The world has rarely seen such a readily transmissible infection as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) over the last century. Within five months, the virus has created a Tsunami of COVID-19 positive cases, comprising almost 4.88 million people and causing 322,000 deaths.
However, the spread of the virus is slower than expected in Africa. A new study by researchers at Makerere University and the London School of Hygiene & Tropical Medicine and published on the preprint server medRxiv* in May 2020 is focused on finding any possible link between the low risk of infection and parasitic infections.
The Role of Inflammation in Severe COVID-19
The disease manifestations in COVID-19 range from asymptomatic to critically ill requiring mechanical ventilatory support. Severe COVID-19 manifests with a hyperimmune response that is marked by high levels of pro-inflammatory cytokines like IL-6, IL-2, and TNF-α often termed the cytokine storm or cytokine release syndrome. High levels of IL-6 are associated with increased severity of disease in COVID-19. Some studies show that when patients with severe disease are treated with monoclonal antibodies that block the IL-6 signaling pathway, the duration of stay in the intensive care unit (ICU) is shortened, and there is an earlier resolution of disease.
Immunomodulators in Parasitic Infestation
Parasitic infestations are widespread in Africa. Many parasites live for years in their hosts, without producing significant symptoms. This is due to the interplay of immunity vs. tolerance. In other words, sterilizing immunity, or the development of an immune response strong enough to eliminate the pathogen, is rarely achieved. Still, the parasite count and distribution are kept in check, allowing the host to live a mostly healthy life.
Thus, it may be inferred that parasites are excellent immunomodulators. This knowledge has been used to treat inflammatory conditions like multiple sclerosis and inflammatory bowel disease, where the excreta of parasites are modified to act as immunotolerogenic substances.
This led to the hypothesis that parasitic incidence could be responsible for the low number of cases and a reduced number of deaths in Africa.
The Current Study
The current study aimed to examine the possible link between endemic parasitic infections and the number of COVID-19 cases and fatalities in each of the six WHO regions.
The researchers collected data on the number of cases and deaths from the WHO Situation Report-104 as of May 4th, 2020. They compared it to the data from the 2019 report on world malaria cases and deaths, and the 2018 data for schistosomiasis and helminthic infestations.
After assigning country-specific and regional data on COVID-19 cases and deaths, malaria incidence, and deaths, as well as schistosomiasis and helminth prevalence and endemicity, they carried out an ecological analysis. They found that 42% of countries had endemic malaria, 33% had endemic schistosomiasis, and 50% had endemic helminthiasis.
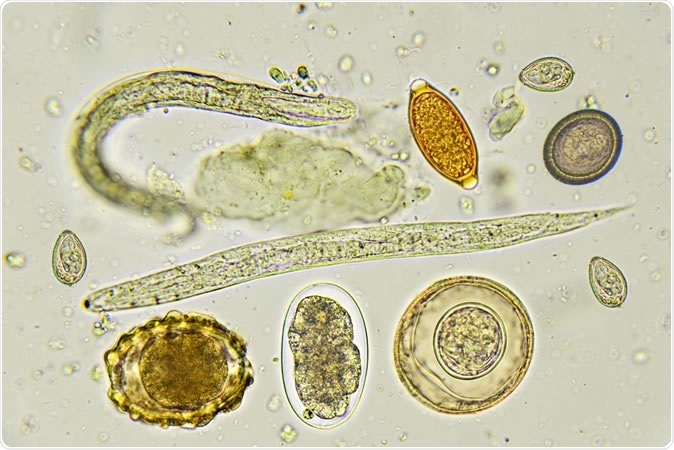
Mixed of helminthes in stool, analyze by microscope. Image Credit: Jarun Ontakrai / Shutterstock

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
COVID-19 Incidence Inversely Related to Endemic Parasitoses
The researchers found that the incidence of COVID-19 was inversely related to that of malaria and soil helminths. In other words, countries with a high incidence of malaria had a low risk of COVID-19. At the same time, those with endemic helminth infestation transmitted through soil or schistosomiasis were at a lower risk for COVID-19.
Africa represents less than 1% of all cases and 0.4% of deaths, though it has 17% of the world’s population. In contrast, Europe, with its relatively sparse population, has 46% of COVID-19 cases and almost 60% of global deaths.
However, Africa also has 93% of the world’s malaria cases, almost 90% of Schistosoma infestations, and a quarter of all soil-transmitted helminths. Europe has only 0.55% of helminth infections, and zero malaria or schistosomiasis cases, in 2018.
The Americas also had about 42% of COVID-19 cases and 33% of deaths, but only 0.4% of malaria cases, 0.7% of schistosomiasis cases, and 5% of helminthiasis worldwide, in 2018.
The median number of COVID-19 cases ranged from 192 to 315 in countries endemic for malaria, schistosomiasis, and helminthiasis. A telling comparison is made from the median number of COVID-19 cases in the WHO African region vs. the median number of cases in the Eastern Mediterranean and Europe (153 vs. 2,344 and 2,127 cases, respectively).
The inverse correlation also means that countries with endemic malaria, schistosomiasis, and helminthiasis would be unlikely to have 600 or more cases of COVID-19. Still, if adjusted for multiple factors, this correlation disappears.
The Hypothesis
An earlier theory was that the molecular and genetic variation in host cells as a result of endemic malaria reduces the susceptibility of the host to COVID-19. The current study extends this protection to schistosomiasis and helminthiasis as well. Similarly, other research suggests that BCG vaccination also negatively correlates with COVID-19 cases and deaths.
The investigators suggested that this was because BCG stimulates nonspecific immunity, which increases the spectrum of protection against other microbes.
People in malaria-endemic areas with stable rates of transmission show detectable malaria parasites in blood but no symptoms of the disease. The same interplay between protective and regulatory immune cytokines is seen in schistosomiasis. Some cytokines promote the formation of granulomas, which protect the parasite eggs, and regulatory cytokines modulate immune responses to prevent pathological responses that would eliminate the parasite.
Severe COVID-19 can also cause a hyperactive pro-inflammatory state, which can be averted or mitigated by IL-6 blockers. All these findings led to the hypothesis that the African sparing by COVID-19 could be due to parasitic infestation-associated immunomodulation.
It is noteworthy that populations who migrate from endemic parasitic infestation areas to others lose their immunity against parasites, and this is supposed to be led to the waning of protection against COVID-19 as well.
As a result of the current findings, the researchers say, “One plausible hypothesis for the comparatively low COVID-19 cases/deaths in parasite-endemic areas is immunomodulation induced by parasites.” The thinking is that parasitic infestation stimulates the host immune response, which involves immunological tolerance through induced regulatory CD4 T cells. This also involves the secretion of IL-10 and TGFβ, which are immunomodulatory cytokines. Together, these may protect the person against COVID-19.
Other Explanations
Alternative explanations exist, such as the lack of diagnostic testing, which excludes the majority of asymptomatic transmission in Africa, limited international travel, which lowers the spread of the infection across country borders, and climate differences. Other mechanisms include the difference in population composition and the lag in the spread of the pandemic.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.