The current pandemic of COVID-19 is spread by the dispersal of aerosols and droplets containing the severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) on to surfaces and through the air around an infected individual. While common sense and scientific evidence both suggest that under such conditions, breaking the chain of transmission by avoiding contact with such droplets is advisable, this has met with unexpected resistance by some sections.
Hand hygiene, social distancing, and the general donning of face masks may help to reduce the transmission of the virus. However, both the public, in some places, and the scientific establishment, have derided or opposed the wearing of masks, in particular. Some say that randomized controlled trials (RCTs) show inconclusive results, while others raise doubts as to the effectiveness or safety of non-surgical face masks worn outside of healthcare settings.
Secondly, the recommendations made by several health organizations and countries regarding masking practices vary, causing further confusion even in countries where this has been made a mandatory or strongly encouraged practice. And thirdly, some feel that masks may cause people to feel a sense of false security, introducing laxity about the more necessary precautions and ignoring the real chances that the virus can get through the mask.
Meta-Analysis of Studies on Mask Efficacy
Now a new study published on the preprint server medRxiv* in August 2020, therefore, presents the results of a meta-analysis that takes account of the lack of compliance with mask-wearing in RCTs, as well as the lag between the event and the measurable effects. The researchers also looked into possible adverse effects.
The study analyzed the findings of RCTs of non-surgical face masks concerning the number of viral respiratory infections, beyond hospitals and households. They attempted to find both protective and infection-promoting effects of mask-wearing in the community setting only.
Predicted and Demonstrated Reduction of Infection Rates
Currently, masking has been predicted to reduce viral spread significantly, and it is also predicted that less than complete compliance and the use of non-medical grade masks is sufficient for this effect. Again, a review showed that they did bring about source control, quite apart from the protective effect. And finally, there is evidence from other real-time scenarios that when masks are used widely, those countries or regions show a decline in the proportion of infection and deaths due to COVID-19. In fact, a meta-analysis showed that not just COVID-19 but also other infectious viral illnesses reported in 172 papers all displayed the same negative trend as already reported in association with mask use.
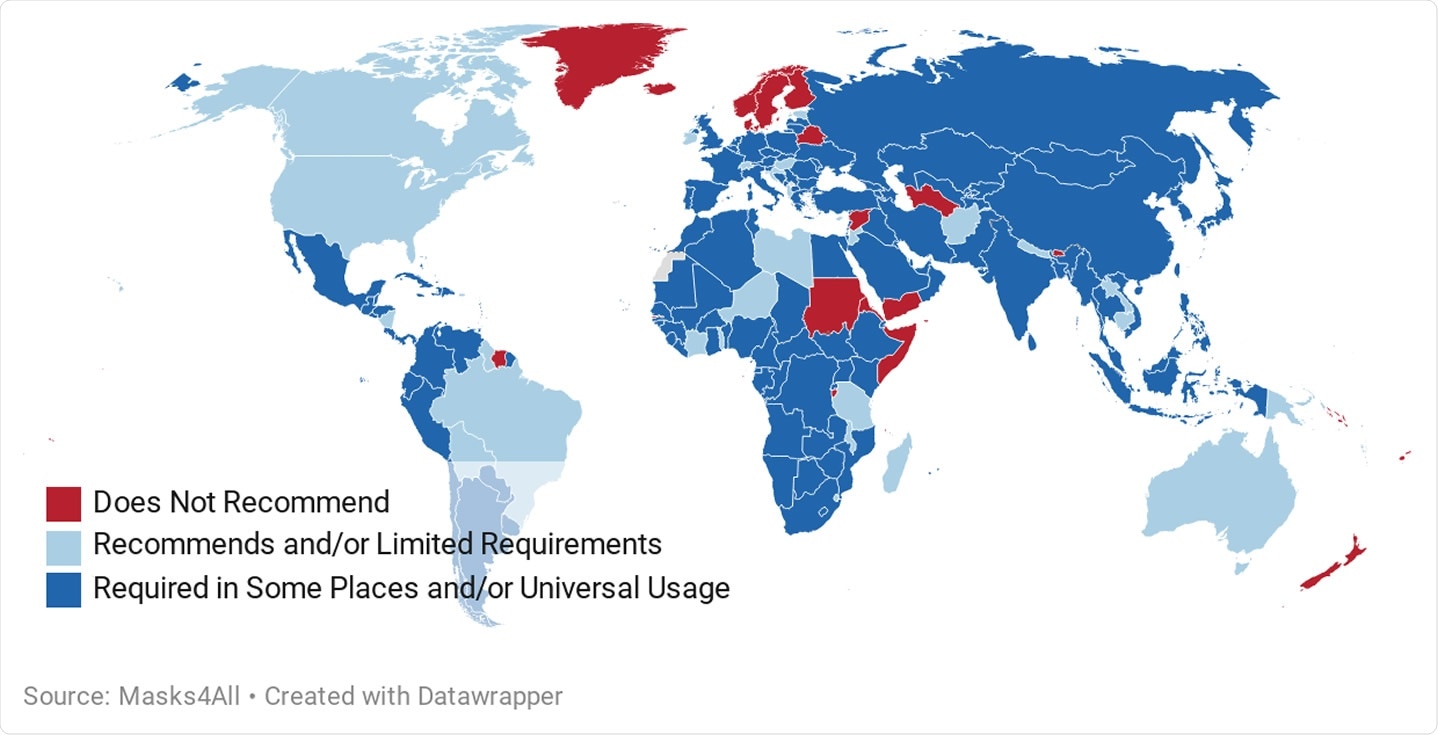
Which countries require or recommend public mask usage to help contain COVID-19 infections (date: July 30, 2020)
Yet, many scientists have complained of the lack of evidence that mask use is effective in hampering COVID-19 rates from the gold standard of modern medicine, the randomized controlled trial. Moreover, existing RCTs have ignored the existence of non-compliance.
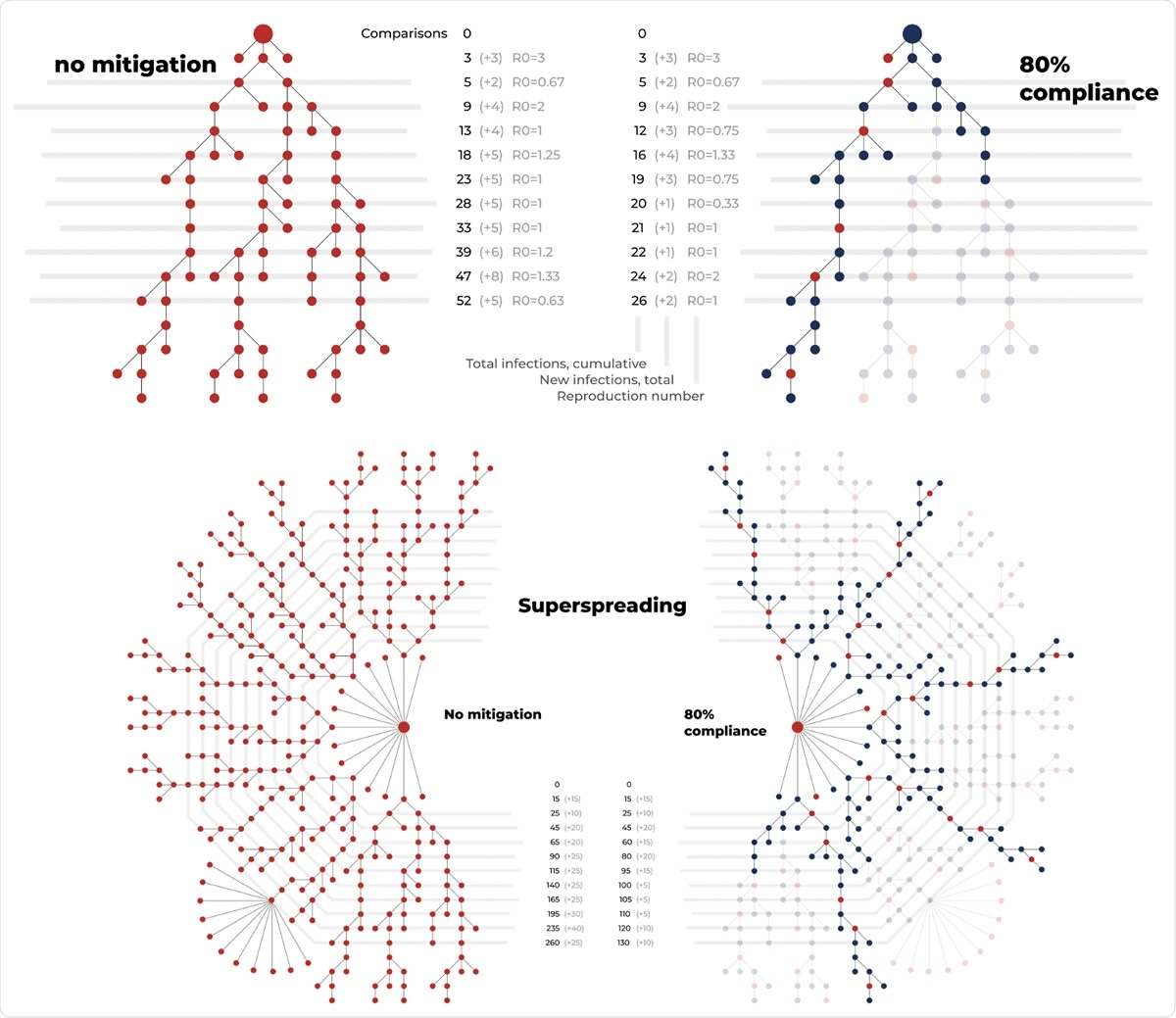
Illustration of possible effects of face mask use in preventing infections. Typical chain of infections without masking (top). When 80 percent compliance in mask use (blue) is achieved, half of the infections can be prevented. Visualization of cluster of infections through one super spreading event below. Mitigation through 80 percent compliance in face mask use together with other protective measures can prevent individual infections and infections through super spreading events. Red shows infection without mask, blue indicates use of face mask and infection. Image by Riina Rupponen.
Controlling for Study Bias
The current study included all papers that examined the use of face masks of various materials, including cloth, surgical sheeting, or FPP1, in a population that was susceptible to respiratory infection, excluding healthcare workers. This population was compared to the group who did not wear face masks. The outcome was measures of the risk of infection in the mask vs non-mask group, as well as the safety and effectiveness of the intervention, in addition to the decline of infection rates in the population.
The researchers found that there was a significant degree of variation in the population and statistical analysis of different RCTs. In many studies, there were a number of individuals in the control group who wore masks, between 12% to 53%, which could significantly vitiate the degree of certainty about the outcome estimates. They, therefore, made adjustments for the proportion of controls who wore masks.
Also, compliance with the use of face masks in the intervention group varied from 27% to 76%, introducing further uncertainty. They also noted that some studies had follow-up lasting for as long as 6 weeks from the start, which they included in their study. This was to reflect the knowledge that respiratory infections typically have incubation periods lasting from 1-10 days, delaying the benefit of the face mask. And in addition, it is wise to allow for pre-study exposure, which could lead to the occurrence of infections in the early days of the study.
Face Masks Are Useful in Controlling Infections
However, they showed that face masks had a strong effect in preventing the occurrence of respiratory infections, with respect to controls. This is the first time such a finding has occurred. This was supported by the sensitivity analyses they made.
While 3/5 studies reported the impact of face masks in controlling the spread of respiratory infections, the other two concluded that evidence was lacking. In contrast, the current study shows that masks do significantly reduce the spread of COVID-19 in the context of RCTs.
The researchers also found that the most significant protective effects were seen with the greatest compliance among both treatment and control groups. Obviously, if over half the control group were wearing masks when they were not supposed to, this would reduce the significance of the outcomes markedly. This occurred in the context of a pilgrim group in an Islamic holy place.
In contrast, where intervention and control groups were clearly demarcated, as in the college student cohort, with compliance of 76% and 88% respectively, the effect was more striking. Moreover, with the pooling of studies using properly chosen statistical methods, information can be derived even from heterogeneous or biased studies.
Non-Universal Use, Non-Surgical Masks, Are Still Useful
One aspect of the current debate over mask use was whether non-medical grade masks were useful in stopping the spread of infection and whether the wearing of masks by untrained individuals is safe, as well as the risk of infection due to contamination, or alternatively difficulty with breathing, in such scenarios.
The studies dealing with mask efficacy have mostly used medical filter masks, including both cases and controls. Moreover, the pooled effect meta-analyses are many, showing agreement with the current study in demonstrating the strong protective effect of face masks. The estimated number needed to treat (NNT), that is, the number of masks that must be worn to prevent a single infection, ranges from 3-6 for N95 respirators and face masks, respectively. The NNT could be still greater if the population prevalence of infection is low.
Another conclusion of this study was that face masks are most effective when coupled with handwashing and other protective steps, and especially physical distancing, which reduces the local concentration of viral particles in the air and so on the masks.
No Adverse Effects
As for the fear that masks could induce carelessness bred of false security, there is no evidence that this occurs. American studies show that when employees are asked to wear masks, people tend to restrict their movement from place to place and maintain their distance from each other.
Adverse effects such as difficulty with breathing were reported by a quarter of mask wearers in one study, whereas another reported that about the same number complained of discomfort, and sometimes of feeling hot, sweating, or fogging of eyeglasses. No severe adverse effects have been reported.
Overall, therefore, they sum up, “Our findings from existing randomized controlled trials support the health policy of public use of face masks to limit the spread of COVID-19.”
Strange Reluctance and Conclusions
In the face of all these findings, say the researchers, “it is surprising that policymakers have been reluctant to recommend masks to prevent infections despite the evidence that masks prevent deaths at hospitals, assisted living and nursing home settings, and globally limit the spread of the pandemic.” In fact, this tardiness in agreeing with evidence in favor of masks was reflected in the advice given by the World Health Organization (WHO) for months after the start of the pandemic.
This strange reluctance is a legitimate subject for further study, as it may identify the cause of slow reactions by national and international health authorities, help to evolve the steps involved in examining and possibly changing existing guidelines in response to evidence, and coming to terms with mistakes more rapidly. This will be of great help in facing future disasters of the same sort.
For now, they conclude, “Recommendations and clear communication of the benefits of face masks should be given by policy makers to limit the number of infections and ultimately deaths, and to ensure sufficient safety measures to control local and global COVID-19 disease clusters providing time for vaccine development.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources