As the UK moved towards a surge in COVID-19 cases at the end of summer, the government introduced a three-tier system of social restrictions on October 14, 2020, to stave off a nationwide lockdown. The results appear unremarkable on the outside, but the truth is that they allowed the authorities to delay a lockdown until November 5. This system could be tweaked to allow a more effective control of viral spread, while still ensuring that families can choose their own course of action over the Christmas holidays, says a new preprint published on the medRxiv* server in late November, 2020.
Though a few vaccines are moving towards limited deployment, it is impossible to vaccinate those at risk before Christmas, 2020. In view of the expected mingling of families from all over the UK during this holiday season, several researchers have predicted that it will lay the foundation for a third wave of COVID-19.
Studies have picked apart non-pharmaceutical interventions (NPIs) to identify the most cost-effective among them, with respect to their human cost. The current study examines the UK three-tiered COVID-19 containment system, which was in force in the second half of October 2020. This envisaged different levels of social mixing restrictions, with tier 1 allowing for groups of up to 6 people from different households to meet. Tier 2 allowed up to 6 such people to meet outdoors. For tier 3, the strictest restrictions were applied, prohibiting mixing between households, indoors, or in private outdoor spaces. Rules were framed to deal with sports activities, travel beyond the neighborhood, eating out, and other social activities. This was designed to be a flexible system, with people in one or other tier being shifted up or down as circumstances changed.
However, a second national lockdown ensued, from November 5 to December 2, 2020 – the latter being the planned end date. Stay-at-home orders with the closure of non-essential businesses, while keeping schools and universities open, were issued. The end of the lockdown may see a reverse shift to a three-tier control strategy again, prompting an examination of its value in containing viral spread, tier by tier based on localized outbreak and transmission.
The researchers estimated the effective reproduction number (R number) for each of the 315 local authorities, over days 0, 7, 14, 21 and 28, beginning on October 14 for those who remained in tier 1 throughout. For other local authorities, it was the date on which they were placed into their final tier. Analyses were reoriented accordingly, with lower tiers that moved higher being included in the former for 7 days from reallocation, and in the higher tier from the day of reallocation.
The number of cases saw a rapid rise from early September to October 5, flattening slightly until October 16, followed by a slower rise from the 23rd to the 30th of October. After this, cases shot up again. For all local authorities, the initial R-value on October 14, or the start date for tiers 2 and 3, was over 1.1, which corresponds to exponential growth, and this remained at this level over the next four weeks.
For tier 1, R remained constant, more or less, indicating exponential growth. In tier 2, the R-value on day 0 was above 1.1 but fell to 1 by day 14. One week later, the transmission rate became greater so that by day 28, the R was higher. Tier 3 authorities had a similar initial R-value, which fell to and remained at 0.9 from day 14 to day 28, indicating that the outbreak declined in these areas. R values were higher even if the Tier 1 authorities were moved up to Tier 2 during this period.
All tiers had the same initial variance on day 0 but a marked difference at each week thereafter, the greatest difference being on day 14 and day 21. Most areas showed growth. Thus, the smaller difference at day 28 is likely to be due to the low number of authorities included in day 28.
The researchers found, therefore, that the tier of restriction predicted the epidemic trend. Most Tier 3 authorities saw a fall in the number of cases with the R falling below 1, while case numbers remained static in tier 2 because of opposing and equal trends in different authorities. Tier 1 restrictions were therefore not effective in terms of transmission control, while tier 3 was very effective in most cases.
Discretionary powers to move up or down the tiers did not seem to be useful, since Tier 2 authorities did not show a significant difference in their R-value at the point when some were moved up to Tier 3 while others remained in Tier 2. In other words, these authorities were split 50:50 between exponentially growing epidemics by day 14 and a slight decline followed by an increase on days 21 and 28.
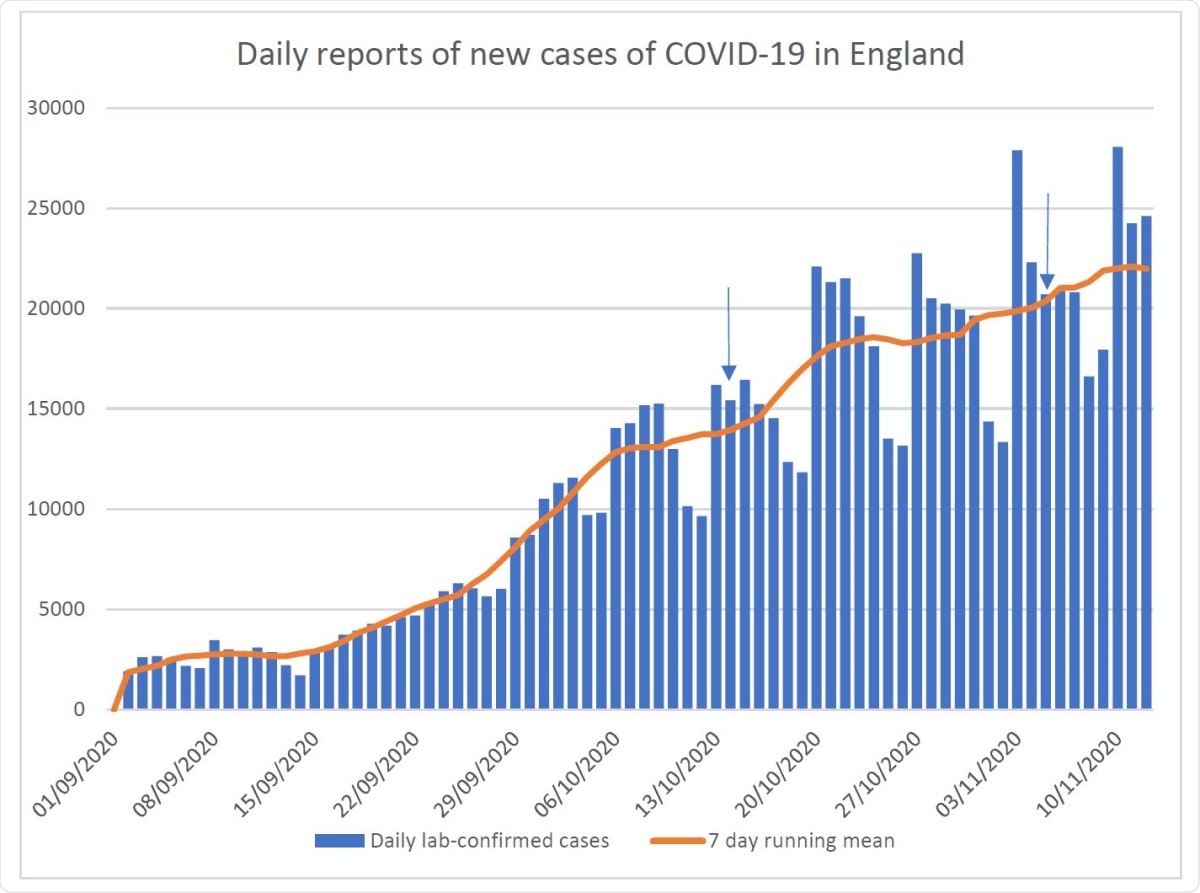
Daily reports of new cases of COVID-19 in England based on sample collection date.
The researchers conclude that the tier 2 authorities that failed to record a fall in R should have been placed in tier 3 from the start, and most tier 1 authorities would have been better placed in tier 2. On the other hand, tier 3 seems to be effective in reducing R to below 1 almost always. Thus, what is needed is not more restrictions, in most cases, but a more rapid identification of increasing spread, with a quick shift to a higher tier.
It is interesting that after the lockdown from November 5 was announced, but before it was implemented, the case numbers went up more steeply, over the first week of November, compared to the last week of October 2020. The authors suggest this could be due to increased social mixing in view of the impending lockdown, though there is no evidence of this. Again, all tiers exhibited some R-value increases at day 28, which may signify some influence that is not clear.
Previous research has suggested that household spread is the major contributor to infection rates. When gatherings of even 10 people are not allowed, transmission rates decline. Since the three-tier system in use here did not allow groups to gather in any number within a building, superspreading events would thereby become less likely in authorities under tier 2 and tier 3 restrictions.
Further study is necessary to elucidate which of the restrictions applicable to each tier was responsible for reducing R-value. Another issue is the observed general lack of awareness of social distancing rules and about when to get tested for the virus. This indicates a shortcoming in population-level education regarding the government’s strategy on controlling the virus, and what people are expected to do.
With the approaching Christmas holidays, it would seem that it is ideal for spreading the awareness of how to get together safely, to minimize the expected boost in viral transmission, rather than prohibit gatherings. As Professor Stephen Reicher, an expert in social psychology at the University of St Andrews, opines that the shift from a ‘the government knows best’ attitude to one encouraging the people to partner with the authorities is desirable.
This will promote greater individual responsibility as people work on making good choices with respect to social interactions. This could be invaluable, not only over the Christmas season, but the rest of the winter season.
Incentives would also be a good idea, says the professor, such as extra holidays to allow family meet-ups later, under safer conditions, when high-risk groups are expected to have received the vaccine. This could reduce gatherings at Christmas without having to skimp on time together.
And finally, allowing families to reunite now would not only be sensible, since some are likely not to see another year but would also boost the general wellbeing of many enough to make it through several more months of social distancing.
The authors sum up, “It seems likely that the tier system will better prevent spread of SARS-CoV-2 with faster identification of the appropriate placement of each local authority and swifter reallocation when needed.”

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.