At the moment, vaccines represent the most effective public health intervention at our disposal against the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), a causative agent of the current COVID-19 pandemic. More specifically, eight vaccines are currently approved for full use, with an additional seven that are authorized for early or limited use on a global scale.
However, even with the approval of multiple vaccine solutions that are being dispersed across different regions worldwide, roll-out has been rather slow in general. Some countries have problems meeting their anticipated deadlines, and vaccination rates differ significantly across countries.
Previous studies targeting specific subgroups in a specific population, including elderly individuals, showed evidence of decreased morbidity and deaths due to COVID-19. Furthermore, previous theoretical work provided some credence to unequal vaccine allocations, but realistic assumptions about population heterogeneity and contact structure question that idea.
Hence, there is a potentially conflicting message for policymakers when tackling resource constraints and considering optimal vaccine allocation decisions. This is why a US research group, led by Dr. Keya Joshi from the Harvard TH Chan School of Public Health, decided to further explore these issues within the context of the COVID-19 pandemic.
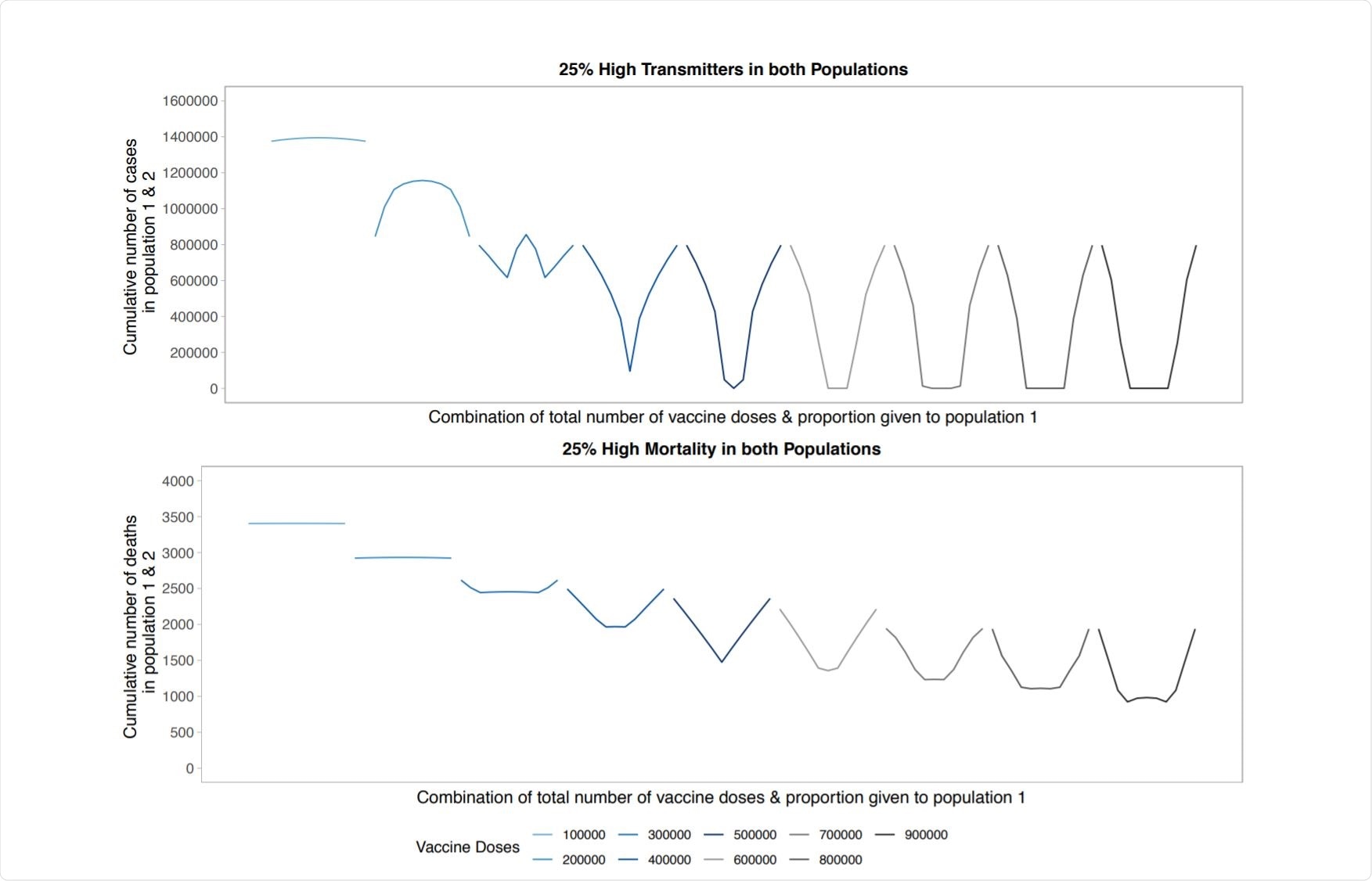
Study Results. Image Credit: https://www.medrxiv.org/content/10.1101/2021.06.18.21259137v1.full.pdf

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Models informed by the literature
By using a so-called susceptible-exposed-infectious-recovered (SEIR) model, these researchers examined optimal SARS-CoV-2 vaccine allocation decisions across two populations – taking into account the impact of population size, ongoing vaccine roll-out, underlying immunity, as well as heterogeneous population risk structure.
Their work heavily relied on the existing scientific literature by initially examining allocation decisions in the straightforward scenario of two indistinguishable, non-interacting populations without any evidence of underlying immunity against SARS-CoV-2.
In short, for each simulation, the research group has calculated the cumulative number of infections and deaths from the deterministic SEIR model at the end of the epidemic. Finally, they have assessed the robustness of their results by varying vaccine characteristics and connections between populations to be more representative of the current pandemic.
Comparative performance of vaccine allocation strategies
The study has shown that for the simple situation of two non-interacting, identically sized populations the most optimal approach would be equal allocation strategies in cases of very high quantities of vaccine, relative to the population size. Conversely, with few doses, basically all strategies yield comparable results.
More specifically, in scenarios that consider heterogeneous population risk, targeting high-risk individuals (either high-transmitters or those at increased risk of death) as an initial step yields more equitable resource allocations between populations.
In addition, both the speed and timing of vaccine roll-out has a paramount role in minimizing the final breadth of the epidemic. The final size is actually minimized when the roll-out speed is increased, which means vaccinating a larger proportion of the population every day.
The study also states that for vaccine stockpiles larger than 500 thousand doses, the feasible vaccination impact is much more dependent on the speed and timing of vaccine roll-out rather than on the total number of doses available to the population.
Maximizing the benefit from each dose
With vaccine stockpiles that are still gravely constrained, there is a need for swift allocation decisions. Likewise, due to the sheer magnitude of SARS-CoV-2 spread and impact, further economic and political constraints also play a significant role in most allocation decisions.
Mathematical modeling can provide insight into optimal allocation strategies that maximize the benefit from each dose. Conclusions from such models should be balanced with ethical considerations on the fairness of allocation that also minimize disparities in access”
And indeed, this study reveals key principles that should be taken into account when designing realistic and implementable allocation strategies. Nonetheless, future modeling work on SARS-CoV-2 vaccination approaches is needed that will follow the roll-out of multiple vaccine candidates.
Such studies should also scrutinize the effects of vaccines on hospitalization reduction and preserving hospital capacity, with indirect implications for COVID-19 mortality rates, but also other diseases beyond the direct prevention of infection in high-risk populations.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources