We were caring for patients in Massachusetts, which was third among U.S. states for both the overall number of cases of COVID-19 and cases per capita at the time we conducted our study, at a safety-net hospital with the second-highest COVID-19 caseload in the state.
Because of the number of COVID patients we were caring for as a hospital, we had the unique opportunity to see a broad spectrum of neurologic complications early on in the pandemic, and we wanted to document these findings for other clinicians caring for COVID-19 patients in similarly diverse settings.
.jpg)
COVID-19. Image Credit: Stanisic Vladimir/Shutterstock.com
What neurologic complications can COVID-19 lead to?
In our study, we saw a broad range of neurologic complications including strokes, seizures, and altered mental status.
Complications of COVID-19 can involve any part of the nervous system, including the blood vessels, brain, spinal cord, nerves, and muscles.
What are the current ideas behind the mechanisms of neurological complications as a result of COVID-19?
There are a diverse range of mechanisms by which COVID-19 can cause neurologic complications. These complications can result from the body’s immunological response to the virus (e.g. Guillain-Barre syndrome, an autoimmune disorder affecting the nerves), from having a systemic severe illness (e.g. brain injury as a result of insufficient oxygenation), from the increased tendency to form blood clots (e.g. stroke), from worsening of pre-existing neurologic disorders, and possibly from the involvement of the nervous system by the virus itself.
Who was involved in this study and what was found?
This study was conducted in collaboration with wonderful colleagues in the Departments of Neurology and Infectious Diseases at Boston Medical Center, including Drs. Anna Cervantes-Arslanian, Nahid Bhadelia, Davidson Hamer, Lan Zhou, and David Greer.
We focused on the patient population of our hospital, Boston Medical Center, where over half of patients come from households making no more than $25,000 annually, two-thirds identify as racial and/or ethnic minorities, and over one-third are born outside of the U.S. We found a range of neurologic diagnoses, including strokes and seizures, among hospitalized patients with COVID-19.
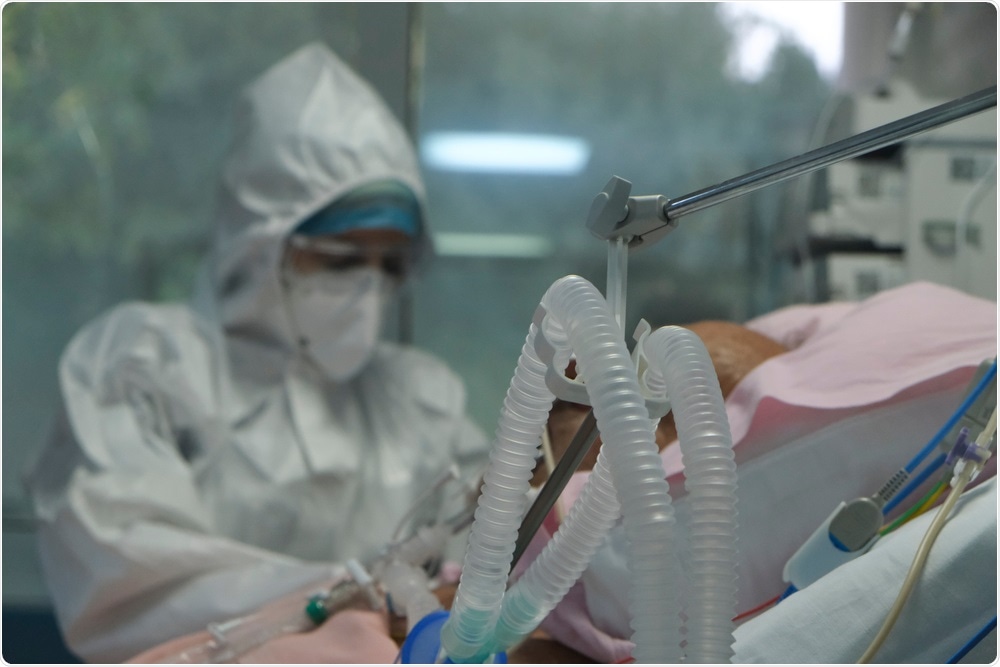
Hospitalized COVID-19 Patient. Image Credit: Alexandros Michailidis/Shutterstock.com
How have your results suggested that neurologic complications may be common in patients of moderate COVID-19 as well as more severe cases?
All of the patients included in our study had neurologic complications, and the majority were not critically ill, suggesting that these complications are not limited just to those patients who require ICU care or a ventilator.
Could certain factors predispose people to having these complications and their severity?
Underlying health conditions may predispose people to having neurologic complications; for instance, patients who have pre-existing chronic kidney disease may be more likely to have some of the neurologic complications of kidney failure we saw in our study.
Is age an important factor affecting these complications?
Although neurologic complications may be more common in older patients, particularly those with predisposing conditions, some studies have found that even younger adults with COVID-19 are at risk for severe neurologic complications such as stroke.
.jpg)
Image Credit: Lemau Studio/Shutterstock.com
Is neurological complication as a result of COVID-19 likely to be more common than generally thought due to cases going undiagnosed?
The fact that we saw neurologic complications even in patients who were not critically ill suggests that even patients with asymptomatic or mild COVID who do not present to medical attention may be at risk of neurologic complications.
What has this research shown about the need for rehabilitation or further help during recovery for some COVID-19 patients?
The survivors in our study had a “moderately severe” disability at the time they left the hospital, and many were discharged to nursing facilities or rehabilitation hospitals.
Although we do not have data on their post-hospital course, this suggests that patients with neurologic complications of COVID-19 are likely to require ongoing rehabilitation, even after they leave the hospital.
What are the next steps for this research?
In the future, our group hopes to follow patients for several years after their initial SARS-CoV-2 infection to look at the risk factors for and trajectory of long-term neurologic complications and recovery.
Where can readers find more information?
Readers can look at the guidance offered by the Centers for Disease Control here: https://www.cdc.gov/coronavirus/2019-ncov/index.html
About Dr. Pria Anand
Dr. Anand practices at Boston Medical Center, where she cares for hospitalized patients with acute neurological disorders and patients with neurological complications of infectious diseases.
She is the chief of the Division of Hospitalist Neurology and an assistant professor within the Division of Neuro-Infectious Diseases at the Boston University School of Medicine.