The coronavirus disease (COVID-19) pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), continues to spread across the globe. With the progression of the pandemic, our understanding of the post-COVID-19 syndromes continues to expand.
There is evidence to suggest that death rates from COVID-19 are higher in men than in women. On the other hand, women seem more likely to suffer the disease's long-term effects and experience negative social and economic consequences.
To better understand post-COVID sequelae, researchers at the University Hospital Basel and the University Hospital Zurich conducted a multicentre prospective observational cohort study.
The study, which appeared in the pre-print server medRxiv*, highlights the sex and gender-specific risk factors of post-COVID-19 syndrome in Switzerland.
COVID-19 and long-term consequences
Some people who were infected with SARS-CoV-2 experience signs and symptoms even after they recovered from the illness. Called long haulers or long COVID, these individuals may experience fatigue or tiredness, difficulty thinking or concentrating, headache, dizziness when standing, palpitations, chest pains, shortness of breath, and the loss of smell or taste.
Identifying risk factors
In the current study, the researchers aimed to determine if women are at a higher risk of developing long-term complications.
They conducted a multicenter prospective observational cohort study (Swiss COGEN Cohort study) of more than 5,800 people in Switzerland who tested positive for SARS-CoV-2 RNA from February to December 2020. About 2,799, who are survived, completed a follow-up questionnaire.
The primary outcome of measure is the persistence of at least one COVID-19 related symptom for more than 60 days. The secondary outcome measures included the current quality of life compared to before the COVID-19 disease diagnosis, being readmitted to the hospital, and the nature of persistent symptoms. These symptoms included difficulty of breathing, physical weakness, chest pain, joint pain, loss of smell or taste, skin changes, palsy, visual problems, excess salivation, memory problems, and headache, among others.
In the patient cohort, the most common risk condition was hypertension, followed by obesity. Meanwhile, cardiovascular disease, including coronary artery disease, cardiomyopathy, and valvular heart disease, was present in 304 patients. On average, men were older than women in the cohort.
Of the 2,799 people who tested positive for SARS-CoV-2 and survived, 2,336 were outpatients, 16.5 percent were inpatients, where 165 women and 117 men were admitted to an intermediate or intensive care unit (ICU).
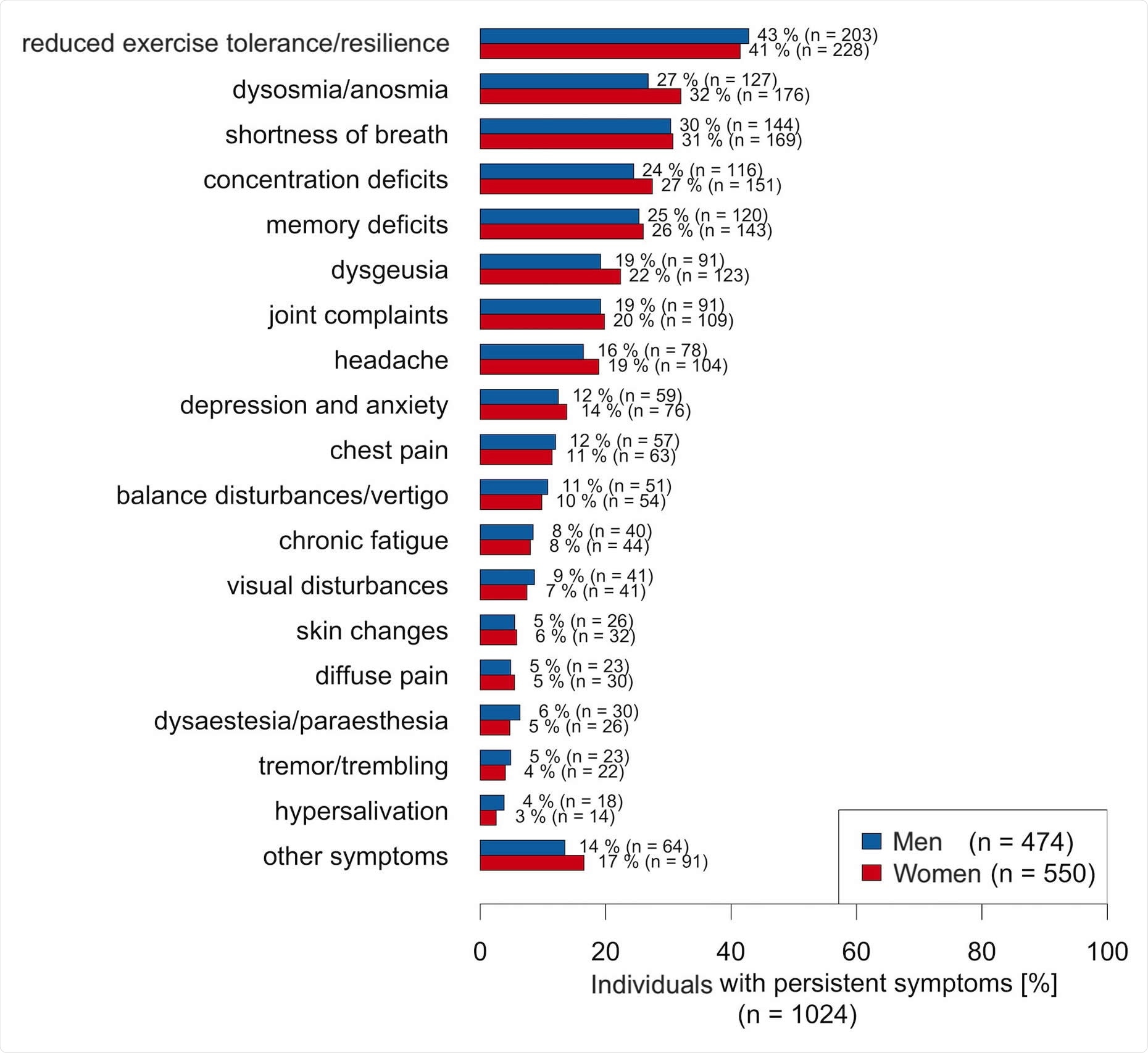
Women at higher risk

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
During the mean follow-up time of 197 days, 36.8 percent of the individuals reported at least one persistent symptom. Also, of the 152 people hospitalized at least once for persistent symptoms, 66 were women and 86 men.
An estimated 43 percent of women and 32 percent of men reported at least one persistent symptom months after their acute infection. The number of symptoms per individual was higher in women. Further, pre-existing mental health conditions and cardiovascular risk factors increased the risk of post-COVID-19 syndrome in women but not in men.
Obesity was an independent predictor of post-COVID-19 syndrome in men, but not in women. Domestic stress level and self-assessed gender identity heightened the likelihood of long-term COVID-19 complications in women. On the contrary, pregnancy during the acute COVID-19 illness and responsibility for taking care of the children seemed to protect women from post-COVID-19 syndrome.
"Our data indicate that post-COVID-19 sequelae and their predictors differ between men and women, suggesting that a tailored and sex- and gender-sensitive approach of healthcare services may be required to support their needs," the team explained in the study.
"Sex- and gender-specific research on the underlying pathophysiology of post-COVID-19 syndrome is now urgent to better understand symptom development and identify targets for intervention," they added.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.