Despite the rapid pace at which vaccines have been administered throughout the United States, only about 52% of the population has received at least one dose of the coronavirus disease 2019 (COVID-19) vaccine. With vaccine rollouts all over this country, only about half the adult population has been vaccinated so far with at least one dose. Comparatively, a little over 42% of Americans have been fully vaccinated as of June 8, 2021.
 Study: The Impact of COVID-19 Vaccination on California's Return to Normalcy. medRxiv preprint. Image Credit: Chansom Pantip / Shutterstock.com
Study: The Impact of COVID-19 Vaccination on California's Return to Normalcy. medRxiv preprint. Image Credit: Chansom Pantip / Shutterstock.com

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Background
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) that emerged towards the end of 2019 is the latest pathogenic human coronavirus to appear over the last two decades. It has caused widespread devastation, with millions of severe or critical patients succumbing to COVID-19.
The adoption of large-scale non-pharmaceutical interventions (NPIs) such as sheltering in place, social distancing while outside the home, the wearing of face masks, and limitations on public gatherings significantly reduced the social lives of people around the world. However, with the roll-out of a score of vaccines in the first quarter of 2021, people everywhere are anticipating the early re-opening of public spaces.
California planned its pandemic strategy based on the Blueprint for a Safer Economy. This guide to navigating a pandemic is based on test positivity rates, viral caseload, and the overall threat of viral transmission, hospital burden, and death rate. Based on these county-specific threat rates, the local authorities mandate NPIs, operative hours and modes for businesses, as well as population-level safety advice.
The California Department of Public Health (CDPH) subsequently published their version of Beyond the Blueprint for a Safer Economy, which is dependent upon case levels, vaccine uptake, and equity assessments to safely reopen the economy by the aforementioned date. The key criteria that must be fulfilled before the state can reopen include:
- A sustained pace of vaccination, which requires adequate facilities and resources.
- Surveillance for new cases and strains, particularly in the most underserved parts of the state.
- Preparedness planning state-wide.
- Strong containment testing and investigation of local outbreaks.
Twin pillars of endemicity
This exit strategy is aimed at ensuring the virus becomes endemic, during which SARS-CoV-2 would circulate at a low level rather than in deadly waves. However, to force a virus to become endemic, the two parameters of transmissibility and effective susceptible population size are critical.
The first is not under human control and is instead a biological feature of the virus as it interacts with the host population genes, immune response, and pharmaceutical interventions. Such interactions may promote the emergence of variants of concern, which are more infectious or resist neutralization by pre-existing antibodies.
In addition to the threat posed by recent mutated variants of SARS-CoV-2, people are likely to resume gatherings that include unvaccinated people. Furthermore, people will likely stop wearing masks and social distancing once restrictions are lifted, or simply because of pandemic fatigue. Taken together, these factors promote an increase in viral transmission.
The effective population includes everyone who has not recovered from an infection, those who have lost adequate levels of immunity, and those with breakthrough infection after vaccination. Additionally, those who have never been infected or immunized are also at risk of being infected.
What are the findings?
Using a model that updates these two model parameters dynamically, the current study sought to better reflect real-world trends.
At baseline values, with vaccination stopping where they are right now, reopening will likely lead to about 11,500 more cases and approximately 430 deaths within the first 15 days in the state of California.
At the current rate of vaccinations, if the rates of viral spread are higher than baseline during this period, deaths would increase by 4%, whereas cases would likely increase by at least 20%. At a rate equal to the peak in this state (0.5), predicted cases and deaths would be double those at baseline.
With an increase in the susceptible population following reopening, cases are likely to increase by more than half, with the number of deaths increasing by 12% relative to the baseline. If coupled with a 30% reduction in vaccination rates, cases may almost double, with well over a third more deaths.
This could happen both because of increased mixing of susceptible and infectious people from different communities or because of the emergence of new strains that are resistant to existing antibodies.
With the transmission rate remaining steady, if vaccination falters by 30%, cases would still increase from the baseline by over a third, and deaths by over a fifth. The reverse trend, with a 30% increase in vaccine uptake, would bring down deaths by approximately 18%, and avert over a quarter of the cases at baseline.
If both vaccine uptake and transmission rates increase by 30% and to 0.4, respectively, cases would reduce by a tenth, while one in seven deaths could be prevented. However, a 30% decrease in vaccine uptake would push up cases by two-thirds.
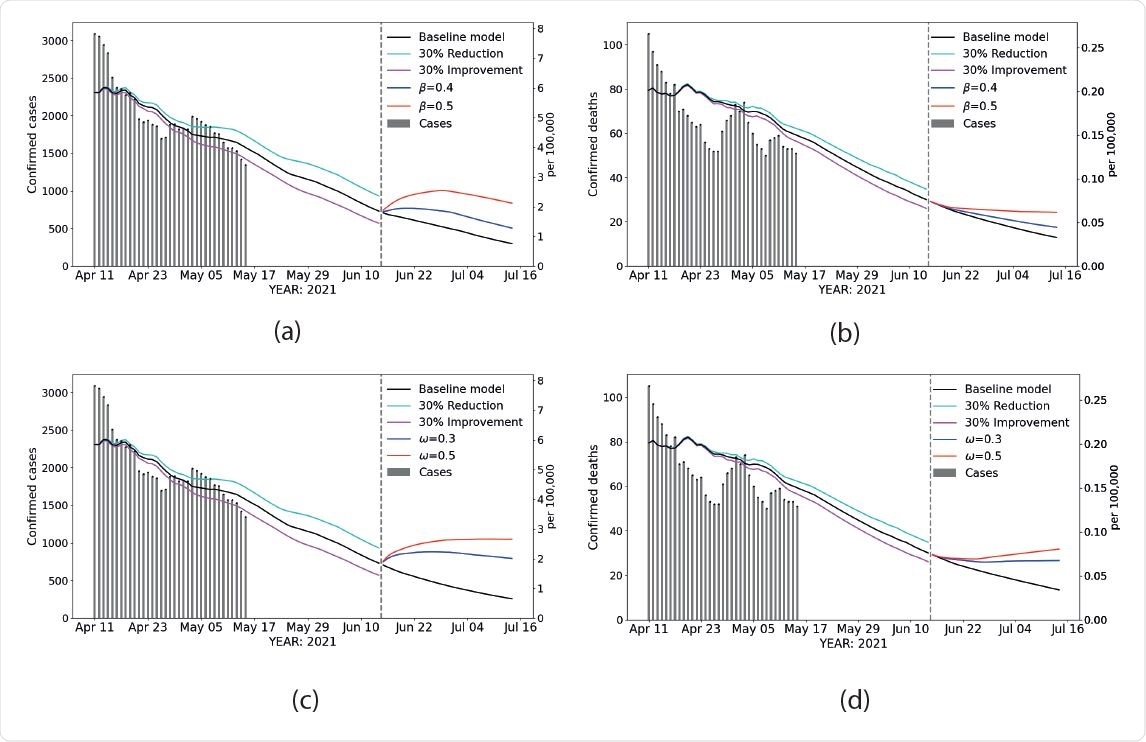
Scenarios Estimated statewide confirmed cases and confirmed deaths during live data collection, extrapolated between May 18th and June 15th for different vaccination rates, and predicted beyond June 15th with different effective susceptible populations and transmission rates. (a) and (b): effects of varying transmission rate on confirmed cases and confirmed deaths, respectively. (c) and (d): effects of varying effective susceptible populations on confirmed cases and conffrmed deaths, respectively. Dashed vertical line: June 15th. Gray vertical bars: daily reported data. Black line: baseline scenario, before and after opening. Cyan line: projection from May 18th assuming a 30% reduction in the current vaccination rate. Magenta line: projection from May 18th assuming a 30% increase in the current vaccination rate.
What are the implications?
At present, both case and mortality rates are predicted to continue to steadily decline. Increases in either transmission rates or the number of susceptible people can tip this in the opposite direction, with low-level spread persisting in the population. This is more likely to occur with a reduction in vaccine rates.
If both increase, the model predicts another wave of cases. This is more likely when the virus is causing a consistently low number of cases. The reason is that local outbreaks may be missed in this situation, as the mean data ranges remain stable.
“The greater the number of outbreaks and the greater their severity, the more likely a new strain is to emerge.”
With reopening being planned within a week, it is absolutely essential to send the right public health messages. These messages should support the continued practice of that social distancing and the use of face masks in public. It is critical to continue these practices until communities, where vaccination has been particularly uneven, are covered adequately.
Moreover, warning signs that the exit strategy is not working as planned include increasing rates of reinfections, breakthrough infections, and more severe disease among children. These must be actively monitored for months, perhaps years, before the risk of a resurgence can truly be avoided.
“The Centers of Disease Control's (CDC) recommendation to ease mask-wearing for fully vaccinated individuals despite major inequities in vaccine uptake in counties across the state highlights some of the logistical challenges that society faces as we enthusiastically phase-out of this pandemic.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Daza-Torres, M. L., Garcia, Y. E., Schmidt, A. J., et al. (2021). The Impact of COVID-19 Vaccination on California's Return to Normalcy. medRxiv preprint. doi:10.1101/2021.06.01.21258187. https://www.medrxiv.org/content/10.1101/2021.06.01.21258187v1.
- Peer reviewed and published scientific report.
Daza–Torres, Maria L., Yury E. García, Alec J. Schmidt, Brad H. Pollock, James Sharpnack, and Miriam Nuño. 2022. “The Impact of COVID-19 Vaccination on California’s Return to Normalcy.” Edited by Charles Shey Wiysonge. PLOS ONE 17 (5): e0264195. https://doi.org/10.1371/journal.pone.0264195. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0264195.