Early results have flagged loneliness, isolation, and unemployment as having negative mental health impacts. Given that mental health conditions are likely to be exacerbated during times of distress, healthcare systems may need to monitor mental well-being more closely to inform public- and individual-level polices, both during and after “such a mass traumatic event,” advise Lude Franke and colleagues.
A pre-print version of the article is available on the server medRxiv*, while the article undergoes peer review.
The worldwide impact
Since the COVID-19 pandemic began in Wuhan, China, last year, governments worldwide have introduced measures to help curb the pandemic. Containment approaches have included testing, tracking contact transmission, halting “business as usual,” and implementing social distancing and stay-at-home policies.
“The effects of the COVID-19 pandemic will, therefore, be multiple: there will be the impact of the infection itself and the broader societal and health impacts,” write Franke and colleagues.
Impact on the Netherlands overall versus the northern provinces
The first three confirmed COVID-19 cases in the Netherlands were recorded on February 27. By March 24, the number of diagnoses per day had reached 1,126, and up to 1,400 new cases per day were being recorded through to April 24. The Dutch government closed schools, public places, sports centers, bars, and restaurants on March 15, with a more general lockdown on public life imposed during the following weeks.
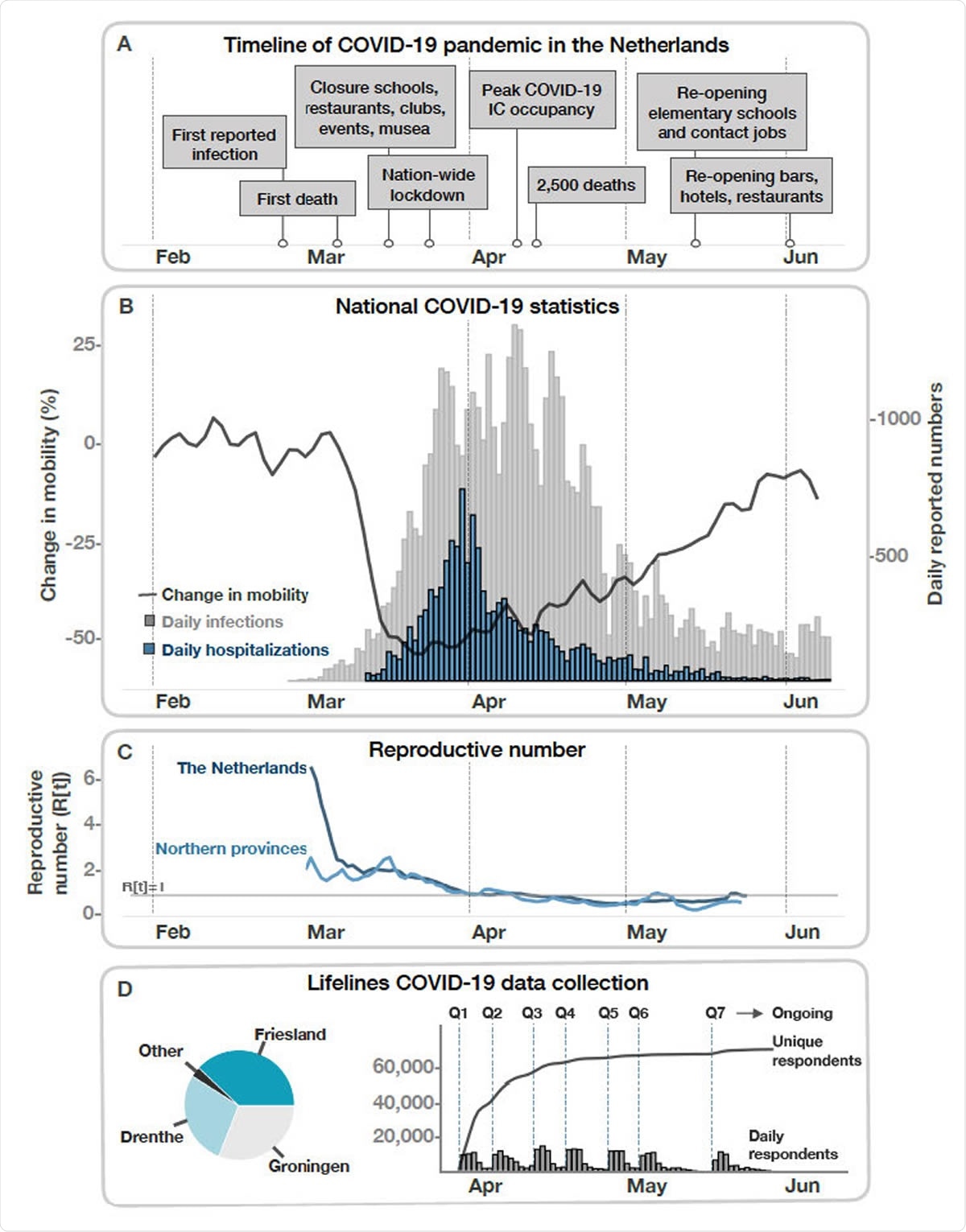

By June 9, 47,903 people had been infected; 11,800 had been hospitalized, and 6,031 had died.
However, the same trends were not observed for the three northern provinces Drenthe, Friesland, and Groningen. The number of infections, hospitalizations, and deaths across the three regions over the same period was 1,491; 320 and 122, respectively.
“It was against this backdrop that the Lifelines COVID-19 research was developed and implemented,” write the investigators.
Investigating the northern provinces
To assess the effects of the pandemic in Drenthe, Groningen, and Friesland, researchers developed a COVID-19 questionnaire that was sent to participants recruited from the Lifelines prospective population cohort and the Lifelines NEXT birth cohort, both of which monitor the health of the northern Dutch population.
This led to the development of the Lifelines COVID-19 cohort, where participants answer questions about their experiences and physical and mental health. The questionnaires were sent on a weekly basis from late March and a bi-weekly basis starting in June. So far, more than 70,000 people have replied at least once.
The researchers say the data will eventually be used to help determine how the pandemic developed in the three northern provinces, which environmental and genetic risk factors predict disease susceptibility and severity and what the associated psychological and societal impacts are.
Preliminary findings emphasize loneliness, isolation and unemployment
Of the participants who responded in the first six weeks, 1,034 (1.5%) said they had been tested for COVID-19, and 116 (0.2%) said the result was positive. A further 811 (1.2%) said a doctor had told them they probably had the disease, and 5,034 (7.3%) said they believed they had the disease.
One of the leading early findings was that feeling of loneliness and isolation had affected people who lived alone more than people who did not live alone, especially in the case of younger individuals aged between 18 and 30 years.
The pandemic also had a significant impact on people’s working lives. The number of responders reporting being unemployed rose from 7.5% when the first questionnaire was sent to 14% by the time the fifth questionnaire was sent.
More recent results showed that by the end of May 2020, when the number of cases and hospitalizations had fallen and schools and businesses reopened, participants started reporting less anxiety, fewer job-loss worries, and improved sleep.
What are the next steps?
The COVID-19 questionnaire data is currently being used to analyze to address the main goals of the project, say the researchers.
The infection cases reported are being used to track the outbreak, and the symptoms reported are being used to produce a COVID-19 prediction model. The information on chronic illness, medication use, and environmental factors will be used to help identify risk and protective factors.
Finally, it will be possible to comprehensively examine genetic factors, since almost 18,000 respondents have been genotyped, says the team.
Given the significant distress that strict government containment measures can place on society, “close monitoring of mental well-being is important for both short- and long-term public health policies and individual-level care,” write Franke and colleagues.
“Alertness in clinical systems and tailored mental health care may be needed during and after such a mass traumatic event,” they conclude.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Franke L, et al. The Lifelines COVID-19 Cohort: a questionnaire-based study to investigate COVID-19 infection and its health and societal impacts in a Dutch population-based cohort doi: https://doi.org/10.1101/2020.06.19.20135426
- Peer reviewed and published scientific report.
Mc Intyre, Katherine, Pauline Lanting, Patrick Deelen, Henry H Wiersma, Judith M Vonk, Anil P S Ori, Soesma A Jankipersadsing, et al. 2021. “Lifelines COVID-19 Cohort: Investigating COVID-19 Infection and Its Health and Societal Impacts in a Dutch Population-Based Cohort.” BMJ Open 11 (3): e044474. https://doi.org/10.1136/bmjopen-2020-044474. https://bmjopen.bmj.com/content/11/3/e044474.