Earlier studies have shown a startling sevenfold increase in illnesses and deaths directly traceable to heroin use in the USA over less than 20 years. Along with this epidemic, HIV and hepatitis infections acquired by injections of drugs have also broken out in large clusters in many places. Yet, the extent of heroin use itself has been neglected. The current study looked at this overlooked area of research.
Heroin
Heroin is a very addictive drug made from morphine, a psychoactive (mind-altering) substance taken from the resin of the seed pod of the opium poppy plant. Heroin’s color and look depend on how it is made and what else it may be mixed with. It can be white or brown powder, or a black, sticky substance called “black tar heroin.”
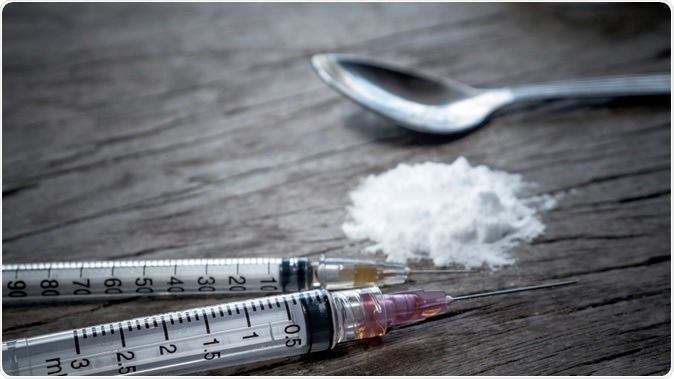
Image Credit: C_KAWI / Shutterstock
Also called by various street names like hell dust, smack, and horse, it is used in multiple ways – injected, sniffed, snorted, or smoked. It is also mixed with crack cocaine – a form of cocaine that can be smoked. Both of these drugs offer an intense high when the resulting mixture (called a speedball) is injected into the veins. Simultaneously, the mouth goes dry, and the skin flushes.
Heroin rapidly reaches the brain after use to affect the nerve receptors that help us feel pain and pleasure, as well as the nerve centers that regulate vital centers like the heart rate, breathing, and sleep.
The long-term complications of heroin abuse include damage to the liver, kidneys, lungs, and brain because of blood vessel blockage by the powdered additives added to the heroin. These can include powdered starch, sugar, or milk. Another major problem is the spread of HIV and hepatitis via shared needles.
Heroin overdose deaths are also on the rise because the drug slows or stops breathing, causing irreversible brain damage.
The study
The study looked at over 800,000 adults who had taken part in the 2002-2018 National Surveys on Drug Use and Health (NSDUH). The information was collected by self-administration of an interview proforma using an audio computer. The average age of the participants was 35 years, while men and women were almost equally represented.
The findings
The researchers found that heroin use went up from 0.2% to 0.3% over the 17 years of the study. This would mean about 1 million people on heroin. Similarly, heroin injection was prevalent in about 0.09% at the beginning but almost doubled to 0.17% by the end. Heroin use disorder was seen in 0.1% at first but went up to 0.21% by 2018.
Those who reported having used heroin at least once in the past year made up a continuously growing percentage of the population, though demographic factors showed some changes. Both men and women contributed equally to this increase. The highest rate of use at the end of the study was in people aged 26 through 34 years (0.31%), men (0.21%), non-Hispanic whites (0.19%), and in the Northeast or West states (0.32%).
The implications
The simultaneous and parallel rise of heroin abuse along with heroin use and injection rates shows that it is due to an increase in the number of people using this drug and not because more people are taking to injections. The real prevalence of these social disorders is likely to be significantly higher than that reported in this study because the NSDUH does not take into account people in jail or homeless vagrants. Self-reporting may also introduce recall bias.
In particular, the recent slowing in the trends of use and abuse may indicate a shift to the use of another illicit drug, fentanyl, and its related compounds.
Suggested solutions
The steady increase in the use of heroin use and addiction, along with accompanying deadly infections contracted by the use of needles for injection, calls for effective measures to combat it. The researchers call for emergency expansion of facilities to offer testing and treatment for these infections; provide sterile syringes so that drug users can continue their habits under hygienic conditions, and use FDA-approved medications for opioid addiction. The focus should be on the population groups at highest risk: Northeast region dwellers, adults up to 49 years of age, men, and whites of non-Hispanic origin.
Interventions to help quit heroin addiction include drugs like buprenorphine and methadone, which can themselves cause addiction. Naltrexone is another therapy, a drug that attaches to the same receptors but blocks the action of the drug. Naloxone is a drug used for emergency treatment of heroin overdose.
Cognitive-behavioral therapy and other psychotherapeutic methods are also used to manage heroin addiction but are usually less effective. Accompanying this, of course, people should be effectively targeted to prevent the use and abuse of opioid drugs, including heroin.
Journal reference:
Han B, Volkow ND, Compton WM, McCance-Katz EF. Reported Heroin Use, Use Disorder, and Injection Among Adults in the United States, 2002-2018. JAMA. 2020;323(6):568–571. doi:10.1001/jama.2019.20844