Researchers at the University of Oxford have conducted a study showing that vaccination against coronavirus disease 2019 (COVID-19) is associated with a lower risk of several sequelae among those who experience breakthrough infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
Maxime Taquet and colleagues say that while it is already established that vaccination protects against COVID-19 hospitalization, ICU admission, and death, little is known regarding the effect of immunization on other outcomes of breakthrough SARS-CoV-2 infection.
Now, using data from a large-scale electronic health records network, the team has shown that immunization with at least one vaccine dose is also associated with a lower risk of other acute and post-acute outcomes following breakthrough infection that have not been assessed in previous studies.
Examples of these additional outcomes include respiratory failure, hypoxemia, oxygen requirement, venous thromboembolism, seizures, psychotic disorder, and hair loss.
On the other hand, previous vaccination does not appear to be protective against several previously documented outcomes such as long-COVID features, arrhythmia, joint pain, sleep disorders, and mood and anxiety disorders.
The team also says that while the benefits of vaccination were clear for younger individuals, they were not clear for those aged 60 years or older.
The researchers say the findings may help to inform service planning, forecast public health impacts of vaccination, and highlight the need to identify additional interventions for COVID-19 sequelae.
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Breakthrough SARS-CoV-2 infections among the vaccinated has caused alarm
The observation that individuals can experience breakthrough SARS-CoV-2 infection despite being vaccinated against COVID-19 has caused concerns among healthcare professionals and the public.
These concerns have been mitigated to a degree by evidence showing that the risk of severe disease (resulting in hospitalization, ICU admission or death) is lessened by vaccination.
However, it is unclear how COVID-19 vaccination affects the broader outcomes of SARS-CoV-2 infection such as venous thromboembolism, ischemic stroke, neuropsychiatric complications, and long-COVID. Furthermore, unvaccinated people may have health behaviors related to vaccination hesitancy that could confound associations with these outcomes.
What did the researchers do?
Taquet and colleagues obtained data from the TriNetX electronic health records network that covers more than 81 million patients, mainly in the United States.
They compared six-month outcomes of SARS-CoV-2 infection among individuals who had received a COVID-19 vaccine prior to infection with those among propensity score-matched individuals who were not vaccinated against COVID-19, but who had received an influenza vaccine. This influenza vaccination criterion helped control for the confounding effect of vaccine hesitancy and related health behaviors.
Vaccinated patients were only included if they had become infected with SARS-CoV-2 at least 14 days after administration with one of the Pfizer-BioNTech (BNT162b2), Moderna (mRNA-1273) or Janssen (Ad26.COV2.S) vaccines approved for use in the United States.
Outcomes were ICD-10 (International Classification of Diseases 10th Revision) codes representing 45 documented COVID-19 sequelae that were recorded between January 1st and August 31st, 2021.
What did the study find?
Among 10,024 vaccinated individuals with SARS-CoV-2 infection, 9,479 were matched to unvaccinated controls.
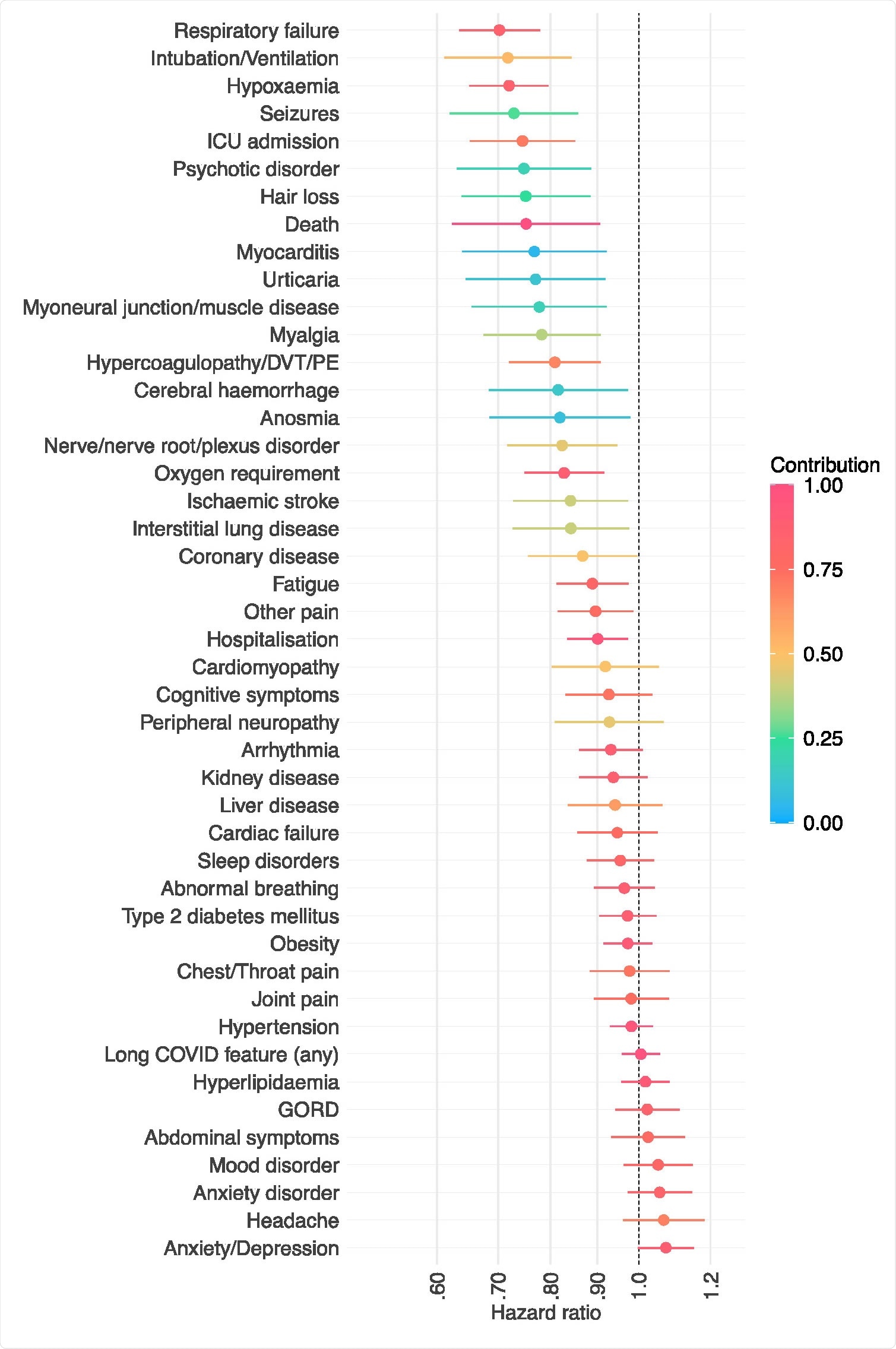
Hazard ratios for the outcome within 6 months of infection with SARS-CoV-2 between individuals vaccinated vs. unvaccinated against COVID-19. HR lower than 1 indicates outcomes less common among vaccinated individuals. Horizontal bars represent 95% confidence intervals. Each outcome is a composite endpoint with death as a component to address competing risks. The contribution of the outcome of interest to the overall incidence of the composite endpoint is encoded by the color.
Administration of at least one COVID-19 vaccine dose was associated with a significantly lower risk of various SARS-CoV-2 sequelae including respiratory failure, ICU admission, hypoxemia, oxygen requirement, ventilation, hypercoagulopathy or venous thromboembolism, seizures, psychotic disorder, and hair loss.
On the other hand, previous vaccination was not associated with a lower risk for several previously documented outcomes, including long-COVID features, arrhythmia, joint pain, kidney, disease, type 2 diabetes, liver disease, anxiety disorder and mood and sleep disorders.
Receiving two vaccine doses was associated with an even lower risk for most of the outcomes. The associations between prior vaccination and outcomes of infection were marked in those aged under 60 years, whereas no robust associations were observed among those aged 60 years or older.
What are the implications of the findings?
Taquet and colleagues say the data suggest that COVID-19 vaccination, especially two doses, is associated with a significantly lower risk for several, but not all, COVID-19 sequelae in younger individuals with breakthrough SARS-CoV-2 infection.
The benefits of vaccination were not clear among older people, which is an essential factor since this group is at an increased risk of most adverse outcomes following infection, they add.
“The findings can help in determining the necessary service provision and underlines the urgency to identify other preventive or curative interventions to mitigate the impact of such sequelae of COVID-19,” concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Taquet M, et al. Six-month sequelae of post-vaccination SARS-CoV-2 infection: a retrospective cohort study of 10,024 breakthrough infections. medRxiv, 2021. doi: https://doi.org/10.1101/2021.10.26.21265508, https://www.medrxiv.org/content/10.1101/2021.10.26.21265508v1
- Peer reviewed and published scientific report.
Taquet, Maxime, Quentin Dercon, and Paul J. Harrison. 2022. “Six-Month Sequelae of Post-Vaccination SARS-CoV-2 Infection: A Retrospective Cohort Study of 10,024 Breakthrough Infections.” Brain, Behavior, and Immunity 103 (July): 154–62. https://doi.org/10.1016/j.bbi.2022.04.013. https://www.sciencedirect.com/science/article/pii/S0889159122001118.