The first phase of vaccination against infection with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the agent that caused the coronavirus disease 2019 (COVID-19) pandemic, is underway in many countries the world over. However, logistical problems and vaccine hesitancy, and the shortage of doses at present are likely to prevent complete and uniform global coverage with the vaccine in the near future. Nonetheless, herd immunity by vaccination is the only feasible path to global recovery from the massive disruption of health, economic activity and lifestyles brought about by the pandemic.
The virus mediates host cell attachment and infection via its spike protein. This antigen is, therefore, the primary target of antibodies elicited by most vaccines. In the current paper, the researchers describe using a live attenuated virus vector to introduce the modified spike antigen into the human host via vaccination, to induce specific neutralizing antibodies directed at the S1 subunit of the spike.
The virus chosen as the vector was the vesicular stomatitis virus (VSV), an RNA virus that can replicate within the human host. This vector is engineered to express the open reading frames with appropriate start and end signals for transcription of the SARS-CoV-2 spike protein's S1 subunit.
The S2 subunit was removed to induce neutralizing antibodies against epitopes on the receptor-binding domain (RBD) on the S1 subunit. The full-length spike can allow the generation of both pre-and post-fusion spike protein, both of which have their own adverse impact on vaccine production.
The S2 subunit is also more highly conserved between coronaviruses, allowing cross-reactivity directed at this unit rather than at the SARS-CoV-2 S1 subunit. Finally, the full-length spike can be expressed only by disrupting host viral protein trafficking, which severely interferes with vaccine virus replication and thus with vaccine production.
A similar strategy was adopted to develop a vaccine candidate against the earlier human pathogen, the Middle East respiratory syndrome coronavirus (MERS-CoV). This was switched to the current setting to speed up the process of vaccine production.
The modified antigen contains the S1 subunit of the SARS-CoV-2 S2 antigen, anchored to the membrane of VSV by the latter's G protein. The G protein tail thus allows the S1 to be integrated into the VSV particle. This vaccine candidate was called ConVac.
The researchers then used the golden Syrian hamster model of COVID-19, which has been recently set up to express severe COVID-19. These animals develop intranasal infection with wildtype SARS-CoV-2, resulting in severe disease, as seen in humans at similar stages of infection.
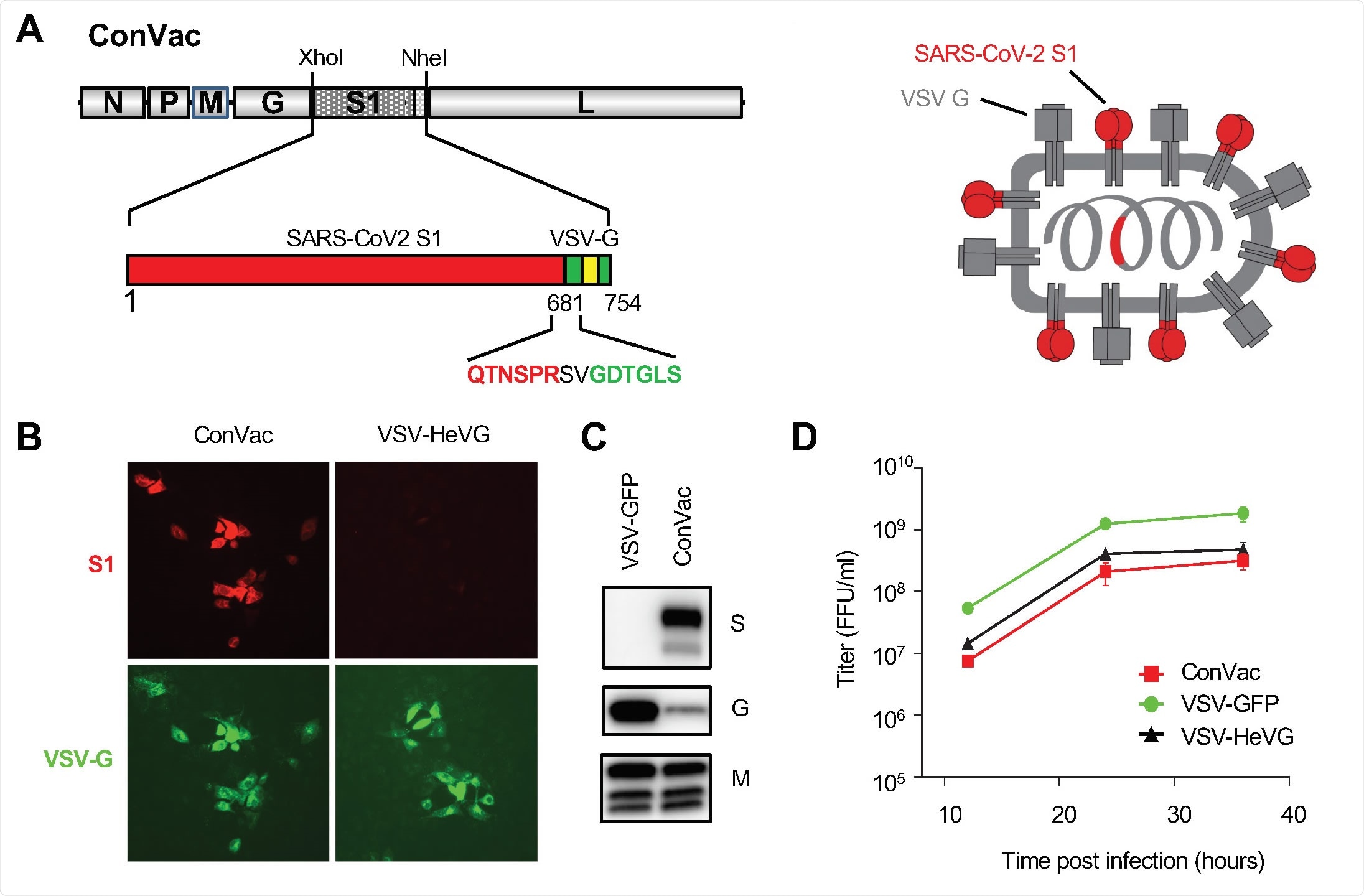
Generation and characterization of ConVac. (A) Left: genome structure of the VSV vector expressing the membrane anchored SARS-CoV2 S1 domain. The S1 domain of SARS-CoV2 spike protein (aa 1-681) was joined to the C-terminal 70 amino acids of the VSV glycoprotein. The fusion construct was inserted between the glycoprotein and polymerase genes of VSV. The S1 domain is shown in red and the VSV G tail in green. The transmembrane domain of the VSV glycoprotein is indicated by a yellow box. The amino acids at the junction between S1 and VSV glycoprotein are highlighted. Right: schematic representation of the vaccine construct which shows the two transmembrane proteins anchored in the membrane. (B) Immunofluorescence staining of Vero E6 cells infected with ConVac and a control virus expressing Hendra virus G (VSV-HeVG). The cells were fixed and permeabilized 10 hours after infection and stained with fluorescently labeled monoclonal antibody CR3022 against the S1 domain (shown in red) and two monoclonal antibodies against the VSV glycoprotein (shown in green). (C) Western blot analysis of BSR cells infected with Convac and a control VSV virus expressing GFP. Protein lysates were resolved on 4-20% polyacrylamide gradient gels and transferred to nitrocellulose membranes. The membranes were probed with polyclonal antiserum against the S1 domain (upper panel), monoclonal antibodies against the VSV glycoprotein (middle panel) and a monoclonal antibody against the VSV matrix protein (lower panel). VSV glycoprotein expression was significantly reduced in cells infected with ConVac whereas matrix protein expression was only modestly affected. (D) Viral growth curve on Vero cells. The cells were infected at an MOI of 0.05 PFU with ConVac, or VSV expressing GFP or another control virus expressing Hendra virus glycoprotein. Supernatants were collected 12, 24, and 36 hours post-infection and titrated on Vero E6 cells.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Robust humoral response
The ConVac vaccine candidate was then tested for immunogenicity and efficacy in the hamsters. With a single dose of vaccine, followed by intranasal challenge with SARS-CoV-2, the hamsters responded with IgG production against the S1 subunit.
The vaccine was found to elicit a Th1-biased humoral immune response, as shown by the measured IgG2/3 titers. A robust neutralizing response was also observed, with a mean titer of 1:370.
Protection against viral lung replication
On day 3 post-challenge, the viral load in the lungs and nose was found to be high in almost all controls. In 4/5 vaccinated hamsters, viral loads were undetectable in the lung, while one had an infectious virus but at a level 645-fold lower than in controls.
Thus, only one vaccinated hamster had detectable SARS-CoV-2 virus in the lungs on day three post-challenge, indicating vaccine efficacy. This animal had the lowest neutralizing antibody titer of all vaccinated hamsters.
The virus was either absent or present at 57-fold lower levels in the nose than in the controls, but no statistical significance is attached to this finding.
After 15 days, the vaccinated and challenged hamsters were found to have less weight loss and signs of clinical disease relative to controls. The virus was not detected in the lungs and nose of either vaccinated or control hamsters at this point.
No evidence of antibody-dependent enhancement
In both groups, the lungs showed signs of interstitial pneumonia on day 3. The ConVac group showed moderate inflammation, unlike the extensive consolidation and inflammation in the controls. The airway in the former showed mild inflammatory changes, unlike the obstruction seen in the latter group.
By day 15, controls showed interstitial pneumonia with airway occlusion, which was present in the vaccine group but to a less severe extent. Septal thickening and airway infiltration with inflammatory cells was observed in both groups. No disease enhancement was apparent in the ConVac group.
Two animals in the vaccinated group were euthanized on day 10 and day 11, respectively, because of an unknown disease. The researchers suggest the possibility of neurological vaccine-induced disease due to the high dose of vaccine virus used in the study.
Conclusion
"Our data show that the VSV-vectored SARS-CoV-2 vaccine based only on the S1 subunit induces a high titer of serum neutralizing antibodies and protects hamsters from SARS-CoV-2."
Further testing will allow more accurate predictions to be made regarding the outcome of vaccination and subsequent exposure to the virus in humans.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Malherbe, D. C. et al. (2021). A single dose of replication-competent VSV-vectored vaccine expressing SARS-CoV-2 S1 protects against virus replication in a hamster model of severe COVID-19. bioRxiv preprint. doi: https://doi.org/10.1101/2021.01.29.428442, https://www.biorxiv.org/content/10.1101/2021.01.29.428442v1
- Peer reviewed and published scientific report.
Malherbe, Delphine C., Drishya Kurup, Christoph Wirblich, Adam J. Ronk, Chad Mire, Natalia Kuzmina, Noor Shaik, et al. 2021. “A Single Dose of Replication-Competent VSV-Vectored Vaccine Expressing SARS-CoV-2 S1 Protects against Virus Replication in a Hamster Model of Severe COVID-19.” Npj Vaccines 6 (1). https://doi.org/10.1038/s41541-021-00352-1. https://www.nature.com/articles/s41541-021-00352-1.