May 5 2004
As a follow up to previous work showing that gene therapy can reduce drinking in rats trained to prefer alcohol, scientists at the U.S. Department of Energy’s Brookhaven National Laboratory have used the same technique to cut drinking in rats with a genetic predisposition for heavy alcohol consumption. The findings, along with additional results on the effects of long-term ethanol consumption on certain aspects of brain chemistry, are published in the May 2004 issue of Alcoholism Clinical and Experimental Research.
 “Though we are still early in the process, these results improve our understanding of the mechanism or mechanisms of alcohol addiction and strengthen our hope that this treatment approach might one day help people addicted to alcohol,” said Panayotis (Peter) Thanos, who lead the study in Brookhaven Lab’s medical department.
“Though we are still early in the process, these results improve our understanding of the mechanism or mechanisms of alcohol addiction and strengthen our hope that this treatment approach might one day help people addicted to alcohol,” said Panayotis (Peter) Thanos, who lead the study in Brookhaven Lab’s medical department.
Genetically predisposed alcohol-preferring rats are a much better model for human alcoholism than the rats used previously, which the scientists had to train to prefer alcohol. Without any training, the genetic alcohol-preferring rats drink, on average, more than five grams of ethanol per kilogram of body weight per day when given a free choice between alcohol and plain water. Genetically non-preferring rats, in contrast, typically consume less than one gram of ethanol per kilogram of body weight per day.
In this study, both groups were treated with gene transfer to increase the level of a brain receptor for dopamine, a chemical important for transmitting feelings of pleasure and reward and known to play a role in addiction. After the gene treatment, the alcohol-preferring rats exhibited a 37 percent reduction in their preference for alcohol and cut their total alcohol consumption in half — from 2.7 grams per kilogram of body weight before treatment to 1.3g/kg after. Non-preferring rats also reduced their drinking preference and intake after gene treatment, but not in nearly as dramatic a fashion. The greatest reductions in alcohol preference and consumption were observed within the first few days after gene treatment, and both preference and consumption returned to pre-treatment levels by day 20.
 |
|
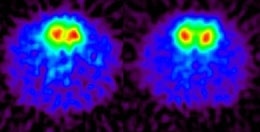
Brain scans showing fewer dopamine receptors (less red) in the nucleus acumbens, or "pleasure center," of alcohol-preferring (P) rats compared to nonpreferring (NP) rats.
|
The gene administered was for the dopamine D2 receptor, a protein shown in various studies to be relevant to alcohol and drug abuse. For example, low levels of dopamine D2 receptors in the brain have been postulated to lead to a reward deficiency syndrome that predisposes certain people to addictive behaviors, including drug and alcohol abuse. The alcohol-preferring rats used in this study have about 20-25 percent lower levels of dopamine D2 receptors when compared to the non-preferring rats, which may, in part, explain their tendency toward heavy drinking.
The scientists delivered the gene by first inserting it into a virus that had been rendered harmless. They then injected the virus directly into the rats’ nucleus accumbens, the brain’s pleasure center. The idea behind this type of gene therapy is to use the virus as a vector to carry the gene to the brain cells, which can then use the genetic instructions to make the D2 receptor protein themselves.
As an additional measure in this study, the scientists used micro-positron emission tomography (microPET) imaging to non-invasively assess the effects of chronic alcohol consumption on D2 receptor levels in alcohol-preferring and non-preferring rats. They measured D2 levels seven weeks after the gene therapy treatment (well after the effects of gene therapy had worn off). D2 receptor levels in alcohol-preferring rats were significantly lower (about 16 percent) compared to that in non-preferring rats. These levels were similar to previous data in naïve preferring and non-preferring rats.
In future studies, the D2 connection to alcoholism will be examined in transgenic mice that are totally depleted of D2. In addition, the scientists plan to develop a second generation D2 vector approach that will provide a longer period of treatment.
“These findings further support our hypothesis that high levels of D2 are causally associated with a reduction in alcohol drinking and may serve as a protective factor against alcoholism,” Thanos said.
This study was funded by the Office of Biological and Environmental Research within the Department of Energy’s Office of Science and by the National Institute of Alcohol Abuse and Alcoholism within the National Institutes of Health.