Sepsis is brought on by infection with a pathogen, to which the body responds excessively and perpetuates a systemic immune response.
Many infections leading to sepsis are due to bacteria, but viral causes are increasing. Among these is the influenza virus, which effects people in epidemics worldwide.
Influenza
There are several subcategories and strains of influenza virus which each have different pathology. One of those subcategories is type A, which can affect both animals and humans and can trigger large pandemics, such as the swine flu.
There is also type B, which do not cause epidemics or pandemics but are still capable of serious damage, and type C, which are milder than type A and B.
One of the main preventative measures against sepsis is to stop infection of pathogens by hygiene practices and vaccines.
A large problem with influenza and influenza-induced sepsis is that it is a set of viruses which cannot be vaccinated against. The viruses are not static, meaning they are constantly mutating and changing into new viruses.
This means they are not recognized by your immune system, given that the virus has changed sufficiently.
Influenza infections can trigger abnormal immune responses, which lead to endothelial damage, deregulation of coagulation, and eventually changes in microvascular permeability, tissue edema, and shock. However, most people manage to recover from influenza infections.
Life-threatening complications include secondary infections that occur as a result of the flu. It is through these that many indirectly develop sepsis because of influenza.
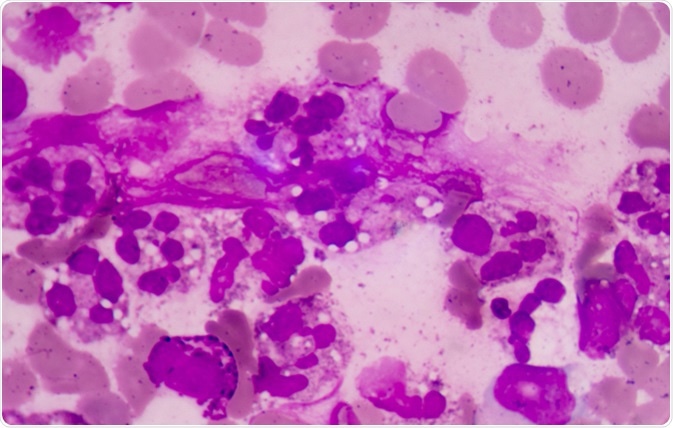
Abnormal neutrophil in pleural fluid smear. Sepsis or septicaemia is a life-threatening illness. Presence of numerous bacteria in the blood, causes the body to respond in organ dysfunction. Image Credit: Toeytoey / Shutterstock
From Influenza to Sepsis
Sepsis and influenza share many pathways in the body. For example, certain influenza strains stimulate Toll-like receptor 4 (TLR4) and eventually lung damage by interleukin 6 (IL-6), both of which are highly implicated in sepsis.
In some strains these pathways, which are associated with the immune system, can directly lead to severe sepsis. They can also create a vulnerability to other infections as the immune system is impaired.
One of the most common pathways through which influenza translates into sepsis is by a secondary infection of pneumonia.
A 2009 study on a cohort of Americans who had been afflicted with the pandemic influenza A virus H1N1 found that those who had influenza pneumonia had a six-fold higher chance of developing bacterial sepsis.
In general, influenza A and B viruses are known to make patients more vulnerable to bacterial infections, in particular S. pneumoniaewhich causes pneumonia. This was especially common during influenza pandemics, such as the Spanish flu in 1918.
1st WSC - Lessons Learned from the 1918 Spanish Influenza by David Morens
The mechanisms through which influenza creates an environment susceptible to bacterial infection is only partly understood.
The influenza virus alters the lungs to increase susceptibility to bacterial adherence, invasion and initiation of disease.
Adherence is made possible by replication of the virus, which uncovers the respiratory epithelium and thereby revealing the basement membrane that the bacteria can adhere to.
Adhesion and invasion are further fostered by pro-inflammatory cytokines triggered by the influenza virus, which may upregulate platelet-activating factor receptors (PAFr). This provides a receptor for pneumococcus bacteria, for instance, to adhere to and invade.
The initiation of the disease is facilitated by damaged antibacterial defense mechanisms. The damage is brought on by the influenza virus, which increases apoptosis of neutrophils, dysfunction of neutrophils and monocytes, depressing chemotaxis and suppressing phagocytosis.
Treatment Challenges
Sepsis induced by influenza can be complicated, as the viral infection or secondary bacterial infections can confound with or alter the way patients respond to typical sepsis treatment.
For example, using steroids as immunosuppressants is used as a treatment against sepsis and ARDS, an implicated respiratory disorder.
However, in cases of influenza when immunity is impaired, using steroids to further repress the immune system can be harmful.
Further Reading
Last Updated: Sep 9, 2018