Since its emergence in Wuhan, China, the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has spread rapidly over most of the world’s inhabited regions, causing millions of cases and hundreds of thousands of deaths. The primary symptoms of COVID-19, the disease caused by SARS-CoV-2, are fever, dry cough, and tiredness.
The spread of the illness is primarily through respiratory droplets. In less than 1% of infected people, conjunctival redness has been observed. This has led to the theory that the surface of the eye could be a pathway of virus entry or a source of infection. This remains to be proved, however.
The ACE2 Receptor Distribution
Studies show that the angiotensin-converting enzyme 2 (ACE2) receptor is responsible for viral entry into cells. This is highly expressed in lung cells, a possible explanation for the pneumonic presentation of the illness, with excessive sputum production and shortness of breath. Transcription product analysis demonstrates that ACE2 is also present in the epithelial lining of the colon and the gut, perhaps responsible for symptoms like nausea, vomiting, and diarrhea.
According to prior research, the cells of the oral, nasal, and nasopharyngeal cavities do not contain ACE2 receptors, which is why the upper respiratory tract is not involved in COVID-19.
.jpg)
Study: COVID-19 receptor ACE2 is expressed in human conjunctival tissue, especially in diseased conjunctival tissue. Image Credit: Kateryna Kon / Shutterstock

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Is ACE2 Present in the Eye?
Now, a new study published on the preprint server medRxiv* focuses on exploring the transmission of SARS-CoV-2 through the conjunctiva, and if ACE2 is expressed in this tissue. The researchers examined the levels of mRNA and protein linked to mRNA in conjunctival tissue.
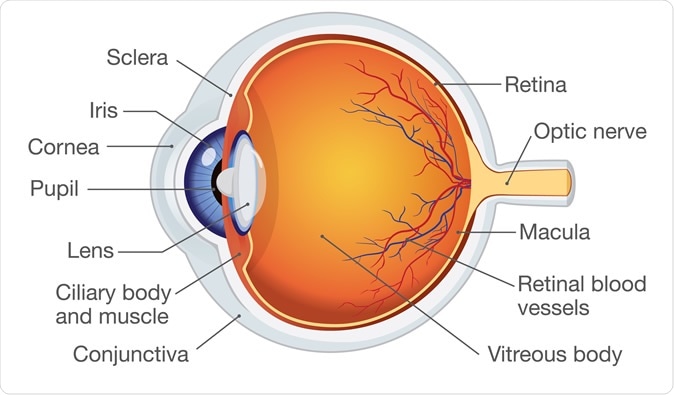
Human eye anatomy. Image Credit: solar22 / Shutterstock
The human conjunctival tissue came from biopsy tissue taken as part of a diagnostic protocol or before surgery. Pathological conjunctival samples came from patients with conjunctival nevi, conjunctivitis, and conjunctival papillomas/cysts/polyps.
Healthy conjunctival tissue came from patients who had suffered an injury to the eye and required removal of the eye as a result.
How Was the Study Done?
The study included 68 patients aged 47 years, on average, with 62 diseased and 6 normal conjunctival tissue samples. The level of ACE2 was examined by real-time quantitative reverse transcription (qRT-PCR). Immunostaining for ACE2 was performed by immunohistochemistry and immunofluorescence.
ACE2 mRNA
The researchers found a marked difference between ACE2 mRNA in healthy and diseased conjunctival tissue, with the inflamed and diseased conjunctiva showing higher levels of overexpression. There was no significant difference between the different diseased tissues in terms of mRNA expression.
The same trend was observed for the ACE2 protein as well, with higher levels being observed in diseased conjunctiva compared to healthy tissue. However, inflamed conjunctiva showed markedly lower levels of ACE2 protein compared to other diseased conjunctival tissues.
Using immunohistochemistry, both polyclonal rabbit and monoclonal mouse antibody against ACE2 receptor, the molecules were found to localize on conjunctival epithelial cells. The level of staining was significantly increased in diseased conjunctiva.
Some other sites of ACE2 expression are the lymphocytes in the supporting tissue and vascular endothelium of the diseased conjunctival tissues like polyps and papillomas, and conjunctivitis, but not in normal conjunctival tissue.
ACE2 Protein
ACE2 protein was also quantitatively overexpressed in diseased and inflamed conjunctival epithelial cells compared to normal conjunctiva. However, the levels were lower in inflamed conjunctival epithelium compared to other diseased conjunctiva.
Potential for Viral Entry and Transmission
The current study reports the finding of the receptor for SARS-CoV-2 in the tissues of the human eye, and especially in the epithelial cells. This represents a potential avenue for viral entry into the human body. The higher expression of the receptors in the pathological conjunctiva compared to that in healthy cells is an important pointer to the at-risk group for infection by this route.
Many respiratory viruses are known to be able to infect the eye and replicate in its tissues, as well as enter the body via this port. This includes parainfluenza viruses in children with conjunctivitis and upper respiratory illness. The earlier SARS-CoV was also observed to spread through contact with the ocular mucous membranes, either direct or indirect.
This indicates that respiratory droplets could well cause the spread of the current SARS-CoV-2 as well through the eye. Earlier studies have shown that the virus was present and detectable by RT-PCR in conjunctival swab specimens from conjunctivitis patients but not in normal tear fluid or conjunctival secretions. The current study confirms the overexpression of ACE2 receptors in epithelium from patients with red or diseased conjunctiva but not in normal conjunctival samples.
Protection Against Conjunctiva-Mediated Infection
The implications are apparent. Since the conjunctiva in such individuals is a potential route of viral entry, protective eyewear must be used by such individuals. Moreover, in addition to masks and other personal protective equipment, protective goggles must be worn by ophthalmologists and other staff who examine eyes at short range.
The researchers also point out that the virus might require a co-receptor in the eye in addition to ACE2, which is an area for future research.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Li, S. et al. (2020). COVID-19 receptor ACE2 is expressed in human conjunctival tissue, especially in diseased conjunctival. medRxiv preprint. doi: https://doi.org/10.1101/2020.05.21.20109652. https://www.medrxiv.org/content/10.1101/2020.05.21.20109652v1
- Peer reviewed and published scientific report.
Li, Shengjie, Danhui Li, Jianchen Fang, Qiang Liu, Wenjun Cao, Xinghuai Sun, and Gezhi Xu. 2021. “SARS-CoV-2 Receptor ACE2 Is Expressed in Human Conjunctival Tissue, Especially in Diseased Conjunctival Tissue.” The Ocular Surface19 (January): 249–51. https://doi.org/10.1016/j.jtos.2020.09.010. https://www.sciencedirect.com/science/article/pii/S1542012420301506.