The molluscum contagiosum virus, the causative agent of molluscum contagiosum, enjoys a global distribution with susceptibility pockets in tropical climates, probably facilitated by increased skin moisture. Although children and sexually active adults are primarily affected by this viral illness, immunocompromised patients (such as those infected by human immunodeficiency virus) are exceptionally vulnerable.
The typical mode of transmission is skin-to-skin contact, either sexually or non-sexually, or via fomites and autoinoculation. Therefore a basic knowledge of this virus, the disease epidemiology and its clinical presentation is pivotal for taking adequate protective measures.
Papules as Primary Lesions
Molluscum contagiosum typically presents as an eruption of round, semi-transparent and shiny papules of dense, elastic consistency, without any systemic manifestations. Those papules are characterized by clear borders, smooth surface and central concavity (due to the latter they are also known as umbilicated lesions).
The size of the papules (also known as mollusca) may vary between 2 and 6 millimeters. They are usually between 2 and 20 in number, and not prone to mixing or grouping (albeit sometimes they can mix to form a giant lesion). Their color varies from flesh and yellow, to dark red with a specific violet shade. These umbilicated and dome-shaped papules have a white curd-like core mass that may be expressed.
Although any area may be involved, the preponderant sites are the abdomen, genitals and inner thighs of sexually active adults, as well as the face, trunk and limbs of children. The life of a lesion is usually less than two months, although they can occasionally last for several years.
The most common scenario is a self-limited disease, which means all papules disappear in a 6- to 9 month span. The resolution of a lesion is usually heralded by dermatitis around it, and in approximately 10 percent of all lesions there is also a surrounding eczema.
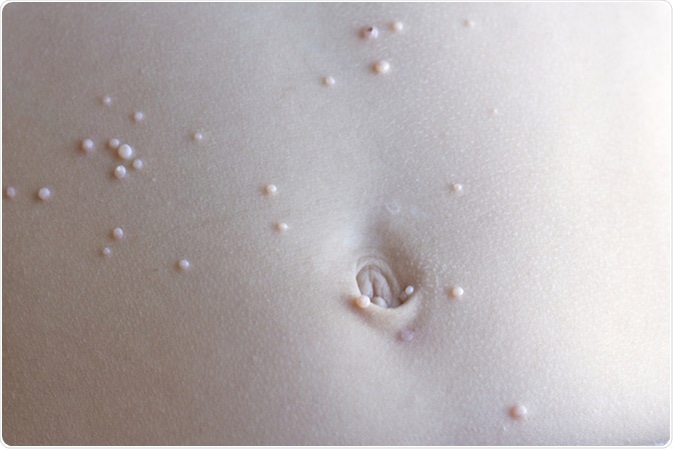
Molluscum contagiosum. Image Credit: Jarrod Erbe / Shutterstock
Long-Term Effects and Complications
The most commonly observed complication of molluscum contagiosum is a secondary bacterial infection that results in pustule formation. Such lesions pose a danger of rupturing into the dermis (i.e. the thicker inner layer of the skin) with a suppurative inflammatory response akin to an abscess. This is especially when the putative bacterial pathogen is Staphylococcus aureus.
On the other hand, a ubiquitous (and highly drug-resistant) environmental microorganism Pseudomonas aeruginosa can instigate the formation of necrotizing cellulitis, which is an unusual complication in HIV-infected individuals. Of note are also lesions on eyelids that are often associated with papillary or follicular conjunctivitis.
Oral lesions may also arise in some long-term cases of the disease and are quite hard to distinguish from those of other diseases. Thus they are usually diagnosed during routine dental visits. The pathognomonic feature is a painless papillomatous mass that is formed from pink nodules.
Patients infected with HIV, those that developed acquired immunodeficiency disorder (AIDS) and organ transplant recipients are more prone to developing giant lesions (i.e. more than 15 millimeters in diameter), as well as a larger number of lesions recalcitrant to standard treatment regimens.
In the differential diagnosis of molluscum contagiosum physicians should always consider plain warts, basal-cell carcinoma, keratoacanthoma, and other infectious states (such as cryptococcosis and histoplasmosis), while vaginal syringomas and condylomata acuminata should be excluded when encountering genital lesions.
References:
- https://www.ncbi.nlm.nih.gov/pubmed/28521677
- https://www.ncbi.nlm.nih.gov/pubmed/12639455
- https://www.ncbi.nlm.nih.gov/pubmed/23972567
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3645633/
- https://www.cdc.gov/poxvirus/molluscum-contagiosum/long-term-effects.html
- Dhar JK. Molluscum Contagiosum. In: Kumar B, Gupta S, editors. Sexually Transmitted Infections, Second Edition. Elsevier Health Sciences, 2012; pp. 374-379.
- Liu D. Molluscum Contagiosum Virus. In: Liu D, editor. Molecular Detection of Human Viral Pathogens. CRC Press, Taylor & Francis Group, 2011; pp. 1001-1008.
Further Reading
Last Updated: Feb 27, 2019