The coronavirus disease 2019 (COVID-19) pandemic caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has presented new challenges to food manufacturers.
Environmental monitoring for foodborne pathogens such as Listeria and Salmonella are routinely conducted in food production facilities. With the COVID-19 pandemic, it is an additional challenge to protect the personnel in the food production facilities and mitigate the transmission of the virus from the facilities.
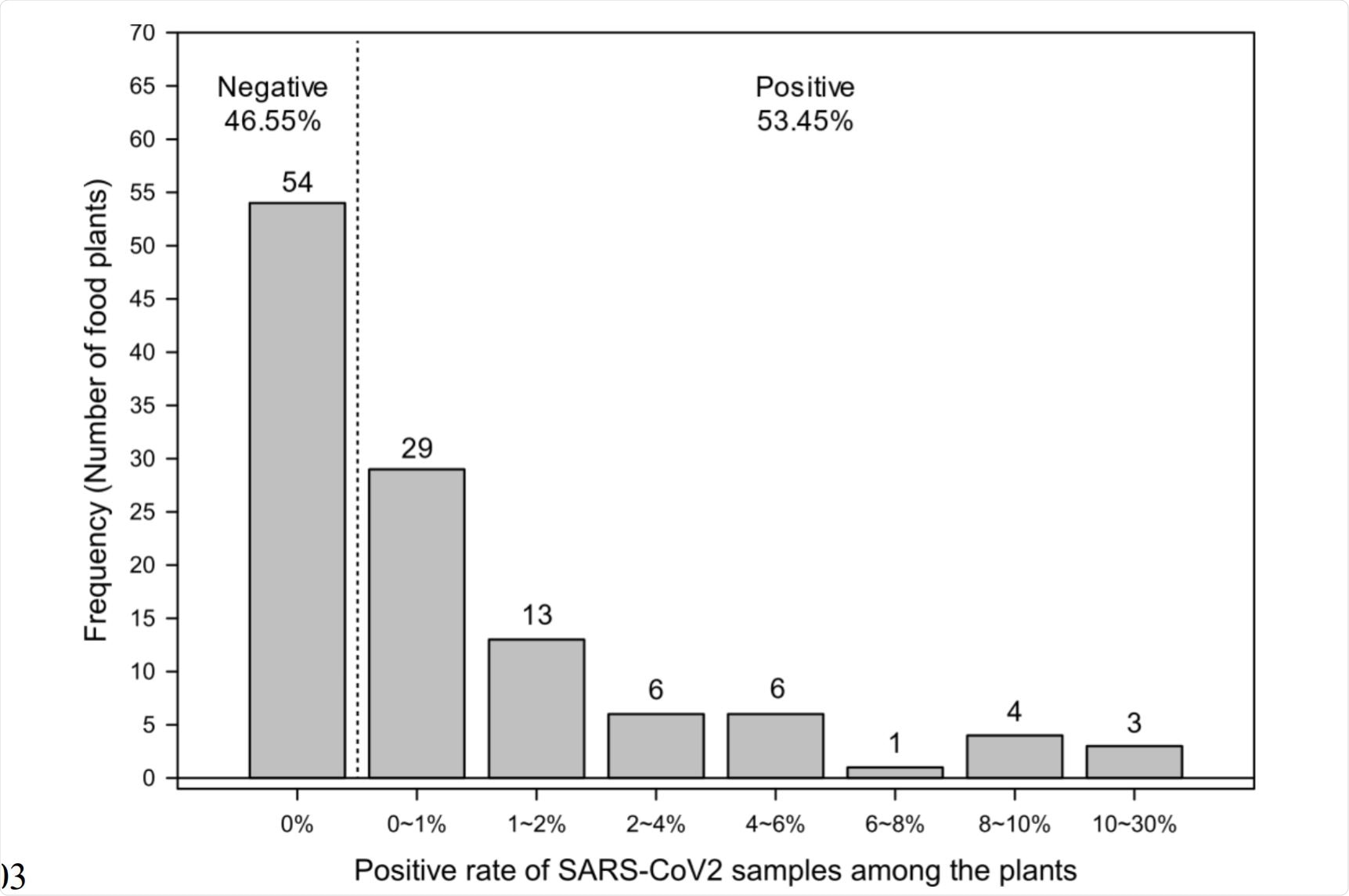
Histogram of percentage of positive cases for each individual plant (n=116). Image Credit: https://www.medrxiv.org/content/10.1101/2020.12.10.20247171v1.full.pdf

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Ziwen Ming et al. have recently investigated SARS-CoV-2 on surfaces in food plants. The team from the Institute of Environmental Health has tested for the presence of SARS-CoV-2 RNA in 22 643 surface samples from the food processing facilities in the US. The positive detection of the SARS-CoV-2 virus in the food plants was published in the medRxiv* preprint server.
The authors collected these samples from 116 food manufacturing plants between March 17 2020, and September 3, 2020. They found that 278 (1.23%) of the samplings were positive for the SARS-CoV-2, with the frequently touched surfaces being most contaminated.
Surface testing for SARS-CoV-2 may indicate presence of asymptomatic carriers.”
They applied the sampling buffer impregnated swab to the facility's built-environmental surfaces and transferred it to a vial containing viral transport medium (VTM).
The SARS-CoV-2 RNA was extracted and detected using The IEH SARS-CoV-2 RT-PCR Test kit. This test kit is derived from the SARS-CoV-2 diagnostic test “CDC 2019-Novel Coronavirus (2019-103nCoV) RT-PCR Diagnostic Panel”, developed by the CDC. The kit detects the viral nucleocapsid gene and the human RNase P RNA (as an internal control).
The cycle threshold (Ct) values from the RT-PCR results were used as indicators of the copy number of SARS-CoV-2 RNA in environmental samples -- with lower cycle threshold values corresponding to higher viral copy numbers.
The authors analyzed the samples by grouping them into workplace sources (welfare area, working area, and entrance) and surface types (such as handles, tables/counters, computer devices, sanitizer-dispensers, switches, rails, chairs/benches, and time clocks). The doorknobs/handles were found to have the highest positive frequency rate for the virus.
The authors also present the frequency distribution of the percentage of positive cases for each plant out of the 116 studied.
They observed a decreasing trend of the daily positive rate as the outcome of SARS-CoV-2 preventive measures implemented by the food industry. From this study, it is essential to note that there were individuals contaminated with the virus on the premises despite the screening for symptomatic individuals and the strict environmental decontamination.
Therefore, the asymptomatic and pre-symptomatic individuals presumably infected their surroundings with the virus. This adds to the robust viral transmission.
The following mitigation measures were in place:
- Personal protective equipment
- Health monitoring of the personnel
- Reducing density in otherwise crowded areas
- Frequent sanitation of surfaces
- Closing down or reducing break rooms' capacity
- Contact tracing
- Quarantine of exposed personnel
- Testing
However, the level of workplace contamination due to asymptomatic and pre-symptomatic COVID-19 infections is unknown.
The authors point out that since the RT-PCR test cannot differentiate between infectious and non-infectious virus, this study does not determine the role of the environmental contamination of the SARS-CoV-2.
In this study, environmental monitoring presents SARS-CoV-2 contamination, suggesting that infected individuals are actively shedding the virus. It is found that 62 of the 116 food production facilities had at least one positive sample for SARS-CoV-2. The rate of positive samples in the production facilities ranged from 0-30%.
This study also shows that in the absence of personnel testing, the environmental testing for the SARS-CoV-2 could indicate active human infections.
Our results clearly show that monitoring for the SARS-CoV-19 in workplaces can be a valuable tool in the control of the spread of SARS-CoV-2 virus.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Environmental monitoring shows SARS-CoV-2 contamination of surfaces in food plants; Ziwen Ming, Sukkyun Han, Kai Deng, Youngsil Ha, SungSoo Kim, Enrique Reyes, Yu Zhao, Anatoly Dobritsa, Meiting Wu, Dandan Zhao, David P Cox, Emma Joyner, Hemantha Kulasekara, Seong Hong Kim, Yong Seog Jang, Curtis Fowler, Xing Fei, Hikari Akasaki, Eni Themeli, Alexander Agapov, Dylan Bruneau, Thao Tran, Cameron Szczesny, Casey Kienzle, Kristina Tenney, Hao Geng, Mansour Samadpour. medRxiv 2020.12.10.20247171; doi: https://doi.org/10.1101/2020.12.10.20247171
- Peer reviewed and published scientific report.
Ming, Ziwen, Sukkyun Han, Kai Deng, Enrique Reyes, Youngsil Ha, Sungsoo Kim, Yu Zhao, et al. 2021. “Prevalence of SARS-CoV-2 Contamination on Food Plant Surfaces as Determined by Environmental Monitoring.” Journal of Food Protection 84 (3): 352–58. https://doi.org/10.4315/JFP-20-465. https://www.sciencedirect.com/science/article/pii/S0362028X22068624?via%3Dihub.