A simulation-based study conducted at the Miami University, USA, has revealed that vaccination of the general population against coronavirus disease 2019 (COVID-19) alone is not sufficient to control the pandemic, given the current availability and implementation strategies. To override the current infection rate of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), strict implementation of non-pharmacological control measures should continue along with mass vaccination programs. The study is currently available on the medRxiv* preprint server.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Background
The United States of America is among the worst-hit countries by the ongoing COVID-19 pandemic. According to the World Health Organization, of 104.8 million global SARS-CoV-2 infection and 2.28 million COVID-19-related deaths, the USA alone accounts for more than 26 million cases and over 450,000 deaths. Moreover, there is evidence suggesting that the pandemic has reduced US residents' life expectancy by more than a year, which is 10-times more severe than the reduction observed during the opioid epidemic.
During the early phase of the COVID-19 pandemic, non-pharmacological control measures were considered the best possible way of curbing the viral spread. These measures mostly include facemask-wearing, hand washing, social distancing, movement restrictions, contact tracing, and quarantine strategies. However, in the later phase of the pandemic, several potential vaccines have started rolling out in many countries, which raises hope for returning to normal life amid the pandemic situation. In the USA, the FDA has recently approved two COVID-19 vaccines for limited and emergency use.
In the current study, the scientists have evaluated the effectiveness of nation-wide COVID-19 vaccination programs, public acceptability for vaccines, and the daily vaccine capacity under two federal plans proposed by the former Trump administration and the Biden administration. Moreover, they assessed the correlation between non-pharmacological control measures and vaccines in managing the COVID-19 pandemic.
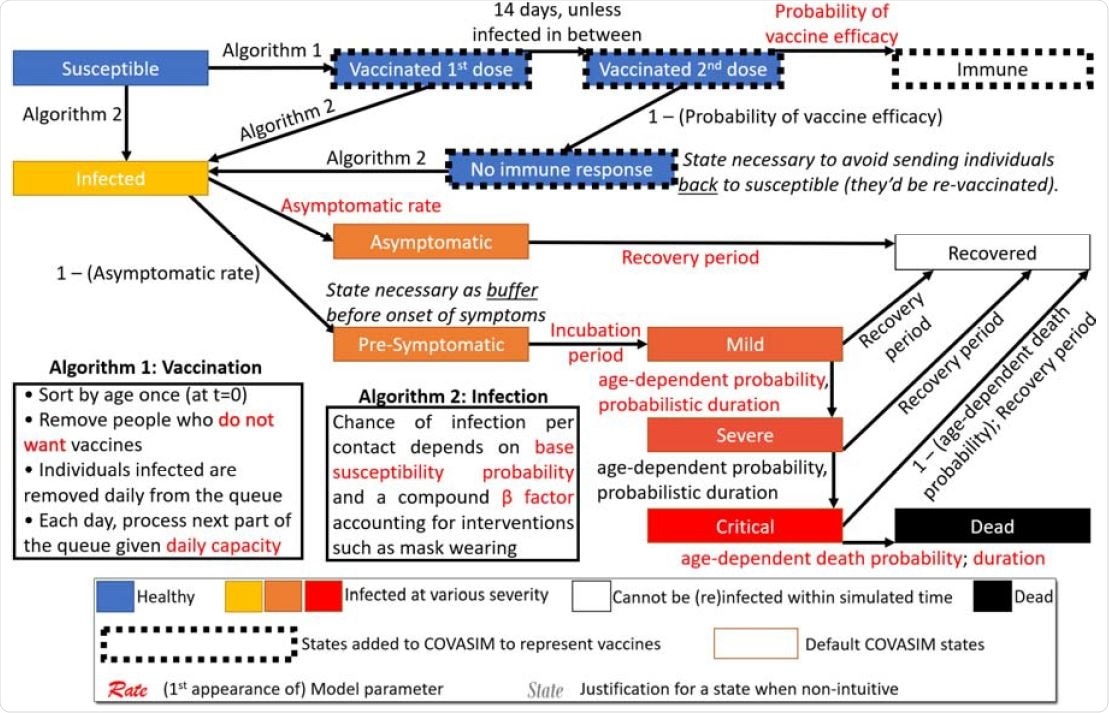
Overview of our modified COVASIM model containing the state diagram and specification of all transitions, including key procedures for vaccination and infection.
Study design
In the current study, the scientists conducted large-scale individual-level simulations by extending a validated open-source agent-based COVID-19 model (COVASIM) with vaccine efficacy, implementation capacity, and public acceptability. Using the model, they simulated the need for two vaccine doses and the probability of acquiring infection before receiving the 2nd dose. Also, they explored whether there is an association between vaccination interventions and non-pharmacological interventions in managing the pandemic situation.
Important observations
The comparison between two federal plans revealed that the Biden plan (1 million vaccine doses/day) is more effective in controlling SARS-CoV-2 infection than the plan generated by the previous Trump administration ("Operation Warp Speed"). According to the simulation data, the planned vaccination regimens can significantly reduce the number of COVID-19 cases even if there is inadequate public willingness toward vaccines and even if they have lower efficacy than expected. Between vaccine efficacy and vaccine compliance/acceptability, it was observed that augmenting vaccine efficacy can significantly reduce infection rate and induction in the proportion of immune people in a given population, which is vital for achieving herd immunity. In contrast, predictions made on vaccine acceptability showed more complex results.
Specifically, the scientists hypothesized that increased vaccine acceptability is associated with a reduced infection rate. However, the simulation data mostly showed reversed outcomes for both vaccination plans, especially in conditions with the lowest restrictions on non-pharmacological control measures. The scientists believe that since vaccination programs mostly plan to immunize elderly populations with much fewer social interactions than the younger population, the actual impact of vaccination in reducing the viral spread is mostly nullified. Another reason for such reversed outcomes could be low vaccine availability. In both situations, the risk of infection transmission continues to rise for the younger population until they become eligible for vaccination. This can lead to an overall induction in infection rate in a given population.
Study significance
The study findings reveal that although effective in reducing the infection rate, vaccination programs alone cannot control the pandemic trajectory. In a situation where non-pharmacological control measure is mostly relaxed, attainment of herd immunity only through vaccination is difficult. Similarly, in situations with no restriction on control measures, higher public compliance toward vaccination results in a higher infection rate, mostly because of low vaccine availability and/or the priority on vaccinating the elderly population. Thus, even with the progression of vaccination programs, the implementation of non-pharmacological control measures should strictly continue to regain a normal life condition amid the pandemic.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources