Laboratory studies have shown that SARS-CoV-2 – the causative pathogen of COVID-19 – is not very stable in warmer temperatures and high humidity. Other studies have found both positive and negative associations between the weather and viral transmission, based on daily confirmed case statistics.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
However, using daily positive cases may not be very useful in studying the climate’s effect of SARS-CoV-2’s transmission. For instance, this data does not include the many cases that go undocumented, the lag between infection and symptom onset and the lag between testing and reporting. Additionally, many studies have not controlled for other confounding factors such as the implementation of health interventions, socioeconomic factors and other environmental factors.
To account for these issues, the authors used the mean reproduction number to allow for delayed reports, unreported infections and population movements. The authors also controlled for other factors like smoking, air pollution, and obesity and making the model stronger.
Researchers from Yale University and Columbia University in the United States have published a paper on the medRxiv* preprint server that explores further the relationship between SAR-CoV-2 transmissibility and the weather. The team looked at the association between air temperature and humidity on SARS-CoV-2 transmission in the US based on the virus’s reproduction number, a metric used to calculate the rate of infection of a pathogen in a population. They define the reproduction number as the mean number of new infections caused by a single infected individual, taking into account public health interventions and assuming everyone in the population is susceptible.
Modeling virus transmission and weather
The team gathered temperature and specific humidity data for 913 US counties, specific humidity being defined as the mass of water vapor in a unit mass of moist air. They also collected other data for the counties, such as geographic location, population demographics, socioeconomic factors and air pollution.
They estimated the daily reproduction number using a metapopulation model where they considered two types of movements: daily commuting for work and random movement. They fitted the transmission model to county-level deaths and daily cases reported between 15 March 2020 and 31 August 2020.
They found the mean reproduction number to be between 0.46 and 5.43. The daily mean temperature varied widely between about 14 and 40 ºC, and the specific humidity varied between about 1 and 22 g/kg.
The largest number of cumulative cases per 100,000 people was in Chattahoochee County, Georgia; conversely, Taylor County, Florida, had the lowest number. Counties in the south were generally hotter and more humid than northern US counties, and coastal counties were cooler and more humid than counties inland.
Using this model, the researchers found lower temperatures were associated with higher transmission of SARS-CoV-2, below an optimum temperature of 32.6 ºC. There was no association above the optimum temperature, however.
The relationship between the reproduction number and specific humidity was non-linear. There was lower transmission at higher specific humidity, except for an increase between 9 to 15 g/kg.
The authors also estimated the fraction of the reproduction number attributable to temperature or specific humidity. Across the 913 counties studied, the fraction attributed to temperature was 5.1%, and the fraction attributed to humidity was 14.5%. The attributable fraction for temperature increased from south to north. The attributable fraction for humidity increased from south to north in eastern parts of the country, while in the western parts, the attributable fraction was lower in coastal counties and higher inland.
Humidity affects transmission more than temperature
The authors found lower temperatures and lower specific humidity were associated with an increased reproduction number, or higher viral transmission. SARS-CoV-2 transmission was associated more with temperature and humidity in colder and drier counties than in warmer and more humid counties. These results are thus in line with some previous studies in the area.
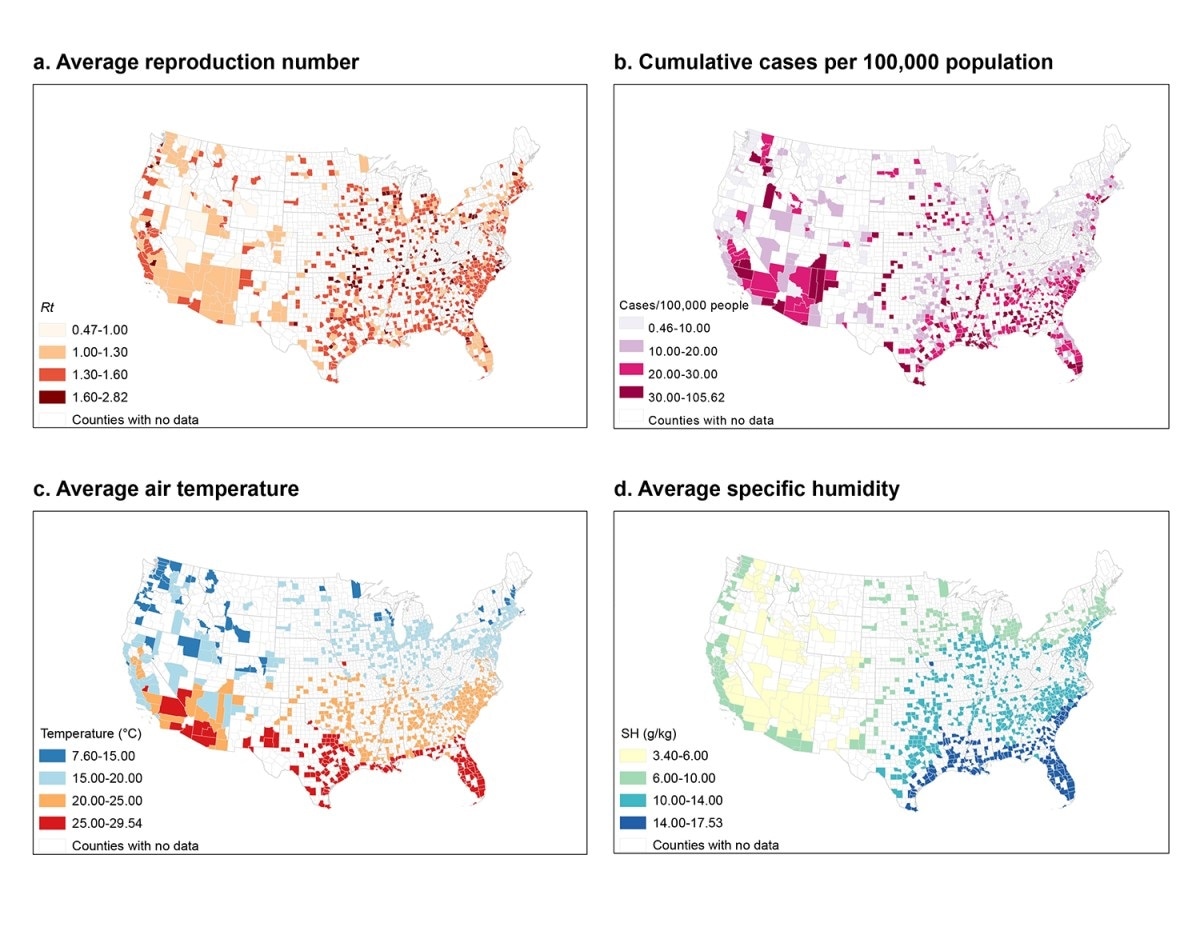
Map of the distribution of reproduction number, cumulative cases, air temperature 85 and specific humidity in study counties.
Lab testing of SARS-CoV-2’s acclimation to temperature and humidity alterations also found it to be less stable at higher temperatures and humidity compared to lower temperatures and humidity. Furthermore, the SARS-CoV-2 virus half-life decreased when relative humidity was increased from 40% to 65% at 22 ºC and 27 ºC, but increased when the humidity increased from 65% to 85%. This is similar to the non-linear association found using the present study’s model.
Thus, the specific humidity contributed more to virus transmission than temperature, but it was not clear if humidity is a cause or an indicator of virus transmission. Further study in this area will need to be done to clarify this issue.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources