Using 3D human brain organoids, the team found that severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes COVID-19, exerted unexpected neurodegenerative-like effects on human nerve cells.
Jay Gopalakrishnan and colleagues say that, as well as shedding light on SARS-CoV-2 as a potential neurotropic virus; their study demonstrates the role that brain organoids could play in helping researchers understand the pathological effects on the central nervous system.
A pre-print version of the paper is available on the server bioRxiv*, while the article undergoes peer review.
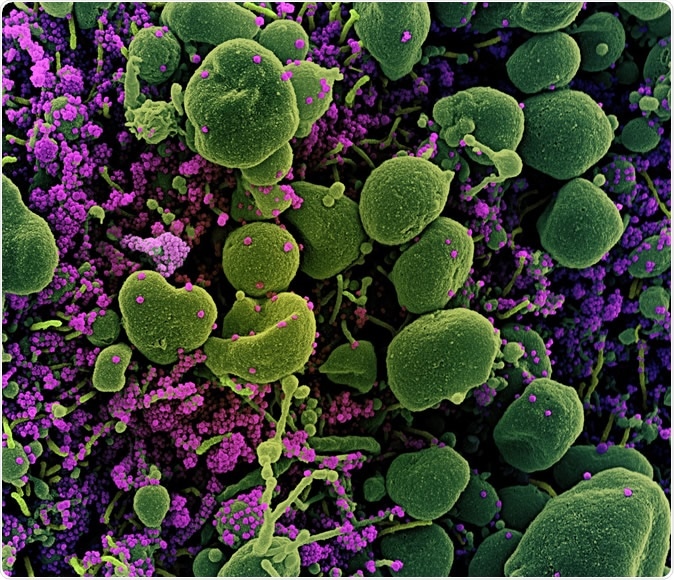
Novel Coronavirus SARS-CoV-2 Colorized scanning electron micrograph of an apoptotic cell (green) heavily infected with SARS-COV-2 virus particles (purple), isolated from a patient sample. Image captured at the NIAID Integrated Research Facility (IRF) in Fort Detrick, Maryland. Credit: NIAID

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Prioritizing research that might help combat COVID-19
As the COVID-19 pandemic continues to pose an immediate risk to global public health, researchers are prioritizing research into the disease’s pathology that might help them better understand how to combat it.
“Thus, it is essential to gain initial insights into the infection mechanisms of SARS-CoV-2, including its target cell types and tropism, to contain its short- and long-term effects on human health,” write Gopalakrishnan and team.
They also emphasize the importance of establishing experimental models that could help researchers understand how to stop SARS-CoV-2 replication and protect human health.
Clinical reports suggest the virus can invade the nervous system
The main symptoms of COVID-19 are dry cough, fever, and shortness of breath - typically indicating respiratory infection.
However, clinical case reports of SARS-CoV-2 patients experiencing neurological symptoms such as loss of olfactory function, stroke, and seizure have been emerging.
These reports suggest that SARS-CoV-2 could be a neurotropic virus that can invade and infect the central nervous system, as do some other viruses such as the ZIKA virus.
Gopalakrishnan and colleagues say that so far, the effects of the virus on the central nervous system have only been debated and not demonstrated in experimental studies.
Now, the team says it is crucial to find out whether the virus can invade and infect human neurons. Furthermore, they add that it is not yet clear whether SARS-CoV-2 is vertically transmitted, from mother to fetus, which could disrupt embryonic nervous system development.
The team used 3D brain organoids to investigate
To examine SARS-CoV-2 as a potential neurotropic virus, an in vitro human model that can closely reflect the neurotoxic effects is needed. In this regard, the team decided to use recently emerged 3D brain organoids that closely resemble the complex and wide array of cell types found in the human central nervous system.
Using serum taken from patients who had recovered from COVID-19, the team showed that SARS-CoV-2 entered the organoids within two days of its introduction.
The virus preferentially targeted cortical neurons, which imaging studies showed was associated with Tau missorting, Tau hyperphosphorylation, and apparent neuronal cell death.
Notably, the team found that in the somas of the cortical neurons, SARS-CoV-2 was specifically localized with Tau phosphorylated at Threonine-231 (T231).
“Detection of early Tau phosphorylation at T231 in SARS-CoV-2-positive neurons is remarkable as it can trigger a cascade of downstream effects that finally could initiate neurodegenerative-like diseases,” writes the team.
Embryonic brains are potentially less susceptible
The team also reports that unlike the ZIKA virus (ZIKV), SARS-CoV-2 did not target neural progenitor cells in the brain organoids.
“The finding that SARS-CoV-2 preferentially targets cortical neurons, but not actively proliferating NPCs may suggest that developing embryonic brains are potentially less susceptible or free from the neurotoxic effects of SARS-CoV-2, writes the team.
“This is indeed is in striking contrast to ZIKV, a neurotropic virus that directly infects NPCs and triggers them to prematurely differentiate into neurons leading to congenital microcephaly.”
Brain organoids can hopefully help scientists prepare for the future
The researchers say their studies highlight the importance of 3D brain organoids as experimental models for investigating the pathological effects of COVID-19 on the central nervous system.
They point out that there have been three coronavirus outbreaks over the last two decades and that future epidemics are not unlikely. The team hopes that with the emergence of human organoid models, which were not available two decades ago, successful modeling of SARS-CoV2 will helps scientists prepare for the future.
“Since organoids are experimentally tractable human in vitro system and convenient to culture as well as to infect, organoid systems may well serve as a test-bed to screen for anti-SARS-CoV-2 agents,” write Gopalakrishnan and colleagues.
“Future experiments utilizing mature state of brain organoids, bioengineered organoids, and orthogonal experiments with complementary in vivo experimental models are assured to dissect the neuropathology of SARS-CoV-2,” they conclude.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources