In recent years, there have been two emerging infectious diseases with a particular impact on pregnant women.
In the 2009 H1N1 flu pandemic, pregnant women had more severe disease, and the Zika virus caused microcephaly and other congenital anomalies.
From this, we can draw 2 conclusions: 1) New infectious diseases will continue to emerge and 2) Some proportion of them will have a disproportionate or additional impact in pregnant women, fetuses, or infants.
When I started to hear about the coronavirus emerging in Wuhan, I started thinking about how we would study the coronavirus in our pregnant population. I put together a team of me, another perinatal pathologist (Dr. Elisheva D. Shanes), a maternal-fetal medicine specialist obstetrician (Emily S. Miller), and a pediatric infectious disease specialist (Dr. Leena B. Mithal).
We designed a study to look at the mom’s disease course, how the infants are doing, and lab tests, including examination of the placenta.
All of the other parts are still happening (including examining more placentas, more testing on placentas), but we felt like there was a gap in the literature that we could start to fill on placentas.

Image Credit: Demkat/Shutterstock.com
How did you carry out your research?
Our hospital began testing every woman coming in for labor and delivery for coronavirus, starting in April.
After women delivered, we collected the placenta, cut out pieces of tissue, made glass slides, and examined them under the microscope. There are about 150 different anomalies we look for, and we note whether they are present.
We tabulated the results and compared then with the placentas examined by our colleagues and former colleagues over the years.
What is the placenta, and what does the analysis of it tell doctors about both mother and fetus?
The placenta is the first organ to form. It is the life support system for the fetus, bringing oxygen and nutrients from the mother and gets rid of carbon dioxide and waste. The placenta also prevents the mother’s immune system from rejecting the fetus like an organ transplant.
The placenta attaches to the wall of the uterus. It links up with the mother’s blood vessels and gets blood from the fetus via the umbilical cord. The blood streams do not mix but get very close together, which allows nutrients and waste to flow back and forth.
Many problems in pregnancy are caused by problems in the placenta. For example, preeclampsia is thought to be caused by problems with the linkage between the mother’s blood vessels and the placenta.
Problems in the placenta can have lifelong consequences for mothers and offspring, including the risk of cardiovascular disease for the mother, breathing problems in infancy or childhood asthma, cerebral palsy, and even cancer in adulthood.
More consequentially for some of our moms, some problems in one pregnancy can reoccur in future pregnancies. Continuing the example, if a mother has preeclampsia in her first pregnancy, she is more likely to have preeclampsia in her second pregnancy.
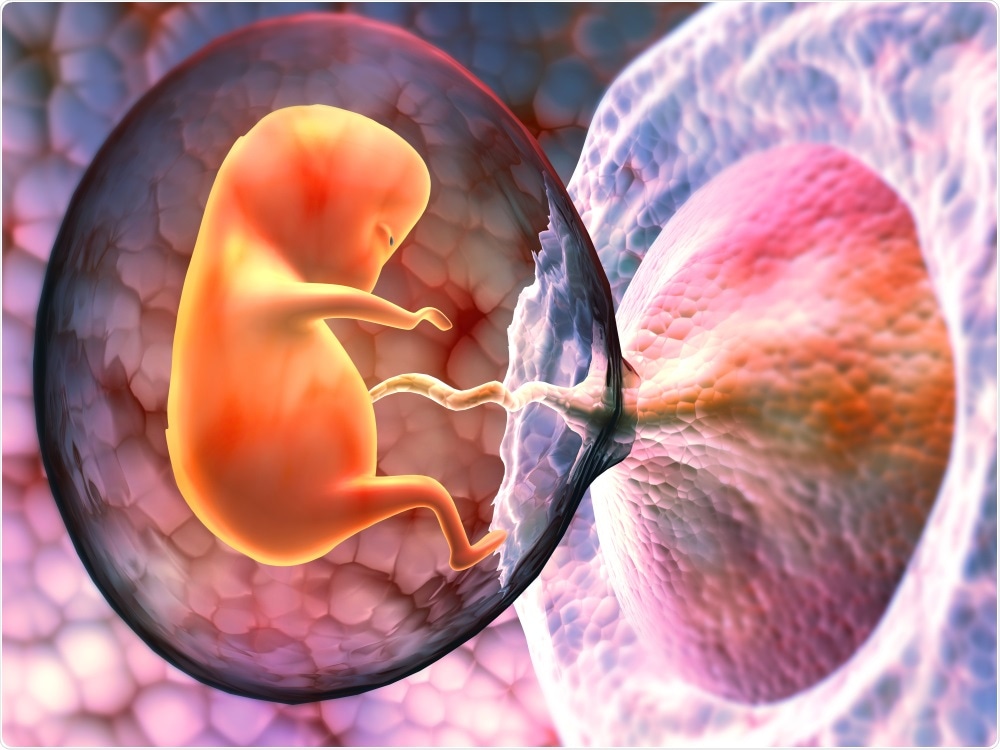
Image Credit: Explode/Shutterstock.com
What type of injury was shown in the placentas of your subjects?
The most significant finding is decidual vasculopathy. As described, the placenta links to the maternal circulation.
Decidual vasculopathy includes problems with that linkage such as blood vessels that can constrict, or even block blood flow, or injury to the vessels.
Were there any other indications of problematic pregnancies?
In the live-born infants, there were very few other indications of problems in pregnancy. One patient had pregnancy-induced hypertension, high blood pressure starting in pregnancy.
Pregnancy-induced hypertension can be associated with decidual vasculopathy, but in our case it was not, and 1/15 women are more or less in line with what you would expect in our general population.
In terms of other problems two women had asthma, 1 had gestational diabetes, high blood sugar starting in pregnancy, and one had cholestasis of pregnancy, a liver problem that manifests as itchiness without a rash.
Could placental injury harm the delivery of a healthy baby?
The injury pattern we saw is associated with maternal hypertension and preeclampsia in the mother. They can cause growth restriction, low amniotic fluid, and fetal demise.
In our case, 1 patient became hypertensive and there was one intrauterine fetal demise, however, it is hard to know whether there is causation.

Image Credit: adriaticfoto/Shutterstock.com
What does this research mean in terms of monitoring COVID-19 in pregnant women?
More intense monitoring of pregnant women with COVID-19 makes sense. For example, fetal growth can be monitored by ultrasound.
Could this placental injury have long-term effects on mothers or infants?
Decidual vasculopathy is part of a larger pattern of a disease called maternal vascular malperfusion (MVM). MVM has been linked with the long-term risk of cardiovascular disease in mothers.
There could be long-term effects on infants. People that were in utero during the 1918-1919 flu pandemic had higher rates of cardiovascular disease decades later.
They also had lower cumulative incomes over their lifetime. To me, this shows that an infectious disease can cause very long-term problems.
What have you found in terms of a possible link between COVID-19 and miscarriage?
We reported 1 miscarriage at 16 weeks. The patient in our case was asymptomatic. There are at least 2 case reports of miscarriages and we are aware of a few cases that have not yet been published.
The problem is that we do not have a denominator, how many pregnancies were there? How many women would have miscarried for unrelated reasons?
We need a larger study involving several hospitals or possibly a large national or state system.
Image Credit: GEMINI PRO STUDIO/Shutterstock.com
What further research is now needed to determine the nature of these findings and expand upon them?
There are a lot of additional directions.
- I regret that we did not include race, ethnicity, and socioeconomic factors, like insurance status, in our paper. COVID-19 is disproportionately affecting communities of color and we have every reason to believe that disproportionality will show up in the placenta.
- Because of the timing of the epidemic, almost all of our cases are in the 3rd trimester. We need to look at 1st and 2nd-trimester exposures to get a better sense of the risk of birth defects or miscarriage.
- Multicenter studies will be important. There is a group in New York that we found (after we had published) published before we did. They do not find the same problems of decidual vasculopathy that we did. I trust our results, but it is important to figure out why they are not seeing what we are.
- We know how some viruses affect the placenta, but there are no well-controlled studies for influenza or the Zika virus, among others. The findings in COVID-19 prompt us to think about what is happening to the placenta in other infections or flu-like illnesses. Are the findings we see specific to COVID-19? Or are they what you would see in anyone that is acutely ill?
- Pregnant women will need to be included in trials of a coronavirus vaccine. The alternative to a controlled vaccine trial in some pregnant women is an uncontrolled vaccine trial in all pregnant women. Their short- and long-term outcomes and placentas will need to be monitored.
How do you hope this research will be used to help ensure the safety of pregnant women and fetuses during the current pandemic, the emergence of any subsequent outbreaks, and any future pandemics?
Our study provides some justification for continuing to treat pregnant women as an at-risk population. Unlike H1N1, COVID-19 does not appear to be more severe in pregnant women than non-pregnant women with similar age and comorbidities.
However, if there is an injury to the placenta, it suggests that fetuses could be at risk. Most states are exiting stay at home orders, but I would suggest that pregnant women, in consultation with their obstetrician or midwife, could choose to stay home and remain scrupulous about social distancing, mask-wearing, etc.
This provides additional information to women and families that are currently considering fertility and would then be pregnant throughout at continuing and possibly resurgent pandemic.
Our study began as a template that could be applied to coronavirus or a different infectious disease on the theory that pandemics are inevitable and that some will have a disproportionate impact on pregnant women.
That is still true. There will be another emergent infection, which hopefully will not be as bad as COVID-19, but one of the lessons learned is that pregnancy researchers (and all sorts of other specialists) should have a plan on the shelf, ready to go, for when that happens.

Image Credit: Maria Sbytova/Shutterstock.com
What is the next stage for your research?
We are continuing to identify new patients and collect placentas. We are also collecting blood from mothers and umbilical cord for biomarker studies. Some inflammatory proteins in the maternal circulation can cross into the fetal circulation.
By measuring those, we can see how much inflammation in the mother could impact infants. Long-term follow-up for these kids is something that we need to make happen.
Where can readers find more information?
Here is our paper: https://academic.oup.com/ajcp/advance-article/doi/10.1093/ajcp/aqaa089/5842018
Here is the other placenta paper: https://journals.sagepub.com/doi/full/10.1177/1093526620925569
Miscarriages:
About Dr. Jeffery Goldstein
I am an assistant professor in the department of pathology at Northwestern University in Chicago, IL. 
My prior scientific work has included studies of the placenta and drug repurposing in gestational diabetes, AI diagnosis in the placenta, and mechanisms of muscular dystrophy in model organisms.
I received my MD and Ph.D. from the University of Chicago, completed residency training in Anatomic Pathology at Vanderbilt University, and a fellowship in Pediatric Pathology at Lurie Children’s Hospital in Chicago, IL.