A study published in the journal Science Translational Medicine describes the development and validation of an octopus sucker-inspired buccal mucosa suction patch as a novel drug delivery system.
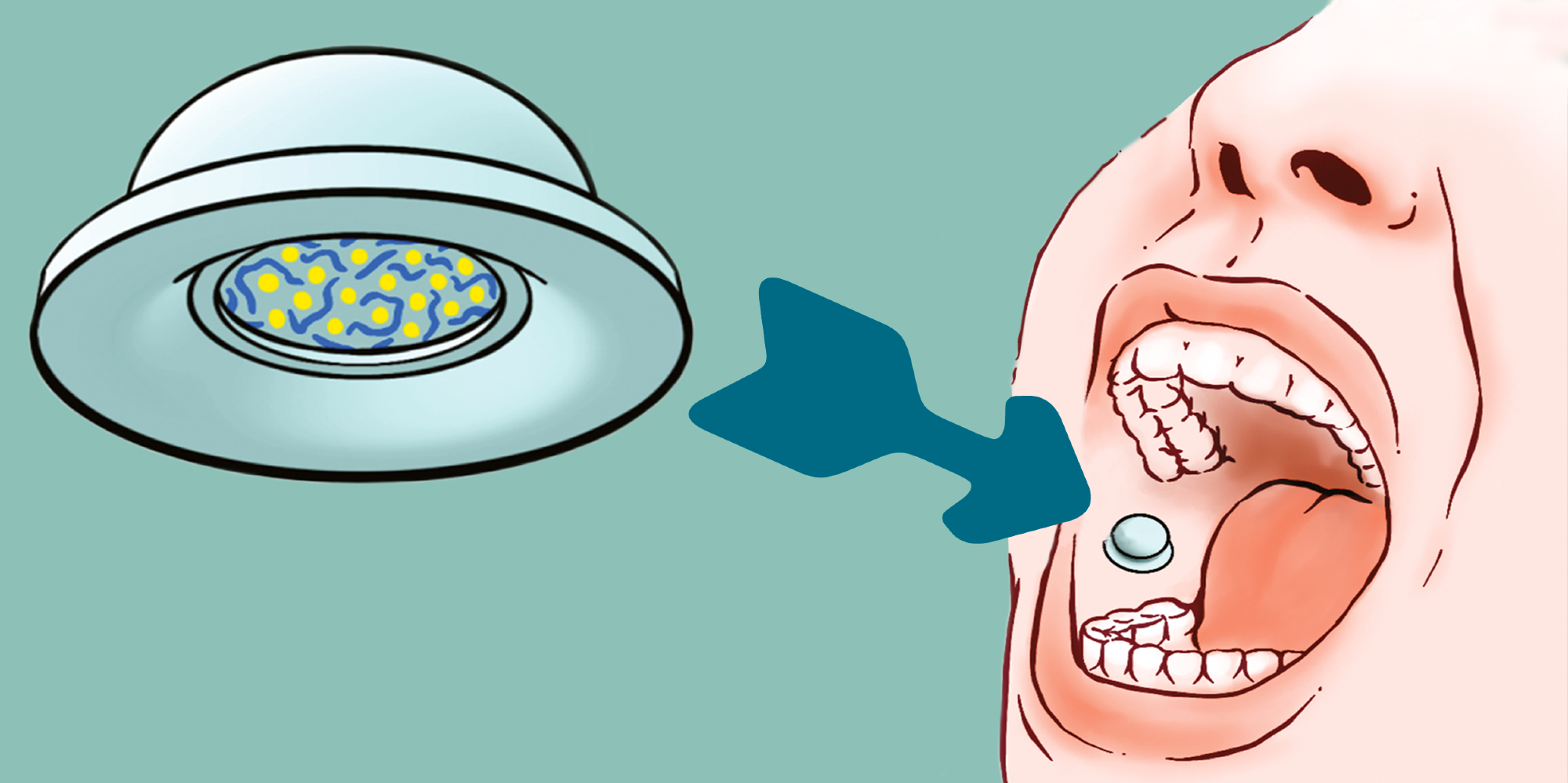 The suction cup contains active ingredients and can be pressed onto the lining of the check with two fingers. Image Credit: Luo Z et al. 2023
The suction cup contains active ingredients and can be pressed onto the lining of the check with two fingers. Image Credit: Luo Z et al. 2023
Background
Optimal drug delivery systems are crucial in improving drug absorption, increasing drug bioavailability, reducing drug-related side effects, increasing patient compliance, and reducing healthcare costs. However, designing strategies for effective drug absorption through biological barriers remains a challenging task in the field of pharmaceutical sciences.
Proteins, peptides, and other macromolecular drugs are not absorbed optimally through the gastrointestinal (GI) tract and thus mostly require intravenous administration. Even permeation-enhancing formulas often fail to increase the bioavailability of orally administered macromolecular drugs considerably.
To improve systemic absorption of macromolecular drugs, scientists in China and Switzerland have developed a noninvasive drug delivery platform that combines mechanical stretching of the buccal mucosa with chemical permeability enhancers. Inspired by the morphological characteristics of octopus suckers, scientists have developed this buccal mucosa suction patch.
The central hypothesis behind this innovation is to impose a mechanical force on the buccal mucosa to transiently loosen up its cellular organization, increase inter-cellular spaces, and subsequently improve drug permeability. The scientists believe that mechanical stretching and permeability enhancers would work synergistically to increase drug diffusion into the highly vascularized tissue, which in turn would facilitate systemic drug absorption.
Suction patch design
The buccal mucosa suction patch was designed based on the structural features of octopus suckers. The patch size was kept similar to commercially available mucoadhesive tablets for easy and comfortable delivery. The dome-shaped structure of the patch was designed to create mechanical pressure. The dome-shaped cavity inside the patch could incorporate more than 50 mg of a drug.
The suction patch showed desirable adhesion performance on porcine buccal mucosa. Further testing showed that the patch causes more than a 250% increase in the tissue surface area due to mechanical stretching.
The histological analysis of the buccal mucosa showed that the patch is able to locally and non-invasively disrupting the epithelial layer without causing any damage to the outermost surface of the epithelium. The examination of the permeability enhancer-loaded patch showed that the permeability enhancer merely works at the mucosal surface in the absence of patch-induced mechanical stretching.
The experiments conducted by applying patches on the porcine buccal mucosa in combination with different permeability enhancers showed that mechanical stretching and permeability enhancers should act synergistically to facilitate effective penetration of the epithelial layer.
Pharmacokinetic study
A comparative analysis of peptide drug (desmopressin) delivery through buccal patches, intravenous injection, and oral route was conducted in dogs. The findings revealed that the plasma concentration of desmopressin increases gradually over the 3-hour period of patch application. The peak level was achieved one hour after the removal of patches. The absolute bioavailability of the drug was comparable to that observed for orally administered desmopressin tablets.
A 3-hour application of the patch with a permeability enhancer caused a 150-times higher plasma concentration of desmopressin compared to that observed after oral administration of desmopressin.
Safety profile
A 3-hour application of the patch with a permeability enhancer caused swelling of the buccal mucosa, which fully resolved after a day or a week of application, depending on the type of permeability enhancer used. A 30-minute application, on the other hand, caused only slight swelling, which fully resolved within 6 – 24 hours after the patch removal.
The biopsy findings revealed that the integrity of the buccal mucosa was fully restored 24 hours after the patch removal.
Human study
To study patient acceptability of the buccal patch, 40 healthy adult volunteers were asked to self-apply drug- and permeability-enhancer-free patches on their buccal mucosa for 30 minutes.
More than 92% of the volunteers reported the application as generally comfortable to only mildly uncomfortable. Only minimal tissue alteration was caused by the patches during the application. About 75% of the volunteers reported not feeling anything unusual one hour after the patch removal. One day after the removal, they could not distinguish between normal and patch-applied mucosa.
The majority of the volunteers reported that they highly prefer buccal patches for drug delivery over intravenous injection.
Study significance
The study finds that octopus sucker–inspired buccal mucosa suction patches might be regarded as an alternative delivery option for macromolecular drugs.