A coloboma is an eye abnormality present at birth that results from the absence of some tissues in certain parts of the eye. One or both eyes may be affected.
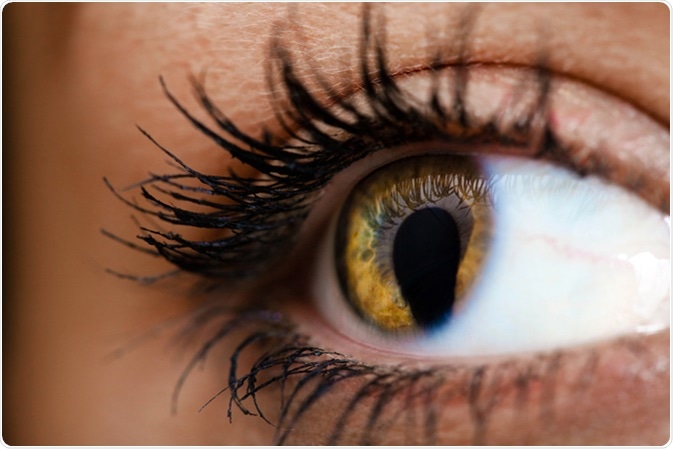
Female eye with Coloboma or cat eye. Image Credit: Shvaygert Ekaterina.
The most obvious presentation of a coloboma is as a notch or a gap in some part of the eye, whether that be the iris, the retina, the choroid, or the optic nerve. Colobomas of the eyelids also occur but have a different route of origin.
There are three types of colobomas:
- those occurring in microphthalmic eyes, where the eyeball is very small; this may cause severe visual impairment
- those with microcornea but with normal axial length
- isolated coloboma
Most ocular colobomas occur in the lower and inner part of the eye, where the optic fissure closes last during development. Depending on the timing and etiology of the developmental disruption, any of the tissues of the eye may be affected. This includes colobomas of the cornea, the iris, the choroid, lens, retina and optic disc.
The tissue affected and the size of the defect will determine whether the person’s vision is impacted or not.
Syndromic colobomas
There are many syndromes in which a coloboma in association with other developmental defects of, eye, brain, or multiple organ systems. The congenital defects most commonly associated with colobomas are cleft lip, bony defects, horseshoe kidney, and genital defects. These are called syndromic colobomas, in contrast to isolated or nonsyndromic colobomas.
Eye abnormalities may include cataracts (when the lens becomes opaque), glaucoma (when the pressure in the eye is abnormally high), short sightedness, nystagmus (oscillation of the eyes) and retinal detachment. The coloboma may often be accompanied by microphthalmos (abnormally small eyeballs) or anophthalmia (absence of any eye tissue).
Some examples of syndromic coloboma include:
- Treacher-Collins syndrome
- Cat-eye syndrome where the coloboma is a vertical one in the iris, caused by an abnormality of chromosome 22q11
- Patau syndrome caused by an extra copy of chromosome 13 (trisomy 13)
- Coloboma with cryptophthalmos where the eyelids are absent
- CHARGE syndrome which stands for a constellation of Coloboma, Heart defects, Atresia of the nasal choanae, Growth retardation, Genital anomalies and Ear abnormalities, sometimes with microphthalmia
- Manitoba oculotrichoanal syndrome with multiple physical anomalies of the eyes, hair and anal opening
- Fraser syndrome with webbing and number abnormalities of the fingers or toes, or both, with renal and genital abnormalities and sometimes cryptophthalmos
- Goldenhar syndrome with faulty development of the ear, nose, soft palate and jaw
General symptoms
Colobomas are sometimes asymptomatic, but if the macula (the central area of the retina, where sight is sharpest) or the optic nerve are affected, vision is likely to be affected. More than the extent of missing tissue, the location determines the impact on vision. An anterior coloboma affecting only the front of the eye will not affect vision.
LITTLE GIRL WITH RARE COLOBOMA (Cat Eye) | Dr. Paul
However, if the retina is missing in any part, vision is always affected, though not always noticeably. A field defect will be present, meaning that when the person looks ahead, vision in a certain section of the surrounding area will be absent. Most often this is in the upper part of the visual field, since the common site of a coloboma is the lower inner part of the eyeball.
When the fovea is missing, in part or the whole, vision will be poor, while it will be more or less normal if the fovea is preserved.
If the optic disc is significantly affected on one side, the child generally presents with sensory esotropia.
Symptoms of iris coloboma
A complete coloboma of the iris means absence of the pigment epithelium as well as the stroma, and the iris has the characteristic “keyhole” shape. These normally leave the vision unchanged.
A partial coloboma affects only the edge of the pupil, causing it to appear oval rather than round. Sometimes the coloboma may be present only in the pigment epithelium, in which case it is noticed when the eye is examined under transillumination.
Iris colobomas may be isolated or more often accompanied by other colobomas in other parts of the eye.
Symptoms of chorioretinal colobomas
Chorioretinal colobomas occur in the posterior segment of the eye, behind the pupillary opening. These colobomas are caused by failure of the posterior part of the optic fissure. The defect could affect the retinal pigment epithelium, the choroid or the nervous part of the retina. It then appears as a bare area of the sclera, uncovered by any other layers of the eye.
Sometimes a poorly formed or scarred retina will be present. Though the defect is typically in the lower inner part of the retina, the optic disc may sometimes be involved as well.
In most cases, chorioretinal colobomas do not cause any noticeable symptoms, but on examination, there are marked defects in the upper part of the visual field. If the coloboma is large or involves the optic nerve, vision may be lost or very poor and uncorrectable with lenses. In many cases retinal detachment occurs. In rare situations, subretinal neovascularization may be observed, particularly when the coloboma involves the optic nerve exit.
Optic nerve coloboma
Optic nerve colobomas are variable, ranging from minimal involvement to a deformed or swollen optic cup. In this case, the visual impairment is in relation to the severity of the defect.
Diagnosis
A coloboma may be found during an ophthalmologic evaluation. Its discovery should prompt a full eye examination, observing each part for specific findings such as dermoid of the eyelids or sclera, defects of the eyebrows, corneal disease or malformation, obstruction of the tear ducts, cataracts or dislocation of the lens, and colobomas of any other ocular structure.
If the optic nerve is affected, other ocular colobomas may also be observed. Other findings include lens notching and microphthalmos, with macular holes and retinal neovascularization, sometimes leading to retinal detachment.
The deeper the excavation produced by the coloboma, the higher is the risk of retinal detachment (but not visual impairment). The risks of low visual acuity less than 20/200 and retinal detachment are also increased by the presence of retrobulbar cysts or malformation.
Imaging
Following fundoscopy, optic coherence tomography (OCT) of the optic nerve is useful to diagnose any abnormalities of the optic nerve. It is also used to follow up patients to detect neovascularization.
Other examination tools used in this condition as required may include ultrasound of the orbits and MRI (or if not possible, CT) scans of the orbits and the brain.
Physical examination
The patient is examined for any signs of syndromic coloboma, both for treatment purposes and to help detect a genetic cause.
Taking a complete family history of ocular defects from three generations back is also helpful, as is a complete ophthalmic evaluation of both parents.
Tests
Additional examinations may be indicated to screen for associated defects:
- Testing of endocrine function
- Dental assessment
- Echocardiography
- Ultrasound of the kidneys and urinary tract
Genetic testing
This may include testing for chromosomal and single-gene defects, as well as multi-gene panel testing.
If the diagnosis doesn’t fit any known syndrome, the patient should be re-assessed after two years for any new developments.
Further Reading
Last Updated: Feb 26, 2019