Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is the causative agent of coronavirus disease 2019 (COVID-19), a respiratory infection for which no specific vaccine is currently available. Studies show that individuals who have recovered from COVID-19 have SARS-CoV-2-specific T cell memory and T cell dysfunction, and hence T cells can play a pivotal role in mounting a robust immune response against COVID-19.
The potential link between BCG vaccination and protection against severe COVID-19
Several epidemiological studies suggest that the Bacillus Calmette-Guérin (BCG) vaccine may offer protection against COVID-19. BCG vaccine contains live attenuated Mycobacterium bovis, and is typically used as a vaccination against tuberculosis (TB). Like other vaccines, BCG can induce cross-protection against other pathogens as well. This cross-protective effect has been shown to reduce respiratory tract infections in adults and all-cause mortality in children.
However, the mechanism by which the BCG vaccine elicits a SARS-CoV-2-specific T cell response is not clear. Currently, there are over 15 clinical trials in progress to determine if BCG vaccination can help reduce or prevent the severity of COVID-19 disease.
Investigating the ability of BCG vaccine to produce cross-reactive T cells specific to SARS-CoV-2
Recently, researchers from the Monash University and Monash Medical Centre, Clayton, Victoria, Australia, investigated whether peptide sensitization using BCG can produce cross-reactive T cells specific to SARS-CoV-2. Their study is published on the preprint server, medRxiv*.
In this work, the researchers identified 8 BCG-derived peptides in silico with considerable sequence homology to either SARS-CoV-2 NSP3 or NSP13-derived peptides. They used an in vitro co-culture system and showed that human CD4+ and CD8+ T cells primed with a BCG-derived peptide developed high reactivity to its corresponding SARS-CoV-2-derived peptide.
BCG peptides helped enhance T cell reactivity to SARS-CoV-2 peptides
Owing to the human leukocyte antigen (HLA) differences between individuals, not all persons developed immune responses to all 8 BCG-derived peptides. Nevertheless, all 20 individuals primed with BCG-derived peptides developed improved T cell reactivity to 7 of 8 SARS-CoV-2-derived peptides.
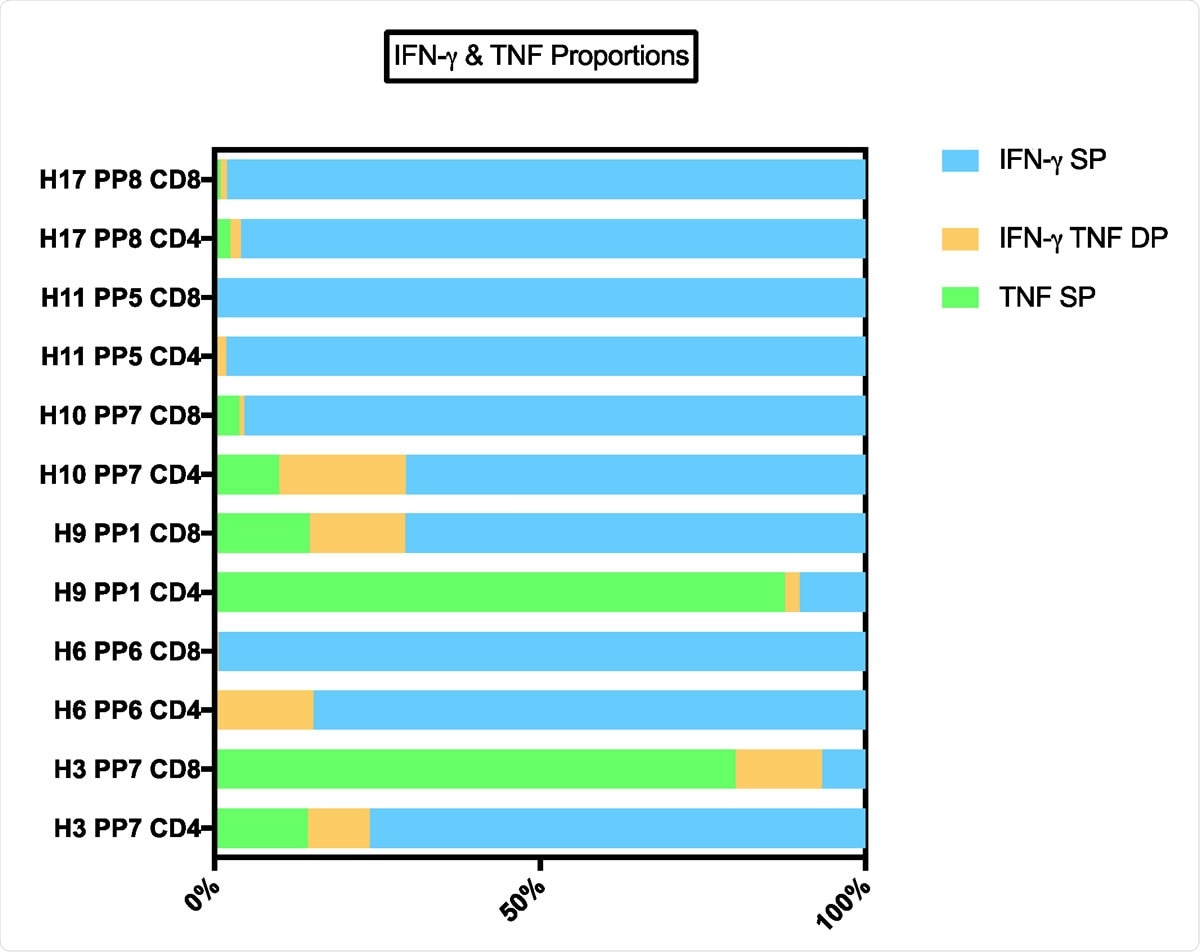
TNF IFNγ proportions of responder individuals. BCG-primed individuals who responded to SARS-CoV-2-peptide restimulation mostly exhibited a strong IFNγ signature with a lower proportion of TNF, although some individuals showed a dominant TNF response. Across individuals and peptide pairs, a variable proportion of IFNγ SP, TNF SP and IFNγ, TNF DP was observed. A selection of 6 individuals CD4+ and CD8+ responses (of N = 20 tested) against 5 peptide pairs (PP) of 8 peptide pairs tested. IFNγ single positive (SP) – proportion of cells producing IFNγ and not TNF. TNF SP – proportion of cells producing TNF and not IFNγ. IFNγ TNF double positive (DP) – proportion of cells producing TNF and not IFNγ.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Cytokine production patterns varied between individuals and peptide pairs, as is clear from the complex pattern of T cell cytokine expression and phenotypes that BCG vaccination produces. The IFN-g and TNF response was mixed, as some individuals produced either IFN-g or TNF in response to a particular peptide pair, and others produced both. These observations agree with previously reported responses in COVID-19.
The researchers also observed that CD8+ T cells primed with BCG-derived peptides showed an enhanced perforin expression upon SARS-CoV-2 restimulation compared to the control primed cells.
“Cross-reactive perforin expression in responders was significantly increased across all 8 peptide pairs with a mean fold increase ranging from 1.9-fold (PP1) to 47.2-fold (PP4).”
Findings support epidemiological observations suggesting BCG vaccination protects COVID-19
The main objective of this study was to show that the observed benefits of BCG vaccination in reducing the severity of COVID-19 can be ascribed to T cell cross-reactivity. Overall, the study results suggest that CD4+ and CD8+ T cells specific for BCG-derived peptides are cross-reactive to SARS-CoV-2-derived peptides. These findings offer a mechanistic explanation for the epidemiologic observation that BCG vaccination protects COVID-19.
Based on the results, the authors endorse the use of BCG vaccination to trigger cross-reactive SARS-CoV-2-specific T cell response. They also support the continuation of ongoing clinical trials across the world, especially in individuals at high-risk of contracting SARS-CoV-2.
“These data provide a mechanistic explanation for the observed negative epidemiological associations between BCG vaccinations and COVID-19 severity and mortality and support the continuation of clinical trials around the world, particularly in people at high risk of contracting SARS-CoV-2.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
BCG vaccine derived peptides induce SARS-CoV-2 T cell cross-reactivity Peter J Eggenhuizen, Boaz H Ng, Janet Chang, Ashleigh L Fell, Wey Y Wong, Poh-yi Gan, Stephen R Holdsworth, Joshua D Ooi medRxiv 2020.11.21.20236018; doi: https://doi.org/10.1101/2020.11.21.20236018, https://www.medrxiv.org/content/10.1101/2020.11.21.20236018v1
- Peer reviewed and published scientific report.
Eggenhuizen, Peter J., Boaz H. Ng, Janet Chang, Ashleigh L. Fell, Rachel M. Y. Cheong, Wey Y. Wong, Poh-Yi Gan, Stephen R. Holdsworth, and Joshua D. Ooi. 2021. “BCG Vaccine Derived Peptides Induce SARS-CoV-2 T Cell Cross-Reactivity.” Frontiers in Immunology 12 (August). https://doi.org/10.3389/fimmu.2021.692729. https://www.frontiersin.org/articles/10.3389/fimmu.2021.692729/full.