
 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Background
The ongoing COVID 2019 (COVID-19) pandemic has led to over 525 million confirmed-SARS-CoV-2 infections and 6.28 million deaths globally. According to available data, roughly half of COVID-19 patients experienced at least one long-term symptom continuing more than a year after the infection. Long COVID, also called the post-COVID-19 condition, is a post-acute sequela of SARS-CoV-2 infection. The frequent symptoms of long COVID consisted of fatigue, dysosmia, and shortness of breath.
A prospective longitudinal observational study demonstrated that the proportion of acute-phase symptoms differed between individuals with SARS-CoV-2 Delta and Omicron infections. Sore throats were more prevalent in Omicron than Delta, whereas loss of smell was less frequent in Omicron versus Delta. Nevertheless, there have been no epidemiological reports of post-COVID-19 conditions caused by the SARS-CoV-2 Omicron variant.
About the study
The present cross-sectional, single-center study aimed to explore and compare the occurrence of the post-COVID-19 condition associated with the SARS-CoV-2 Omicron variant and other viral strains.
The authors conducted a telephonic interview for Japanese individuals who recovered from COVID-19-linked with Omicron (Omicron cohort) and assessed patients infected with other SARS-CoV-2 strains using self-reported questionnaires (control group). They collected written informed consent from subjects in the self-reported survey group and oral informed consent from the telephonic survey cohort.
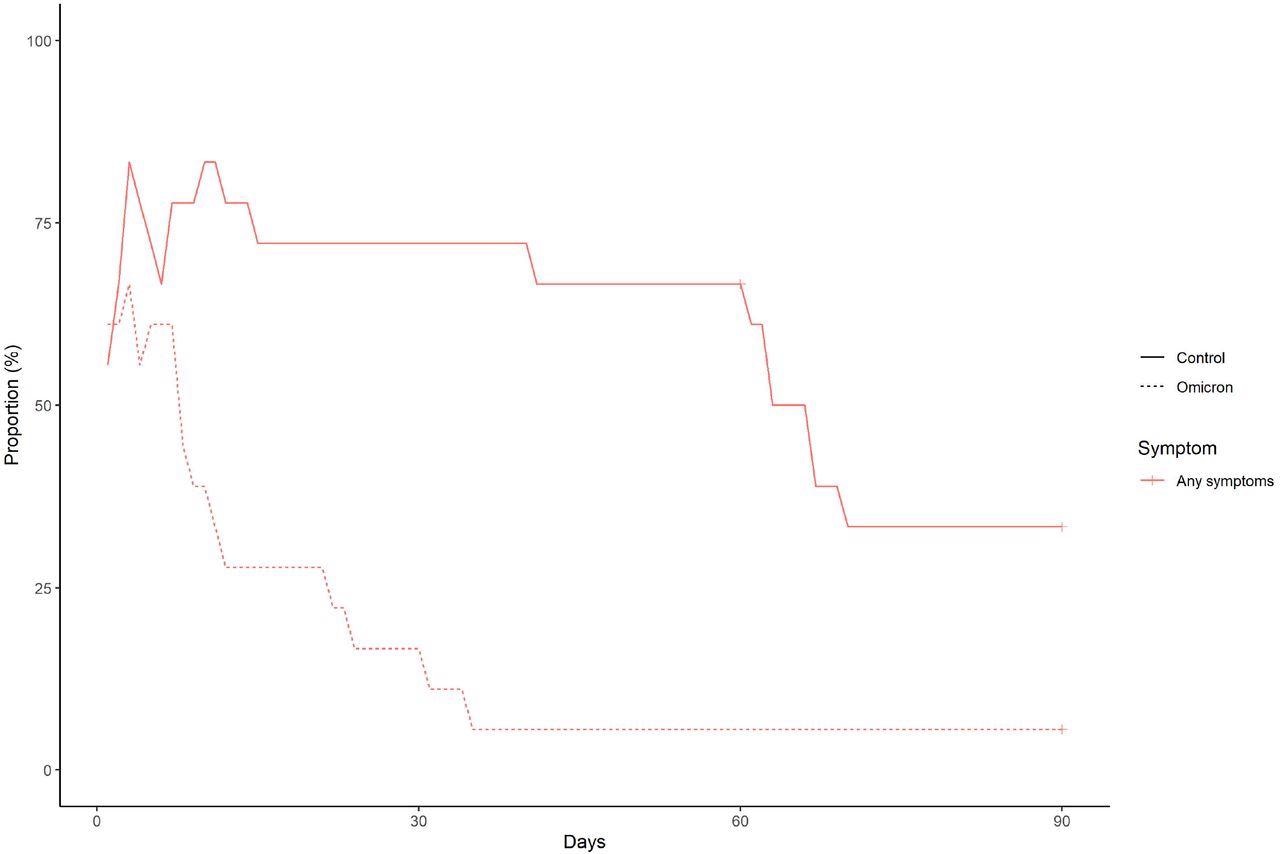
The frequency and duration of at least one symptom in the Omicron group and the control group after matching
Patients admitted to the National Center for Global Health and Medicine (NCGM) with COVID-19 between 1 December 2021 and 9 February 2022 were requested to participate in telephonic interviews. These patients tested negative for the L452R mutation and positive for the E484A mutation of SARS-CoV-2, as determined by reverse transcription-polymerase chain reaction (rtPCR). Further, patients who died while in the hospital were not included in the research. COVID-19 convalescent individuals who visited the NCGM's outpatient facility of the Disease Control and Prevention Center from February 2020 to November 2021 were included in the control cohort.
The scientists gathered information on the patients' characteristics, the acute-phase SARS-CoV-2 infection, and the occurrence and duration of COVID-19-associated symptoms. A SARS-CoV-2-related symptom that persisted at least two months within three months of the initiation of COVID-19 was classified as a post-COVID-19 condition in this investigation. After completing propensity score matching, the team evaluated and compared the incidence of the long COVID-19 in both cohorts.
Results
The study results indicated that the authors interviewed 53 out of 128 patients with post-Omicron infection status and received 502 replies in the control cohort. Upon matching, 18 subjects in both the control and Omicron groups exhibited better covariate balance of the female sex, older adult, COVID-19 vaccination status, and obese patients. There were no notable variances in the prevalence of each post-acute SARS-CoV-2 symptom among the two cohorts. Besides, 5.6% and 55.6% of patients had a minimum of one post-acute COVID-19 symptom in the Omicron and control cohorts, respectively.
The team found that 28.3%, 84.9%, and 56.6% of Omicron patients experienced a runny nose, fever, and sore throat, respectively, yet none of these symptoms lasted more than two months within three months following the disease's beginning. They stated that describing the clinical course of Omicron infection was vital for public health since it informs the physicians and the public about the symptoms to monitor. It also helps them understand the possible impacts of potential SARS-CoV-2 variants of concern (VOCs).
Moreover, hair loss, dysosmia, and dysgeusia were seen in 3.8%, 5.7%, and 13.2% of individuals with Omicron infection, respectively. These findings can assist raise knowledge about which symptoms were more frequent with the Omicron mutant, allowing for rapid diagnosis and limiting COVID-19 spread.
Conclusion
To conclude, the study findings showed that the prevalence of long COVID did not differ significantly between the Omicron and control groups, albeit the post-Omicron COVID-19 conditions were less common than other SARS-CoV-2 strains. Furthermore, the Omicron group had a considerably lower number of patients with a minimum of one post-acute SARS-CoV-2 symptom than the control cohort.
The authors stated that although the prevalence rate in the Omicron group may be lower, the exact number of individuals experiencing the post-COVID-19 condition might be higher due to the vast number of persons infected with Omicron internationally. Hence, they suggested that more studies with a large sample size were required to explore the accurate epidemiology of the Omicron-linked long COVID condition and its influence on social productivity and health-associated quality of life.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Post COVID-19 condition of the Omicron variant of SARS-CoV-2; Shinichiro Morioka, Shinya Tsuzuki, Michiyo Suzuki, Mari Terada, Masako Akashi, Yasuyo Osanai, Chika Kuge, Mio Sanada, Keiko Tanaka, Taketomo Maruki, Kozue Takahashi, Sho Saito, Kayoko Hayakawa, Katsuji Teruya, Masayuki Hojo, Norio Ohmagari. medRxiv preprint 2022, DOI: https://doi.org/10.1101/2022.05.12.22274990, https://www.medrxiv.org/content/10.1101/2022.05.12.22274990v1
- Peer reviewed and published scientific report.
Morioka, S., S. Tsuzuki, M. Suzuki, M. Terada, M. Akashi, Y. Osanai, C. Kuge, et al. 2022. “Post COVID-19 Condition of the Omicron Variant of SARS-CoV-2.” Journal of Infection and Chemotherapy 28 (11): 1546–51. https://doi.org/10.1016/j.jiac.2022.08.007. https://www.jiac-j.com/article/S1341-321X(22)00233-1/fulltext.