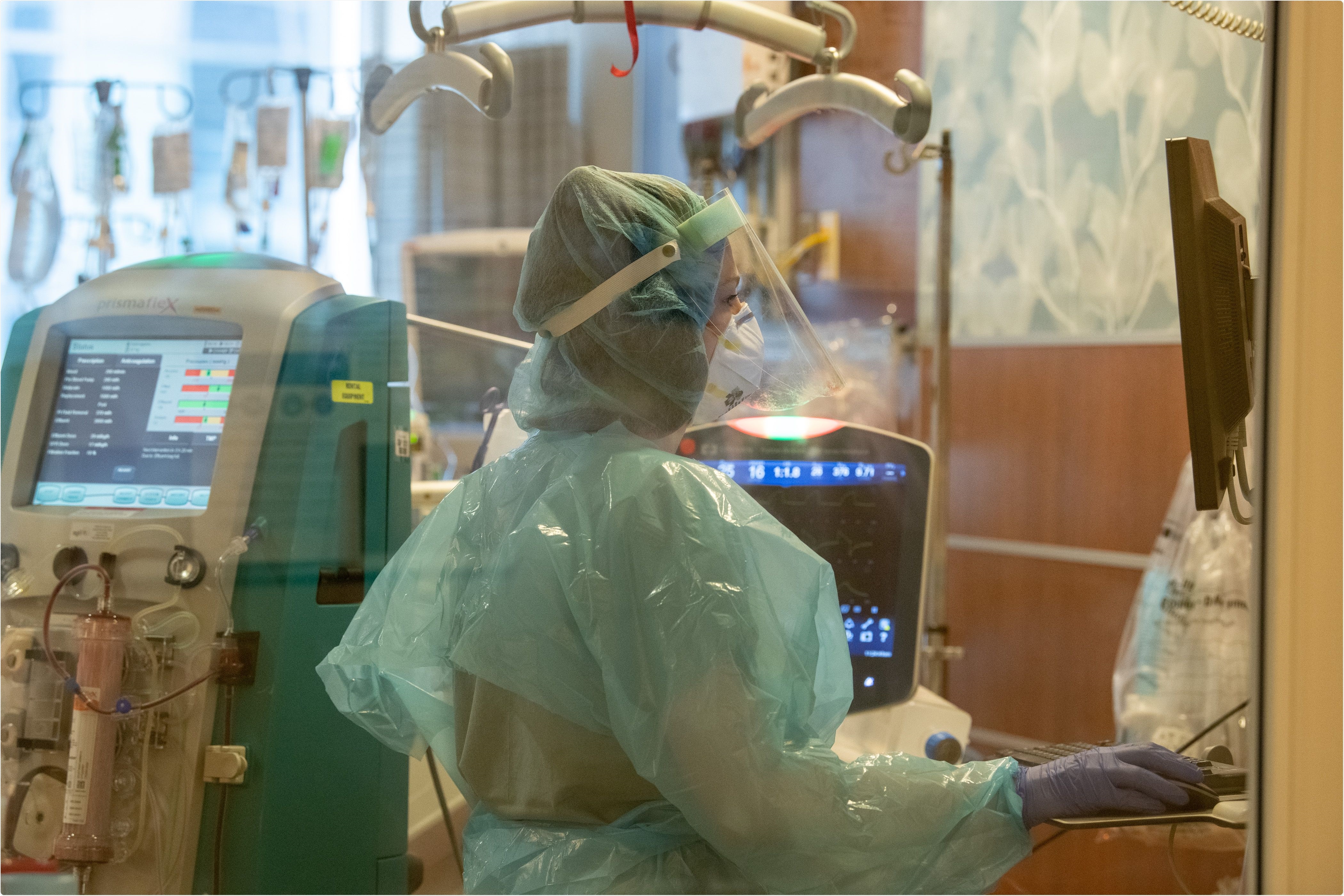
Image Credit: Northwestern Medicine
The study
To arrive at the study findings, which appeared in the Annals of Clinical and Translational Neurology, the researchers examined neurologic manifestations in more than 500 patients who were admitted to a hospital network in Chicago, Illinois, due to COVID-19.
The team compared the severity of COVID-19 outcomes in patients and determined predictors of any neurological manifestations, encephalopathy, and functional outcome using binary logistic regression.
What did the researchers find?
Results of the study show that symptoms range from mild to severe, including headaches, dizziness, and altered mental function. These findings underline the broad-ranging impacts of the virus on the body. Further, the study revealed that patients may persist in experiencing the symptoms even if they have already recovered from the viral infection, which has now sickened more than 35.68 million globally.

Image Credit: Northwestern Medicine
Of the more than 500 patients in the study, the team detected neurologic manifestations at COVID-19 onset in 215 patients, equivalent to 42.2 percent. At hospitalization, these symptoms were seen in 319 patients (62.7 percent), and at any time during the disease course in 419 patients (82.3 percent).
The team unveiled that the most frequent neurological symptoms in COVID-19 patients included myalgias, headaches, encephalopathy, dizziness, dysgeusia, or the distortion of the sense of taste, and anosmia or the loss of smell.
However, stroke, motor and sensory deficits, mobility disorders, seizures, and ataxia were uncommon.
Encephalopathy, which is defined as damage, malfunction, or disease in the brain, which can lead to mild to severe neurological manifestations, including memory loss, personality changes, altered mental state, confusion, dementia, seizures, coma, or death.
Furthermore, the team has found that the independent risk factors in patients for developing any neurologic manifestations were severe COVID-19 and younger age.
“This is the first study of its kind in the United States,” Dr. Igor Koralnik, chief of neuro-infectious diseases and global neurology in the Ken & Ruth Davee Department of Neurology at Northwestern Medicine, said.
“There are only two other published papers describing the prevalence of neurological manifestations in hospitalized COVID-19 patients in China and Europe. Our research group spent the summer performing chart reviews on the first 509 patients hospitalized for COVID-19 within the Northwestern Medicine health system, and our findings show neurological manifestations are very common in these patients,” he added.
What is more, the team discovered that upon discharge from the hospital, only 32.1 percent of the patients with encephalopathy were able to handle routine daily activities, such as cooking or running errands like paying bills. In contrast, 89 percent of patients who did not develop encephalopathy or altered mental function were able to perform their daily activities without assistance.
There was also higher mortality or death in patients with encephalopathy at 21.7 percent, compared to 3.2 percent of those who did not develop the condition.
“We are now looking to characterize the long-term neurologic effects of COVID-19 and the cognitive outcomes in patients with COVID-19-associated encephalopathy,” Dr. Koralnik said.
“We’re studying this in patients who are discharged from the hospital, as well as in COVID-19 ‘long-haulers,’ who have never been hospitalized but also suffer from a similar range of neurological problems, including brain fog,” he added.
The study findings highlight the effect of COVID-19 on the brain, which can lead to serious complications in some patients. They concluded that neurologic manifestations happen in most patients hospitalized due to COVID-19.
“Encephalopathy was associated with increased morbidity and mortality, independent of respiratory disease severity,” the authors wrote in the paper.
Sources:
Journal reference: