Sep 21 2016
Researchers from the University of Arkansas for Medical Science (USA), in collaboration with University Hospital Frankfurt and University Hospital Dresden, under the supervision of Prof. Vladimir Zharov and with the participation of Alexander Melerzanov, the dean of Department of Biological and Medical Physics (MIPT), conducted experiments on mice to detect blood clotting using photoacoustic flow-cytometry. The results have been published in the journal PLOS ONE.
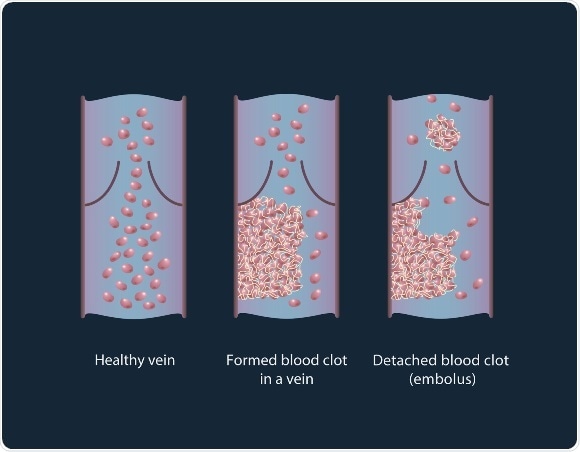
Healthy vein, thrombus formation and its detaching from a vessel wall, leading to thromboembolism.
Clots are classified into two major groups depending on the relative amount of platelets and red blood cells: white clots (characterized by the predominance of platelets) and red clots (predominance of red blood cells). A thrombus (clot) formation is a healthy response to injury intended to prevent bleeding, but can be harmful in case of thrombosis, when clots obstruct blood flow through blood vessels. A thrombus lodging inside a blood vessel is called an embolus (an embolus may be a fat globule, a bubble of air or another gas). Thromboembolism is the flow of a clot that breaks loose in the bloodstream to block another vessel. It is a significant cause of morbidity (disease rate) and mortality (death rate), especially in adults. According to the World Health Organization (WHO), 100-150 out of 100,000 people suffered from thromboembolism in the year 2014.
Unfortunately, existing methods still do not provide accurate results and are not able to destroy thrombi (clots). Doppler ultrasound techniques have shown promise for detecting a large thrombus in vivo, but this method cannot detect micro-thrombi, suffers from artifacts, and requires highly trained personnel. As a result, many thromboses remain undetectable, unless they result in clinical phenomena. About 5–10% of patients die because of a failure to diagnose, rather than inadequate therapy. Although the risk of recurrence decreases with longer durations of preventive anticoagulant treatment, there is no tool for estimating the risk of thrombus-related complications versus the risk of bleeding-associated complications, particularly hemorrhage.
In this paper, the scientists decided to use a theranostics approach – photoacoustic flow-cytometry. Theranostics is a powerful new tool paving the way for personalized medicine, a combination of diagnostics and therapy. Photoacoustic flow-cytometry is a unique method of thrombus detection providing a high spatial resolution for detecting signals up to a few millimeters and potentially destroying the blood clots.
The technique involves irradiating fluorescent dye-labeled cells with a laser beam. The specific wavelength excites fluorescent markers and they emit light at their own wavelength (which differs from the excitation wavelength). The emitted light is collected by a lens and mirror system and decomposed. The detected light is then converted into electrical impulses recognized by a computer, which analyzes the data and plots graphs. Peaks on the graph indicate the blood clot and its type. During the experiment, the mice were injected with a fluorescent dye and the laser was directed onto the blood vessels in their paws.
In this preclinical study, the scientists conducted experiments on two groups of mice: healthy and melanoma-bearing. In the group of healthy mice either clamps were applied to their legs or an incision was made by cutting through the skin and muscle on the mouse’s back. In both situations emboli were produced. In the melanoma-bearing mouse model, researchers observed a correlation between the presence of white emboli and melanoma.
The signals obtained were first averaged 10 times to increase the signal to noise ratio, then the peak to peak amplitude of waveforms was traced. The appearance of a negative peak indicates the passage of a low absorbing object (e.g., white embolus). Traces were then analyzed for the presence of positive and negative peaks exceeding the thresholds obtained from a control experiment.
“We showed that it is possible to detect emboli in the bloodstream using photoacoustic flow-cytometry. PAFC may also be used to destroy blood clots and we hope to work on this in our next experiments,” said Alexander Melerzanov Ph.D., dean of the Department of Biological and Medical Physics (MIPT).
The high sensitivity of the photoacoustic flow cytometry method enables specialists to detect the earliest appearance of emboli in the bloodstream. We expect that this platform, attached to a patient’s hand, or to bypass tubes in the operating room or during a transfusion procedure, will provide an early warning of dangerous embolus formation.