As a second wave of the COVID-19 pandemic hits many regions worldwide, a new study reports a method to monitor the effective reproduction number (Re) in near real-time. The study, published on the preprint server medRxiv* in November 2020, helps assess the status of the pandemic in any given country, while it allows different public health policies and other factors affecting the rate of viral transmission to be compared directly between countries.
The Re value is an essential tool for monitoring the rate at which an infectious disease is spreading. It calculates the average rate at which infected individuals transmit to others. When it drops below 1, the epidemic is no longer self-sustaining and reduces in size. Some important factors that change the Re during an epidemic include a marked reduction in the number of susceptible individuals, seasonal drop in transmission, changes in the way infected and non-infected people interact, and the effect of pharmaceutical and non-pharmaceutical interventions (NPIs).
There are two main methods of calculating the Re, the first category following a compartmentalized model and those which count the number of secondary infections for each primary infected individual directly in a time-series model of incidence.
Advantages of time series incidence modeling
The current study follows the second method. The chief difficulty here is the inability to directly observe the secondary infections, which brings in the need to identify their probable occurrence by testing of symptomatic individuals or by regular surveillance by testing a group of contacts, for instance. This necessarily entails a delay in detection and the use of a proxy indicator of infection such as the incidence of infection, hospitalization and death.
This method also has the advantages of requiring few and simple assumptions and can independently use multiple indirect indicators of infection events, allowing for sensitivity analyses.
The critical point for such a method is the availability of broad-based accurate data. The researchers in this study used data provided by different public health authorities, from various case reports, such as those on deaths, hospitalizations and total cases. This was for comparative purposes, which increased the validity of the final estimates.
They also used the Re to assess the association between various NPIs and viral transmission, which will help to formulate further decisions on public health policy. The Re values were first fixed at about 3, then dropped below 1 and then hovered just above 1 for some time. They observed that using this method allowed them to track the Re accurately, over the whole period of the pandemic so far, especially whether it was below or above 1 at any point. The actual date at which the Re crosses this threshold could be identified within a margin of 3 days or less.
The Re estimate is also appropriate for smaller-scale studies. For instance, it may be applied to estimate the Re relative to local transmission alone, disregarding imported cases. This part of the work was assisted by data from the Federal Office of Public Health (FOPH) in Switzerland, regarding the Swiss COVID-19 outbreak.
Lockdowns associated with arrest of epidemic expansion
The researchers found that in most cases, the Re fell below 1 only after nationwide lockdowns were put in force. Comparing multiple NPIs with the dates of interventions, in 20 European nations with good-quality data, they found that all, except Sweden, had issued stay-at-home orders. In all these countries, Re was significantly above 1 before the lockdown, except for Denmark. The most reliable estimates are based on the number of cases rather than the number of deaths, because the latter is much smaller. Still, the results are similar, whatever the type of data used, say the researchers.
They also repeated the same study with 39 countries across the world, which had implemented stringent NPIs. They found that 28 of them had an Re above 1 before the date when the NPIs crossed a stringency index (SI) of 50. The faster the government instituted a lockdown, the more rapid was the decrease in Re. In Europe, as the SI changed to a larger extent, reflecting stronger interventions, in the days before it reached 50, the Re estimate fell by a larger extent on the reference date.
This same pattern was seen in the global study, though the changes were not significant. The presence of such trends indicates that the lockdowns were necessary to clamp down on viral spread, since the Re was much above 1 at that point, rather than being below it, as was often claimed.
The best way to predict when Re falls below 1 is the Re on the day when lockdown begins, they found, rather than the SI at lockdown. They also observed little association between the highest SI during the lockdown and the lowest Re attained during this period. In places like Africa, for instance, where, in some cases, the NPIs were introduced even before any cases were detected, there was obviously no detectable change in Re.
The results also shed light on the effects of relaxations of NPIs, in North America, Asia and Europe, where increases in the SI were more significantly linked with a lower Re estimate than reducing the SI. “This suggests that reversing non-pharmaceutical interventions had a very different effect than introducing them.” This could be due to continuing changes in public behavior and public health measures like contact tracing and quarantine, which reduces viral transmission even without a lockdown.
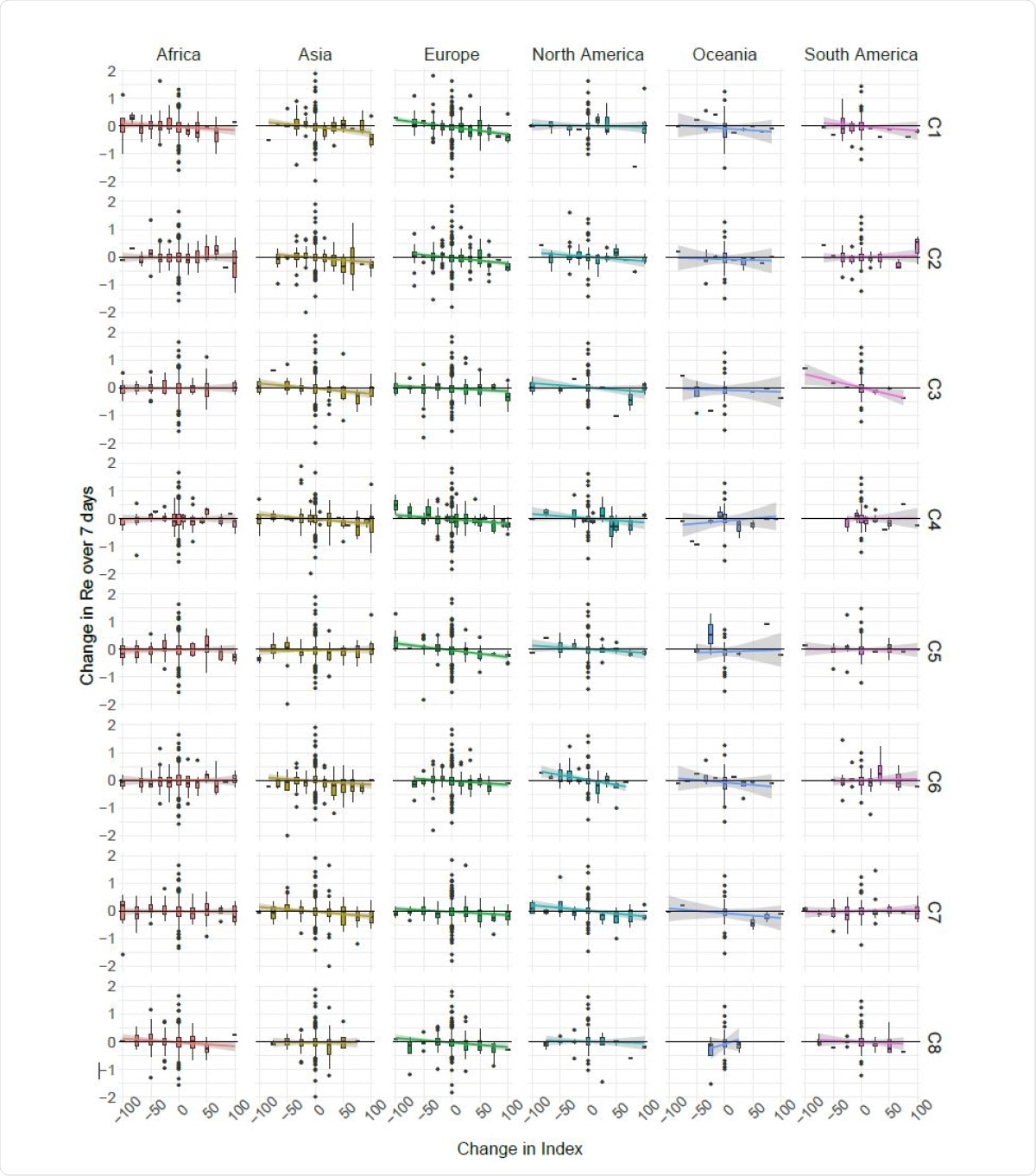
The one-week change in Re following changes in government stringency.
What are the implications?
To sum up, the findings show that NPIs are associated with a decline in Re, but their relaxation does not immediately cause a reversion to the original values.
The researchers stress the importance of communicating such results to win public confidence in health policies that affect their daily life and economic well-being. The investigators also constructed an online dashboard where all Re estimates are put up, using observations from multiple sources. This would allow comparisons within a country, between countries, or between multiple data sources such as hospitalizations versus cases or deaths.
In their words, “During the ongoing SARS-CoV-2 pandemic, Re estimates are of interest to health authorities, politicians, decision makers, the media and the general public. Because of this broad interest and the critical importance of Re estimates, it is crucial to communicate both the results as well as the associated uncertainty and caveats in an open, transparent and accessible way. This is why we display daily updated results on an online dashboard, accessible at https://ibz-shiny.ethz.ch/covid-19-re/.”
Along with data on the virus characteristics, it is important to account for lockdown fatigue, local cultural factors, trust in governmental and public health authorities and in scientists, as well as financial stress induced by stringent NPIs, all of which can confuse the final results of Re estimation. Future studies could use this method to explore these contributions as well as that of variations in weather and in climate, so as to arrive at the lowest level of NPIs that, in combination with other active factors, will peg the Re below 1 for a given location.
The authors conclude, “Generally, our framework is useful both to inform governments and the general public on the status of the epidemic in their country, as well as a source for detailed comparison between countries and in relation to local public health policies and external covariates such as mobility, behavioural, or weather data.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Huisman, J. S. et al. (2020). Estimation and worldwide monitoring of the effective reproductive number of SARS-CoV-2. medRxiv preprint. doi: https://doi.org/10.1101/2020.11.26.20239368, https://www.medrxiv.org/content/10.1101/2020.11.26.20239368v1
- Peer reviewed and published scientific report.
Huisman, Jana S, Jérémie Scire, Daniel C Angst, Jinzhou Li, Richard A Neher, Marloes H Maathuis, Sebastian Bonhoeffer, and Tanja Stadler. 2022. “Estimation and Worldwide Monitoring of the Effective Reproductive Number of SARS-CoV-2.” Edited by Miles P Davenport. ELife 11 (August): e71345. https://doi.org/10.7554/eLife.71345. https://elifesciences.org/articles/71345.