Researchers in the United States, Germany and Uganda have conducted a study showing that the factors responsible for a higher rate of coronavirus disease 2019 (COVID-19) mortality among males are specific to COVID-19 rather than related to men’s shorter life expectancy.
Pascal Geldsetzer from Stanford University in California and colleagues showed that the sex difference in age-standardized COVID-19 mortality was substantially larger than is seen for most other common causes of death.
The sex difference was particularly significant among older age groups, especially those aged 80 years and older.
The team says the findings support the hypothesis that causal pathways linking male sex to higher COVID-19 mortality are not related to those responsible for a shorter life expectancy among men or a higher mortality rate among men due to other causes.
Geldsetzer and colleagues say that a combination of biological, behavioral, and social pathways may be responsible. Identifying these causal chains could facilitate the development of therapeutics and preventive measures for COVID-19 and future coronavirus outbreaks, they add.
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
A higher risk of death among men has been observed since the pandemic began
Since the COVID-19 outbreak first began in Wuhan, China, in late 2019, researchers have observed a higher risk of death from the disease among men than among women.
However, it is not yet clear whether the observed sex difference in COVID-19 mortality is simply a reflection of men’s shorter life expectancy or specific to infection with the causative agent severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
Geldsetzer and colleagues say the sex difference is substantially larger than would be expected if it could be explained by the causal pathways that link male sex to a shorter life expectancy, thereby suggesting that other pathways may be involved.
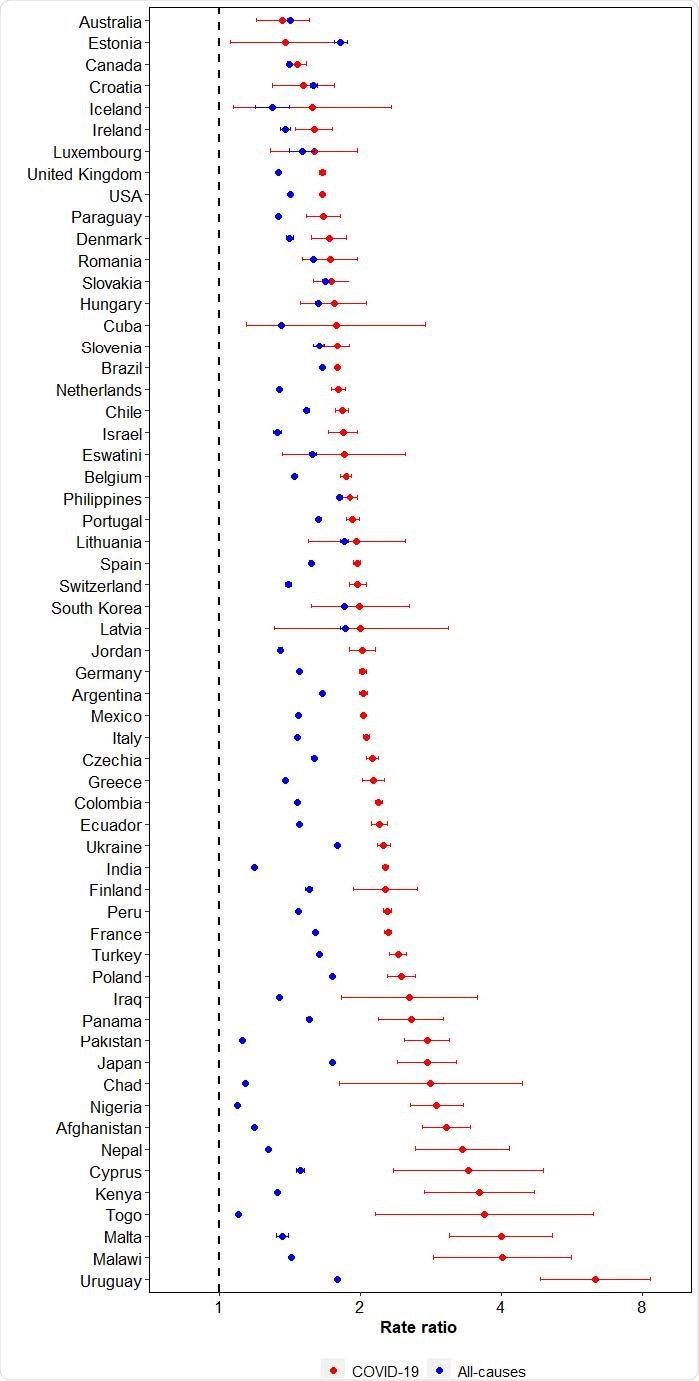
Male-to-female rate ratios of mortality from COVID-19 and all causes. Caption: Rate ratios for the sex differences in COVID-19 and all-cause mortality were calculated for each country by dividing the age-standardized mortality rate in males by the age-standardized mortality rate in females.
What did the researchers do?
The researchers set out to determine whether the size of the sex difference in COVID-19 mortality is any larger than the difference observed for other common causes of death, including other respiratory diseases.
“In doing so, we aim to provide evidence as to whether the causal pathways for the sex differences in the mortality rate of COVID-19 likely differ from those for other causes of death,” they write.
The team says this information is crucial since it could help determine whether the higher COVID-19 mortality rate among men reflects a survival advantage among females and the pathways responsible for this advantage.
“Understanding these causal pathways could help in the development of therapeutics and preventive measures for COVID-19 and future coronavirus disease outbreaks,” says Geldsetzer and colleagues.
The team extracted the latest available country-level age- and sex-aggregated data on COVID-19 mortality from the open-access database COVerAGEDB, which includes cumulative counts of confirmed COVID-19 cases and deaths.
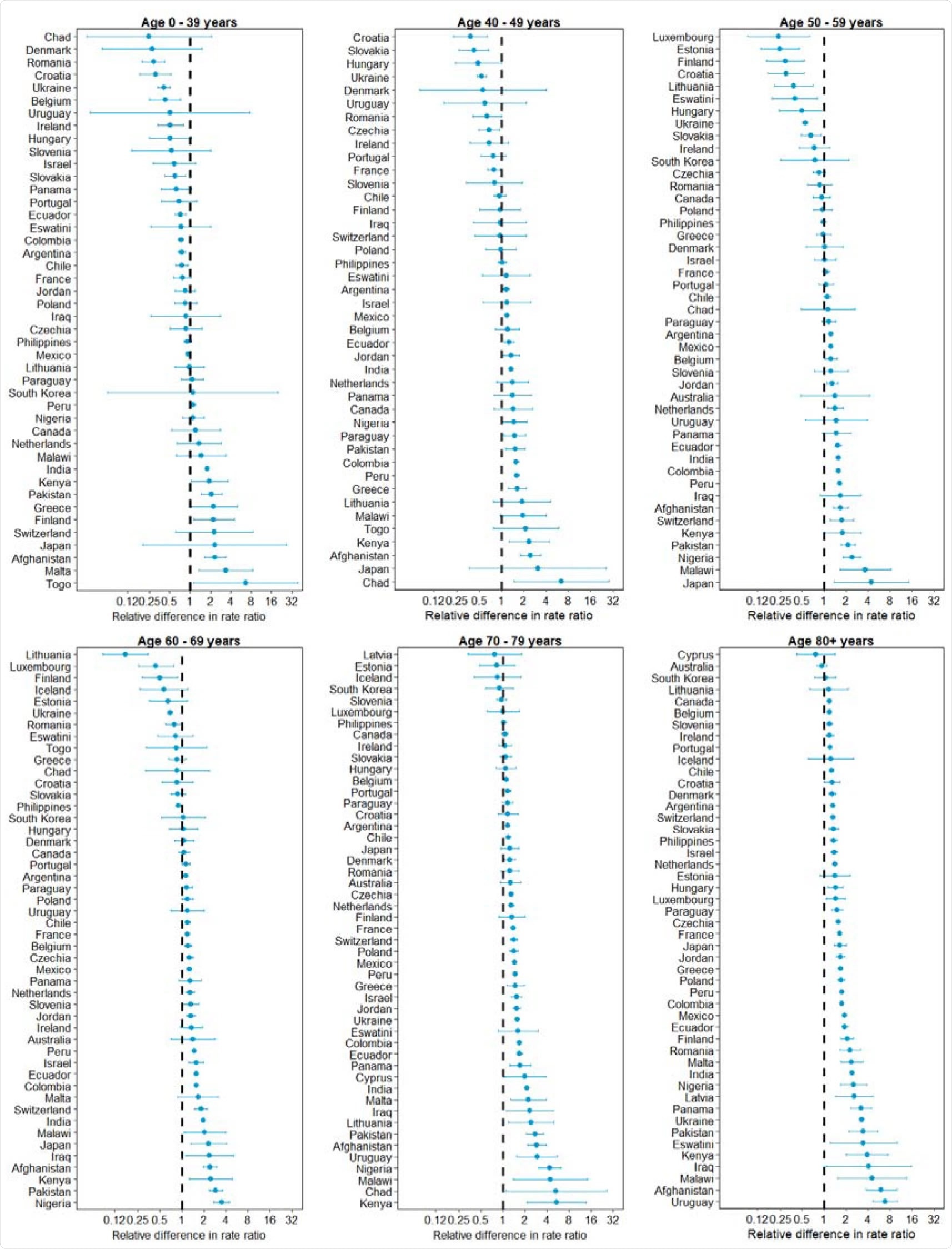
Relative difference in the male-to-female rate ratios of COVID-19-specific and all-cause mortality, by age group. The relative difference in the rate ratio was calculated by dividing (separately among each age group shown) the male-to-female rate ratio for the COVID-19-specific mortality rate by the male-to female rate ratio for the all-cause mortality rate.
Age- and sex-disaggregated data on all-cause mortality and population size were also obtained for each of the countries from the Human Mortality Database and the United Nation’s World Population Prospects.
The latest available data on specific causes of death were obtained from the World Health Organization’s mortality database.
The researchers used these data to calculate the age-standardized male-to-female rate ratios of COVID-19 mortality, all-cause mortality and other significant causes of mortality, including cancer, circulatory diseases, diabetes, respiratory diseases, and neurologic disorders.
What did the study find?
For most countries, the sex difference in age-standardized mortality rate was substantially larger for COVID-19 than for all-cause mortality and most other common causes of death.
This difference was especially large among older age groups, particularly those aged 80 years and older.
The team says their findings support the hypothesis that the causal pathways linking male sex to higher COVID-19 mortality are specific to SARS-CoV-2 and not related to those that link male sex to a shorter life expectancy or higher mortality rates in other common causes of death.
“Ultimately a combination of biological, behavioral, and social pathways may be responsible for the high male disadvantage in COVID-19 mortality,” write the researchers.
“Elucidating these causal chains is important, given that it may assist in the development of therapeutics and preventive measures for COVID-19 and future outbreaks of coronavirus diseases,” they conclude.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources