Using data from the national register in Denmark, researchers studied how likely persons infected with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) transmit it within their households. The study found additional household members tested positive in 17% of cases after one person in the household was infected. The research is published on the preprint server medRxiv* in September 2020.
The world has been grappling with the coronavirus pandemic for nine months now. A critical component of responding to the pandemic and taking steps to control it is to understand how it is transmitted.
There are several ways in which the virus is transmitted, such as by touching contaminated surfaces and via aerosolized droplets. However, it is believed that human-to-human transmission is one of the most common methods by which the COVID-19 disease spreads.
To fully understand SARS-CoV-2 transmission during this pandemic, most authorities rely on contact tracing, or tracing and monitoring individuals who come in contact with an infected person.
However, this is an extremely laborious process requiring a lot of resources. This technique worked well during the beginning of the pandemic when there were relatively low numbers of infected persons. With the number of cases touching tens of millions now, contact tracing becomes very difficult.
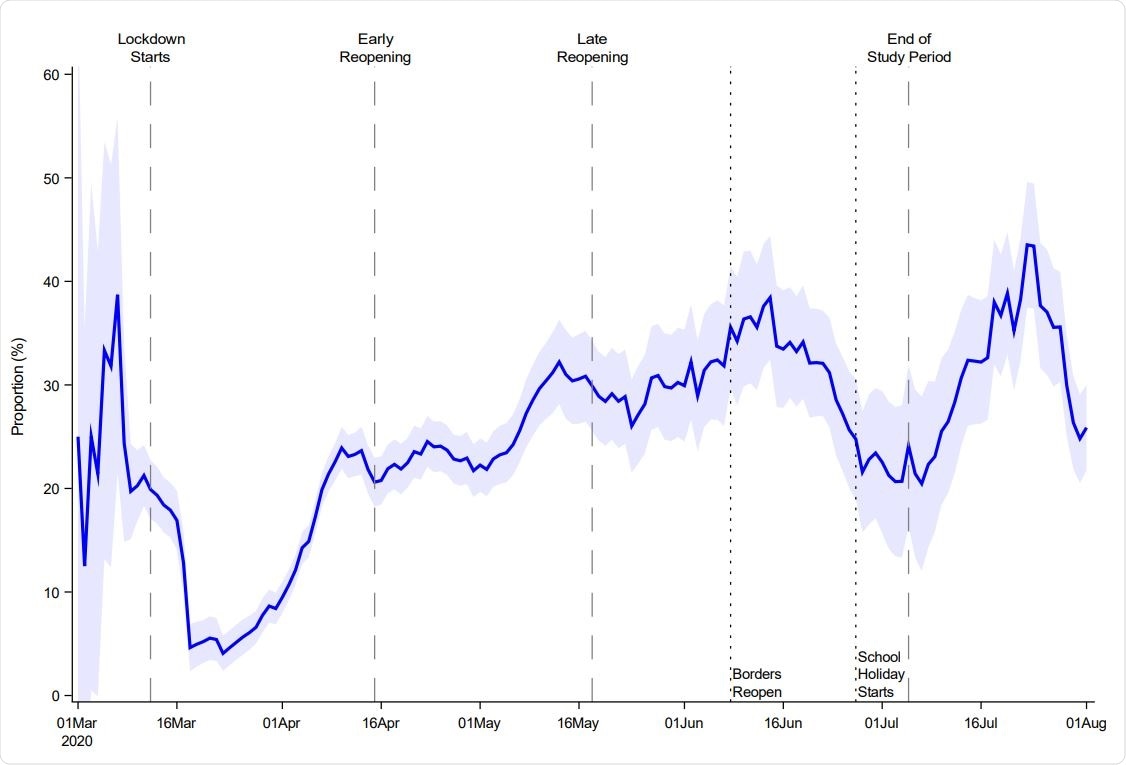
This figure shows the proportion of positive tests originating from households, as defined by new cases that live in a household with another case that tested positive within the preceding 14 days. The figure shows a seven day moving average, while the shaded area shows the 95% confidence bands with standard errors clustered on the individual level.
Modeling transmission using Danish registry data
To get around contact tracing challenges, a team of researchers in Denmark took advantage of the Danish administrative register, which contains information about all residents of Denmark linked to their unique personal identification number. The Danish Civil Registry System has information about the age, sex, and home addresses of individuals, which they linked to the data about SARS-CoV-2 individual infection from the Danish Microbiology Database.
Using these databases, the researchers first formed households by putting together individuals with the same address, limiting the household size to six or less. Their data covered about 98% of the Danish population.
The first positive case from a household was considered a primary case. Any other positive cases within 14 days of the primary case were secondary cases.
After the first case was reported in Denmark in late February, the country went into a near-total lockdown from March 12 to April 14. The next month, or the early reopening, saw the reopening of daycare and schools up to grade 5. After May 18, all schools and colleges were opened along with restaurants and small bars, which the authors call late reopening.
Transmission within households
Using this methodology, the team identified 6,783 primary cases from March 12 to July 24. Of the potential about 14,000 secondary cases, they found about 13% tested positive for the virus over the total period of the analysis. The number of positive secondary cases increased once the country started reopening, with the maximum being about 17% in the late reopening phase.
About 76% of the secondary cases were detected three days after the primary case. “This highlights the importance of fast contact tracing, as most secondary cases are found in the first couple of days after the primary case,” write the authors.
Since April 2020, household transmission contributed to between 20% and 45% of all the positive cases, suggesting that national guidelines take into account this mode of disease spread as well.
The transmission depended on the ages of the people in the household. If the primary case was a child, less than 15 years old, the additional members of the household that tested positive did not change with the ages of the members. But, children less than 15 years also have a higher chance of transmitting the infection to others in the household, perhaps because of close contact with parents and other caregivers.
In contrast, when the primary case was older than 25 years, the chance of transmission increased linearly with the age of the people in the house, suggesting susceptibility to the disease increases with age.
The researchers found that once a primary case was detected in a house, the probability of at least one other case caused by the primary case was 23%. Surprisingly, this probability was the same irrespective of the number of people in the house.
Implications
The results of the study can be used in mathematical models that are used to understand and estimate how COVID-19 spreads. Most models assume that each contact has the same probability of transmitting the virus. However, that is not true, and the first step is to determine if the contact is infectious.
Furthermore, there is a difference in transmission with the age of the primary and secondary cases, which should also be taken into account. However, even though transmission risk increased with age, children can also transmit the virus.
The authors suggest that because a significant proportion of transmission was within households, strategies for preventing COVID-19 should also include in-house transmission.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Lyngse, F. P. et al. (2020) COVID-19 Transmission Within Danish Households: A Nationwide Study from Lockdown to Reopening. medRxiv. https://doi.org/10.1101/2020.09.09.20191239
- Peer reviewed and published scientific report.
Lyngse, Frederik Plesner, Carsten Kirkeby, Tariq Halasa, Viggo Andreasen, Robert Leo Skov, Frederik Trier Møller, Tyra Grove Krause, and Kåre Mølbak. 2022. “Nationwide Study on SARS-CoV-2 Transmission within Households from Lockdown to Reopening, Denmark, 27 February 2020 to 1 August 2020.” Eurosurveillance 27 (6). https://doi.org/10.2807/1560-7917.es.2022.27.6.2001800. https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2022.27.6.2001800.