The global rise in obesity and related health issues remains unabated despite numerous weight-loss initiatives. A key player might be changes in intestinal barrier function and gut microbiota, leading to increased bacterial toxins in the bloodstream (endotoxemia). This results in inflammation due to the Toll-like receptor 4 pathway. Such inflammation from diet-induced endotoxemia has been linked to specific dietary components, like saturated fats and sugars. Although the World Health Organization (WHO) advises limiting sugar intake, its consumption remains high in many countries, with sugar-sweetened beverages as a prime source. Replacing these with low-calorie sweeteners may offer health benefits, but long-term consumption could lead to weight gain and altered gut microbiota. One popular sweetener, sucralose, poses concerns for long-term glucose tolerance and immune function. Further research is needed to understand the role of different sweeteners on intestinal barrier function and endotoxemia.
 Study: Acute Intake of Sucrose but Not of the Intense Sweetener Sucralose Is Associated with Post-Prandial Endotoxemia in Healthy Young Adults—A Randomized Controlled Trial. Image Credit: Tatjana Baibakova / Shutterstock
Study: Acute Intake of Sucrose but Not of the Intense Sweetener Sucralose Is Associated with Post-Prandial Endotoxemia in Healthy Young Adults—A Randomized Controlled Trial. Image Credit: Tatjana Baibakova / Shutterstock
About the study
Amidst the complications of the Coronavirus Disease 2019 (COVID-19) pandemic, the research was limited to immediate intervention. Registered on ClinicalTrials.gov (NCT04788680) from 2021 to 2022, the present study involved eighteen healthy non-smokers within a specified Body Mass Index (BMI) range; eleven completed the study, while seven withdrew for various reasons, including COVID-19 infections.
Participants, having refrained from consuming intense sweeteners three weeks prior, were given dietary adjustments based on recommendations by the German, Austrian, and Swiss (D-A-CH) nutrition societies. On intervention days, participants were provided with a light breakfast accompanied by beverages containing varying concentrations of sucrose, sucralose, or a combination thereof, and blood samples were taken at intervals to evaluate their responses.
To further analyze the results, blood pressure, blood sugar levels, and lipid profiles were routinely assessed using various tests and measures, and a limulus amebocyte lysate assay was employed to determine the beverages' impact on bacterial endotoxin levels in participants. Additionally, Enzyme-Linked Immunosorbent Assay (ELISA), in-vitro tests on Caco-2 cells, and ex-vivo everted gut sac experiments were conducted, with statistical significance established at a p-value < 0.05.
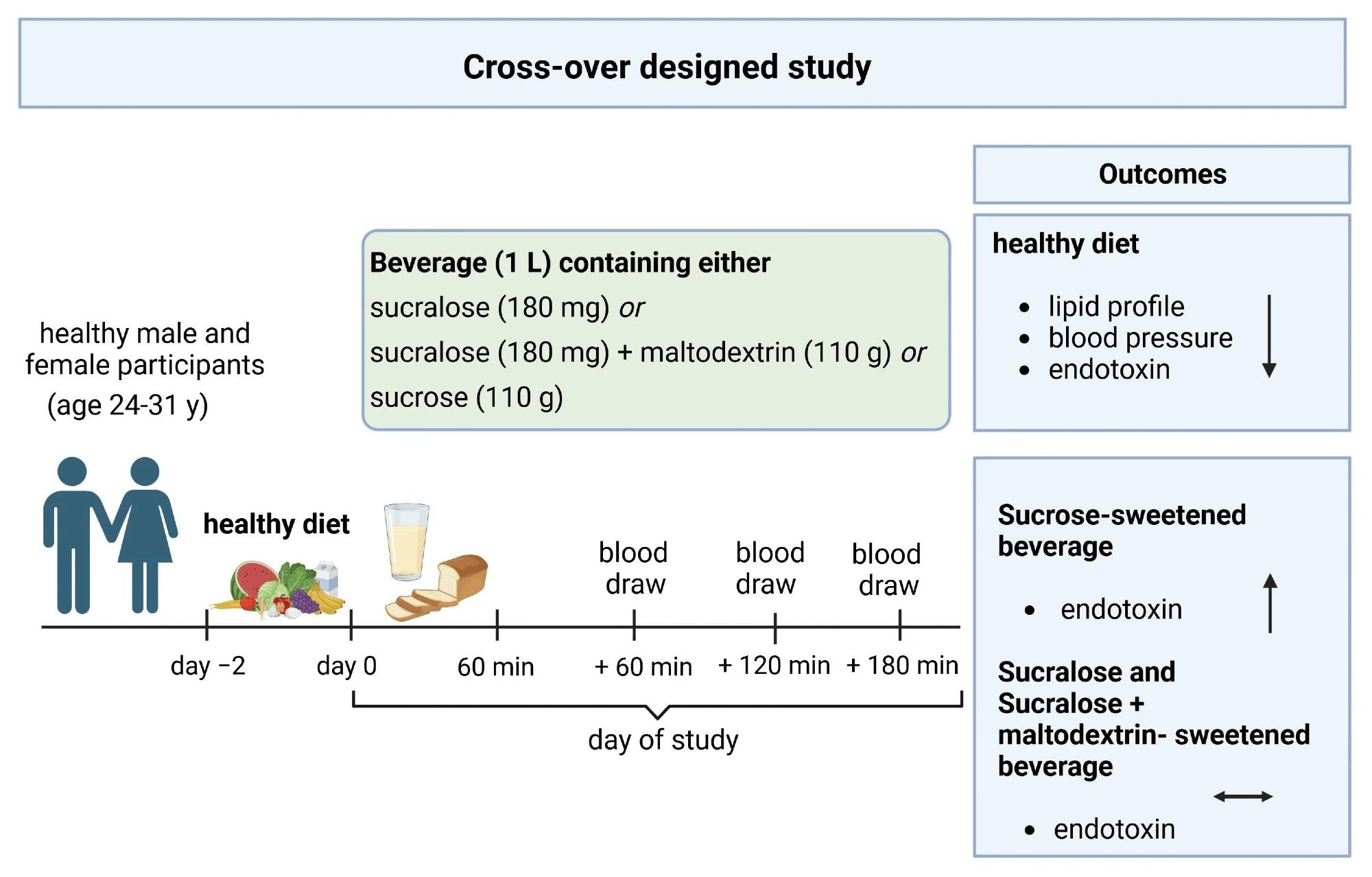 Graphical Abstract
Graphical Abstract
Study results
Of the initial 18 healthy, normal-weight men and women who enrolled in the study, only 11 completed it, while seven dropped out due to various reasons, including COVID-19 infections, relocations, or personal matters. The baseline details of these 11 participants, which included their anthropometry, routine laboratory results, and dietary intake, were noted. Subsequently, participants were provided with a nutritionally balanced, isocaloric diet based on D-A-CH recommendations. During the standardization period of two days, where the study team provided all consumables except plain water, there were no significant changes in the participants' anthropometric parameters. However, most experienced a decrease in their total fat and protein intake and saw an uptick in their carbohydrate, fiber, fruit, and vegetable consumption.
There were noticeable shifts in some serum parameters. Triglyceride levels went down approximately by 11 mg/dL, total cholesterol was reduced by around 11 mg/dL, High-Density Lipoprotein (HDL) cholesterol decreased by about 2 mg/dL, and Low-Density Lipoprotein (LDL) cholesterol dropped by roughly 7 mg/dL. Moreover, there was a notable decline in the systolic blood pressure and bacterial endotoxin levels in the serum after the nutritional standardization phase.
After consuming the sucrose-sweetened beverage, a significant rise in plasma endotoxin levels was observed compared to baseline data. This spike was not observed when participants consumed beverages sweetened with sucralose or a blend of sucralose and maltodextrin. Specifically, 120 minutes after consuming the sucrose-sweetened drink, bacterial endotoxin levels in the plasma were markedly higher than after the intake of the sucralose-sweetened alternative.
To determine if the increased bacterial endotoxin levels post-sucrose consumption were related to changes in intestinal barrier function, a model using differentiated Caco-2 cells was employed. When these cells were treated with sucralose before being exposed to bacterial endotoxin, there was no significant change in bacterial endotoxin levels in the system. However, when the cells were treated with sucrose, bacterial endotoxin levels were notably higher. Furthermore, the intestinal fatty acid binding protein (iFABP) concentration, previously indicated as a sign of intestinal barrier disruption, only increased in cells treated with sucrose, not those exposed to sucralose.
Additionally, when testing on small intestinal tissue with sucrose, there was a noticeable increase in xylose permeation. Conversely, sucralose did not have the same effect, and the xylose permeation remained unchanged.
Conclusions
To summarize, intense sweeteners, frequently used as sugar substitutes, may offer health benefits. However, it has been found that consuming 1 liter of a beverage sweetened with sucrose significantly increases bacterial endotoxin levels in the blood, an effect not observed with drinks sweetened with sucralose. Some evidence suggests that fructose, a component of sucrose, might be the cause, possibly by affecting intestinal flora. Contrasting results in rodent studies underscore potential species differences and the influence of study durations, while a short-term dietary adjustment in participants led to reduced endotoxin levels and enhanced health markers.