Coronavirus disease 2019 (COVID-19) is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Infected individuals can have no symptoms, mild symptoms, or severe disease leading to hospitalization and even death.
Anecdotal reports stated that while recovery from symptoms of acute SARS-CoV-2 infection such as fever and chills is uniform, some infected individuals had persistent symptoms such as fatigue and pain long after the period of acute infection. These ‘long-haul’ patients were said to experience something called “long-COVID.” Studies on these post-acute sequelae of SARS-CoV-2 infection (PASC) are currently limited, but the early studies have been able to establish the condition beyond anecdotal reports and have been successful in demonstrating the geographic and sociodemographic diversity of PASC.
However, these early studies have a lot of limitations, including small study groups and short follow-ups. Also, the pathogenesis of PASC is still not clear, though some studies link them to biological abnormalities. As SARS-CoV-2 continues to affect millions of people worldwide, the public health impact of PASC and the need to develop effective methods to prevent or treat the condition need to be studied further.
Analyzing the prevalence of PASC in a rapidly established cohort of COVID-19 patients
Researchers from the US recently studied the prevalence of PASC in a well-characterized cohort of patients to gain insights into the period following acute SARS-CoV-2 infection. The research is posted online to the preprint server medRxiv*.
From April 21 to December 31, 2020, the researchers assembled a cohort of volunteers with documented SARS-CoV-2 RNA-positivity, who were ≥2 weeks past the onset of their COVID-19 symptoms, and those who were able to travel to San Francisco, where the study was conducted. In the case of asymptomatic patients, the chosen volunteers were ≥2 weeks past their first test for SARS-CoV-2.
Participants were either identified on medical center-based health registries and notified or responded to advertisements. One hundred and seventy-nine adults were enrolled in the study. At 4-month intervals, the participants were asked about new or worse physical symptoms compared to the period before COVID-19, mental health signs, and their overall quality of life. The researchers described 4 time periods - 1. Acute illness - 0-3 weeks, 2. Early recovery - 3-10 weeks, 3. Late recovery 1 - 12- 20 weeks, and 4. Late recovery 2 - 28-36 weeks. Blood and oral specimens of the patients were gathered at each visit.
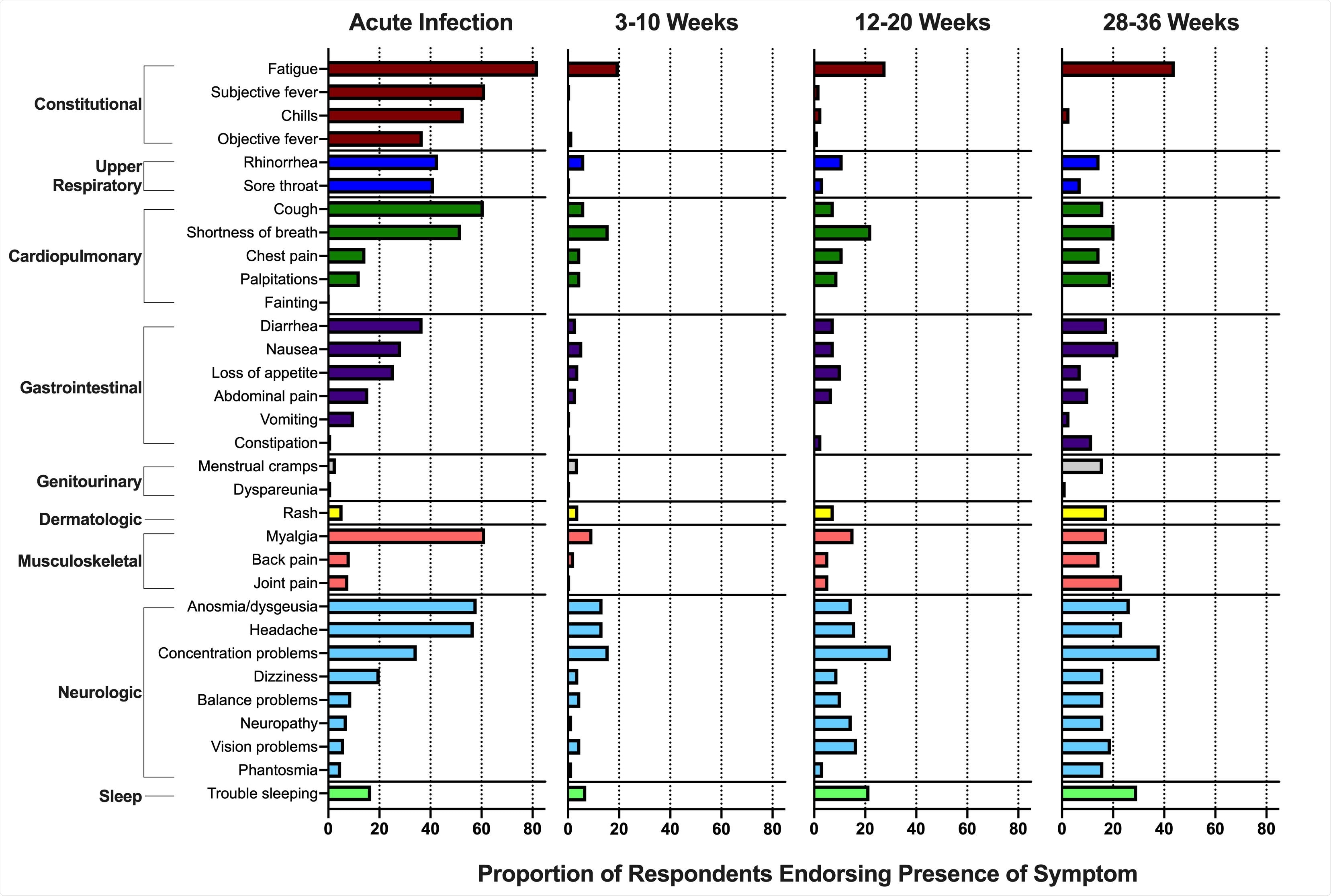
Prevalence of symptoms reported by participants in a study of individuals with SARS-CoV-2 infection during acute infection and three time points in the post-acute phase. Symptoms were limited to those not present prior to the occurrence of COVID-19. Concentration problems refers to “Trouble concentration, trouble with your thinking, or trouble with your memory.” Vision problems refers to “Trouble with vision, for example double vision, blurry vision, or other visual issues.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Patients experienced physical as well as a few mental health issues in the post-acute phase
During acute SARS-CoV-2 infection, 10 patients were asymptomatic, 125 patients were symptomatic but not severe enough to be hospitalized, and 44 patients were symptomatic and hospitalized. During the acute phase, fatigue, myalgia, fever, cough, and anosmia/dysgeusia were the most common symptoms. In the post-acute phase, the most commonly reported symptoms were shortness of breath, fatigue, concentration issues, trouble sleeping, headaches, and anosmia/dysgeusia. Some participants experienced various symptoms other than these, including anxiety, symptoms of depression, post-traumatic stress, difficulties in performing day-to-day activities. Biospecimens from participants were collected at about 600 visits.
“We found substantial interest among affected community residents to participate, and among those who volunteered to enroll, we found many who reported persistent physical symptoms through 8 months following the onset of COVID-19.”
Large and characterized cohorts essential for a better understanding of recovery phase events
As more and more attention turns toward a better understanding of the recovery phase post the acute SARS-CoV-2 infection, large and well-characterized study cohorts will help bring some clarity. In this study cohort, many participants enrolled in the post-acute phase of infection had persistent physical symptoms through the 8 months following COVID-19 onset, which affected overall health.
The researchers conclude, “we have established a cohort of participants enrolled in the post-acute phase of SARS-CoV-2 infection. We found substantial interest among affected community residents to participate, and among those who volunteered to enroll, we found many who reported persistent physical symptoms through 8 months following the onset of COVID-19. The convenience nature of our sampling — like many other nascent cohorts of PASC — precludes estimation of the population-level prevalence of these persistent symptoms, but it will allow for investigation of the duration of symptoms conditioned upon their occurrence. Importantly, the presence of both participants without symptoms and ample biological specimens will also allow for analytical work to study the pathogenesis of PASC, which we anticipate will burgeon as the field begins to investigate mechanisms that will inform prevention and treatment.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Rapid implementation of a cohort for the study of post-acute sequelae of SARS-CoV-2 infection/COVID-19, Michael J. Peluso, J. Daniel Kelly, Scott Lu, Sarah A. Goldberg, Michelle C. Davidson, Sujata Mathur, Matthew S. Durstenfeld, Matthew A. Spinelli, Rebecca Hoh, Viva Tai, Emily A. Fehrman, Leonel Torres, Yanel Hernandez, Meghann C. Williams, Mireya I. Arreguin, Jennifer A. Bautista, Lynn H. Ngo, Monika Deswal, Sadie E. Munter, Enrique O. Martinez, Khamal A. Anglin, Mariela D. Romero, Jacqueline Tavs, Paulina R. Rugart, Jessica Y. Chen, Hannah M. Sans, Victoria W. Murray, Payton K. Ellis, Kevin C. Donohue, Jonathan A. Massachi, Jacob O. Weiss, Irum Mehdi, Jesus Pineda-Ramirez, Alex F. Tang, Megan Wenger, Melissa Assenzio, Yan Yuan, Melissa Krone, Rachel L. Rutishauser, Isabel Rodriguez-Barraquer, Bryan Greenhouse, John A. Sauceda, Monica Gandhi, Priscilla Y. Hsue, Timothy J. Henrich, Steven G. Deeks, Jeffrey N. Martin, medRxiv, 2021.03.11.21252311; doi: https://doi.org/10.1101/2021.03.11.21252311, https://www.medrxiv.org/content/10.1101/2021.03.11.21252311v1
- Peer reviewed and published scientific report.
Peluso, Michael J, J Daniel Kelly, Scott Lu, Sarah A Goldberg, Michelle C Davidson, Sujata Mathur, Matthew S Durstenfeld, et al. 2021. “Persistence, Magnitude, and Patterns of Postacute Symptoms and Quality of Life Following Onset of SARS-CoV-2 Infection: Cohort Description and Approaches for Measurement.” Open Forum Infectious Diseases 9 (2). https://doi.org/10.1093/ofid/ofab640. https://academic.oup.com/ofid/article/9/2/ofab640/6472960.