There are vast differences in the mortality rate and toll of coronavirus disease 2019 (COVID-19), most likely due to demographic, climatic, or social factors. Even so, there are likely to be additional factors contributing to the variation in disease outcomes at the local level.
Identifying these factors may aid in forecasting trajectories of pandemics, which may lead to non-pharmaceutical interventions and research directions in the development of novel therapeutic and immunological strategies.
The interactions of the host with non-pathogenic microbes in the environment also significantly modulate disease outcomes, including those of COVID-19.
In general, environmental microbes that enhance health outcomes harbor certain features:
- Environmental microbes having beneficial effects often originate from soils, freshwater environments, plants, and other non-anthropogenic sources – potentially reflecting a history of human evolutionary adaptation to them
- These microbes reduce disease severity by stimulating the immune system early in life
- Exposure to various environmental microbes is necessary to confer beneficial effects
Functional immune response is essential for moderating outcomes of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. In addition, evidence suggests that COVID-19 disease severity correlates with bacterial community composition in patients and the hospital environment and with dysbiosis of the lung and the gut microbiomes.
A new study published on the medRxiv* preprint server was based on the hypothesis that the environmental mycobiome (fungi) is a likely important factor in determining area-level variation in COVID-19 mortality.
 Study: The impact of environmental mycobiomes on geographic variation in COVID-19 mortality. Image Credit: Kateryna Kon / Shutterstock
Study: The impact of environmental mycobiomes on geographic variation in COVID-19 mortality. Image Credit: Kateryna Kon / Shutterstock

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
The study
The present study utilized taxonomic information on fungal communities from 1,135 homes nationwide, as well as COVID-19 data from across the United States. Paired samples were collected from each house—indoors and outdoors—allowing for comparison. An innovative approach was used to estimate the number of SARS-CoV-2 deaths per 1,000 infections in each county in the United States and in each home which provided fungal data.
Additionally, the influence of demographic, sociological, climate and soil factors was extensively explored, some of which influence Infection Fatality Ratios (IFR) and fungal community composition.
![COVID-19 mortality is suppressed in homes where outdoor fungi occur indoors. (A) In United States homes where indoor and outdoor fungal communities are similar (low beta-diversity), COVID-19 mortality is reduced by over a factor of two compared to homes where the communities are dissimilar (high beta-diversity). Each point represents a United States county; shading indicates point density. Although the 90th percentile is sensitive to spatial autocorrelation, these trends are not driven by a single state or region of the United States (Figures E2 - E4). (B) The reductions in COVID-19 mortality (as measured by the standardized effect size, SES) are greatest in the upper quantiles of the COVID-19 mortality distribution, suggesting that outdoor fungi are sufficient but not necessary to reduce COVID-19 mortality. (C) The association between COVID-19 mortality and fungal beta-diversity is strongest early in the pandemic, before December 2020 when vaccination became widespread. Circles with black outlines indicate significant associations (SES> 3). (D) Fungal beta-diversity is a strong predictor of suppression of SARS-CoV-2 IFR relative to other variables [column graph; points represent individual variables, columns show means; correlations give the association between the given variable and the windowed 75th percentile of IFR (see Supplementary Information)]. Moreover, fungal beta-diversity is most strongly associated with soil pH and other environmental variables (inset bar graph), suggesting that it is not a proxy for demographic and other variables that are known to effect COVID-19 mortality. COVID-19 mortality is suppressed in homes where outdoor fungi occur indoors. (A) In United States homes where indoor and outdoor fungal communities are similar (low beta-diversity), COVID-19 mortality is reduced by over a factor of two compared to homes where the communities are dissimilar (high beta-diversity). Each point represents a United States county; shading indicates point density. Although the 90th percentile is sensitive to spatial autocorrelation, these trends are not driven by a single state or region of the United States (Figures E2 - E4). (B) The reductions in COVID-19 mortality (as measured by the standardized effect size, SES) are greatest in the upper quantiles of the COVID-19 mortality distribution, suggesting that outdoor fungi are sufficient but not necessary to reduce COVID-19 mortality. (C) The association between COVID-19 mortality and fungal beta-diversity is strongest early in the pandemic, before December 2020 when vaccination became widespread. Circles with black outlines indicate significant associations (SES> 3). (D) Fungal beta-diversity is a strong predictor of suppression of SARS-CoV-2 IFR relative to other variables [column graph; points represent individual variables, columns show means; correlations give the association between the given variable and the windowed 75th percentile of IFR (see Supplementary Information)]. Moreover, fungal beta-diversity is most strongly associated with soil pH and other environmental variables (inset bar graph), suggesting that it is not a proxy for demographic and other variables that are known to effect COVID-19 mortality.](https://www.news-medical.net/images/news/ImageForNews_699908_16399736436415824.jpg) COVID-19 mortality is suppressed in homes where outdoor fungi occur indoors. (A) In United States homes where indoor and outdoor fungal communities are similar (low beta-diversity), COVID-19 mortality is reduced by over a factor of two compared to homes where the communities are dissimilar (high beta-diversity). Each point represents a United States county; shading indicates point density. Although the 90th percentile is sensitive to spatial autocorrelation, these trends are not driven by a single state or region of the United States (Figures E2 - E4). (B) The reductions in COVID-19 mortality (as measured by the standardized effect size, SES) are greatest in the upper quantiles of the COVID-19 mortality distribution, suggesting that outdoor fungi are sufficient but not necessary to reduce COVID-19 mortality. (C) The association between COVID-19 mortality and fungal beta-diversity is strongest early in the pandemic, before December 2020 when vaccination became widespread. Circles with black outlines indicate significant associations (SES> 3). (D) Fungal beta-diversity is a strong predictor of suppression of SARS-CoV-2 IFR relative to other variables [column graph; points represent individual variables, columns show means; correlations give the association between the given variable and the windowed 75th percentile of IFR (see Supplementary Information)]. Moreover, fungal beta-diversity is most strongly associated with soil pH and other environmental variables (inset bar graph), suggesting that it is not a proxy for demographic and other variables that are known to affect COVID-19 mortality.
COVID-19 mortality is suppressed in homes where outdoor fungi occur indoors. (A) In United States homes where indoor and outdoor fungal communities are similar (low beta-diversity), COVID-19 mortality is reduced by over a factor of two compared to homes where the communities are dissimilar (high beta-diversity). Each point represents a United States county; shading indicates point density. Although the 90th percentile is sensitive to spatial autocorrelation, these trends are not driven by a single state or region of the United States (Figures E2 - E4). (B) The reductions in COVID-19 mortality (as measured by the standardized effect size, SES) are greatest in the upper quantiles of the COVID-19 mortality distribution, suggesting that outdoor fungi are sufficient but not necessary to reduce COVID-19 mortality. (C) The association between COVID-19 mortality and fungal beta-diversity is strongest early in the pandemic, before December 2020 when vaccination became widespread. Circles with black outlines indicate significant associations (SES> 3). (D) Fungal beta-diversity is a strong predictor of suppression of SARS-CoV-2 IFR relative to other variables [column graph; points represent individual variables, columns show means; correlations give the association between the given variable and the windowed 75th percentile of IFR (see Supplementary Information)]. Moreover, fungal beta-diversity is most strongly associated with soil pH and other environmental variables (inset bar graph), suggesting that it is not a proxy for demographic and other variables that are known to affect COVID-19 mortality.
Findings
It was noted that a majority of the citizens primarily interact with indoor microbes only—as they spend most of their time in their homes or other constructed environments. For fungi, two major types were of concern – non-pathogenic outdoor species (which are sometimes also found indoors) and pathogenic or opportunistic species that proliferate in damp indoor environments. These types elicited notable differences.
The presence of outdoor fungi in the built environment was speculated to be associated with reduced SARS-CoV-2 IFR. Based on the analysis, a marginal impact was observed of the relative abundances of fungal genera or indoor-outdoor beta diversity—after taking into account demographic, sociological, climate and soil factors. While considering the alternative factors, fungal genera relative abundances depicted a statistically significant but small impact on the mean IFR.
Quantile analysis revealed that indoor-outdoor beta-diversity is associated with reduced SARS-CoV-2 IFR, indicating reduced mortality. At the same time, dissimilar indoor and outdoor mycological flora are associated with elevated SARS-CoV-2 IFR. These results were consistent pan-counties.
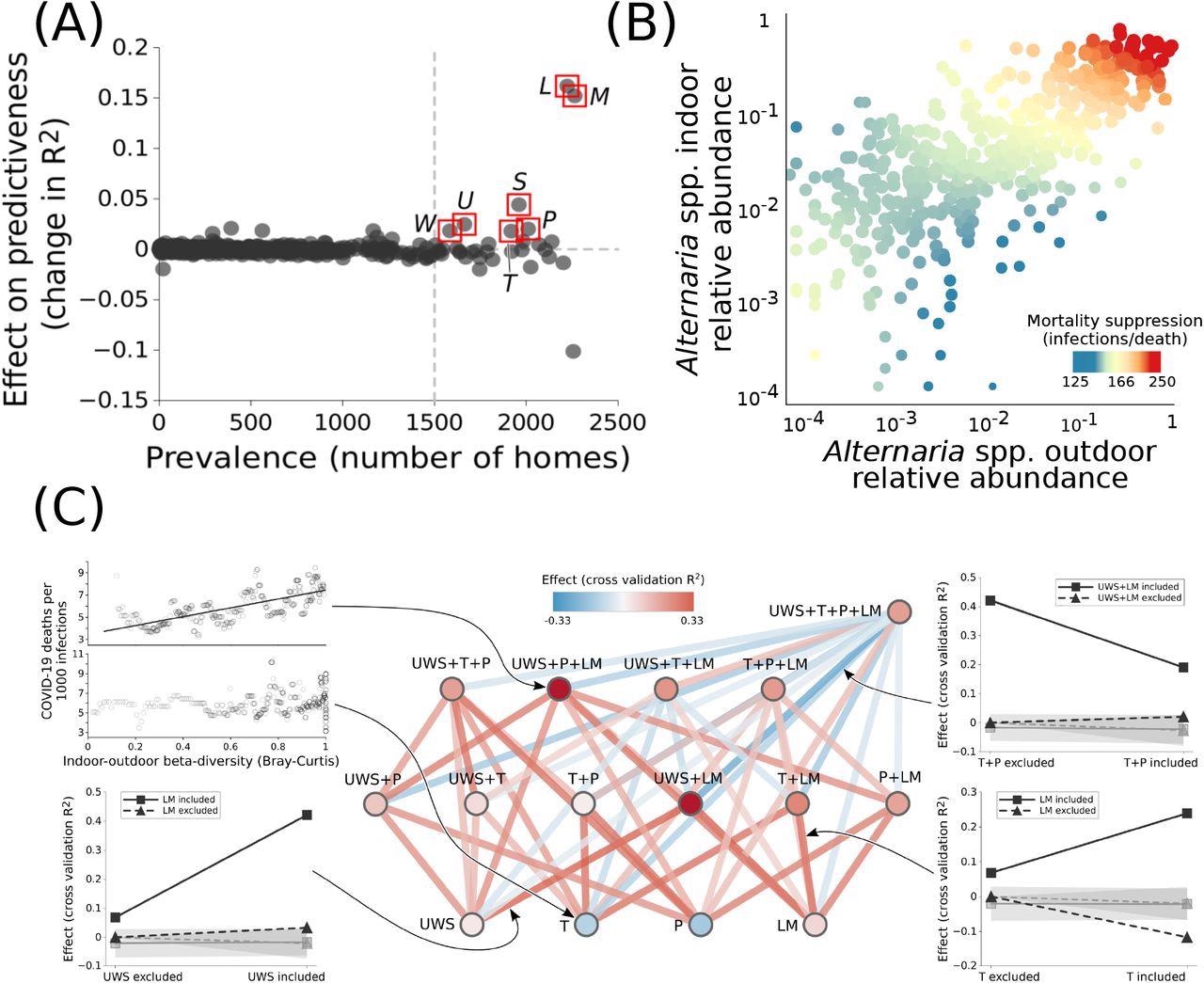 The occurrence of at least four outdoor fungal genera indoors suppresses COVID-19 mortality. (A) Seven prevalent genera significantly increase the predictiveness of indoor-outdoor fungal beta-diversity on COVID-19 mortality. Abbreviations are L: Alternaria, S : Aspergillus, P : Epicoccum, U : Eurotium, T : Toxicocladosporium, W : Wallemia, M : Mycosphaerellaceae genus. (B) For some of these genera, including Alternaria spp., high relative abundance both outdoors and indoors is necessary for suppressed COVID-19 mortality. (C) However, the full beneficial effects result from synergistic effects of multiple genera: vertices represent sets of genera (colored by predictive power), while edges represent interactions when sets of genera are considered jointly as predictors (colored by interaction strength). Genera with correlated relative abundances are grouped together (e.g., LM : Alternaria and Mycosphaerellaceae genus). The graphs around the edges show examples of predictive power and interactions; gray lines demarcate null (randomized) expectations plus or minus one standard deviation. Except for when the full set of genera is considered (top right vertex), super-additive effects dominate, pointing to synergistic effects.
The occurrence of at least four outdoor fungal genera indoors suppresses COVID-19 mortality. (A) Seven prevalent genera significantly increase the predictiveness of indoor-outdoor fungal beta-diversity on COVID-19 mortality. Abbreviations are L: Alternaria, S : Aspergillus, P : Epicoccum, U : Eurotium, T : Toxicocladosporium, W : Wallemia, M : Mycosphaerellaceae genus. (B) For some of these genera, including Alternaria spp., high relative abundance both outdoors and indoors is necessary for suppressed COVID-19 mortality. (C) However, the full beneficial effects result from synergistic effects of multiple genera: vertices represent sets of genera (colored by predictive power), while edges represent interactions when sets of genera are considered jointly as predictors (colored by interaction strength). Genera with correlated relative abundances are grouped together (e.g., LM : Alternaria and Mycosphaerellaceae genus). The graphs around the edges show examples of predictive power and interactions; gray lines demarcate null (randomized) expectations plus or minus one standard deviation. Except for when the full set of genera is considered (top right vertex), super-additive effects dominate, pointing to synergistic effects.
Moreover, the presence of high diversity of outdoor fungi indoors was associated with suppressed COVID-19 mortality, as opposed to lower diversity indoors. This association was valid in the first few months of the pandemic and weaker during the later phases—December 2020 to January 2021—after vaccine availability and in the setting of access to pharmaceutical treatments.
Remarkably, soil edaphic factors – particularly pH, appeared to affect COVID-19 severity by affecting microbial distributions. In addition, a causal link was found between indoor-outdoor fungal beta-diversity and SARS-CoV-2 IFR even after considering other potentially confounding variables.
The results revealed that at least four of these fungal genera play a key role in suppressing SARS-CoV-2 IFR, which are – Alternaria, Aspergillus, Epicoccum, Eurotium, Toxicocladosporium, and Wallemia spp., and a novel Mycosphaerellaceae genus. Some of these have interdependent distributions; hence, it is difficult to distinguish the effects of individual genera. Besides, a high relative abundance of three of these genera both indoors and outdoors is necessary for significant SARS-CoV-2 IFR reduction.
The findings mark a novel illustration of the beneficial effects of seven mycological genera for reducing COVID-19 mortality. Although these genera may be pathogenic in some settings, they may confer positive effects in others.
Furthermore, different species of environmental and endemic microbes from the same genus can have differential effects based on host genetics and age, immune status, and interactions with other microbial exposures.
The seven genera identified in this study reveal positive synergistic effects; the beta-diversity of these genera taken together is strongly predictive. Further, fungal beta diversity was more strongly associated with SARS-CoV-2 IFR suppression in regions with stable human habitation. Hence, these observations could accurately map locations to forecast regions with strong suppression of COVID-19 mortality in the US – the Desert Southwest, Intermountain West, and Upper Midwest.
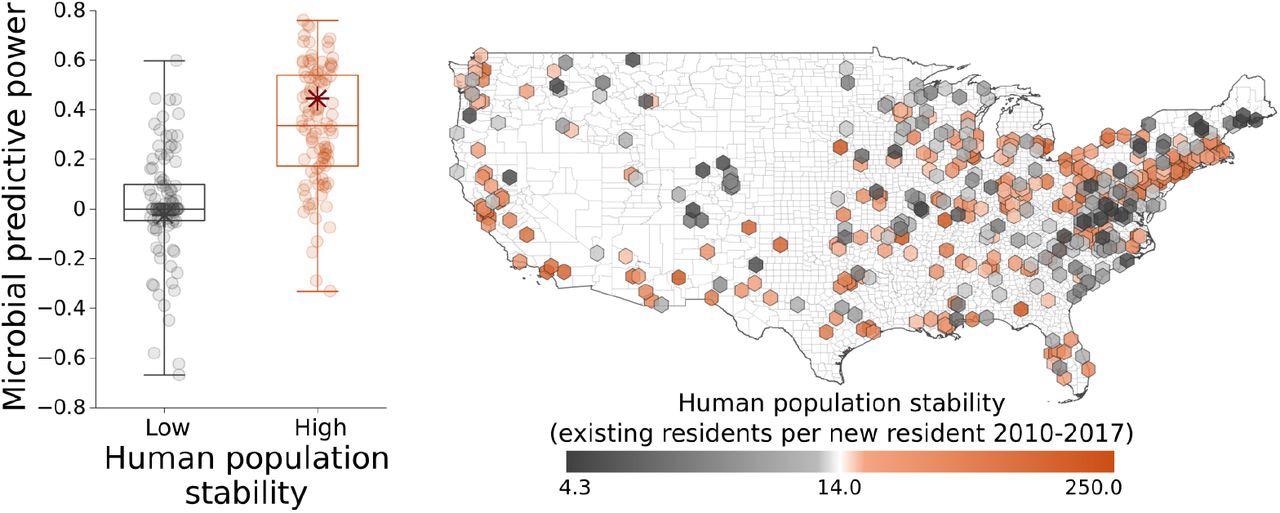 The occurrence of outdoor fungi indoors is more predictive of COVID-19 mortality in locations where people have been less transient from 2010-2017 than in regions where there are many new residents.
The occurrence of outdoor fungi indoors is more predictive of COVID-19 mortality in locations where people have been less transient from 2010-2017 than in regions where there are many new residents.
In addition to the climate in the US, pH may denote the microbial composition and propensity for microbial transport into homes through dust. There is a correlative effect between bioaerosol counts, specifically mold spores, and respiratory disease incidence.
In inference, exposure to high levels of outdoor fungi in homes is protective against poor COVID-19 outcomes. The results underscore the utility of the environmental mycobiome as a biosensor. Moreover, the beneficial effects of environmental fungi may not be specific to COVID-19; it may be relevant for other autoimmune and immune-mediated diseases as well.
Thus, further research on the role of fungi and fungal interactions with the host immune system is warranted. Recent advances in the sequencing and classification of environmental fungi will enhance future efforts in this area and highlight the usefulness of biosurveillance for future pandemics.
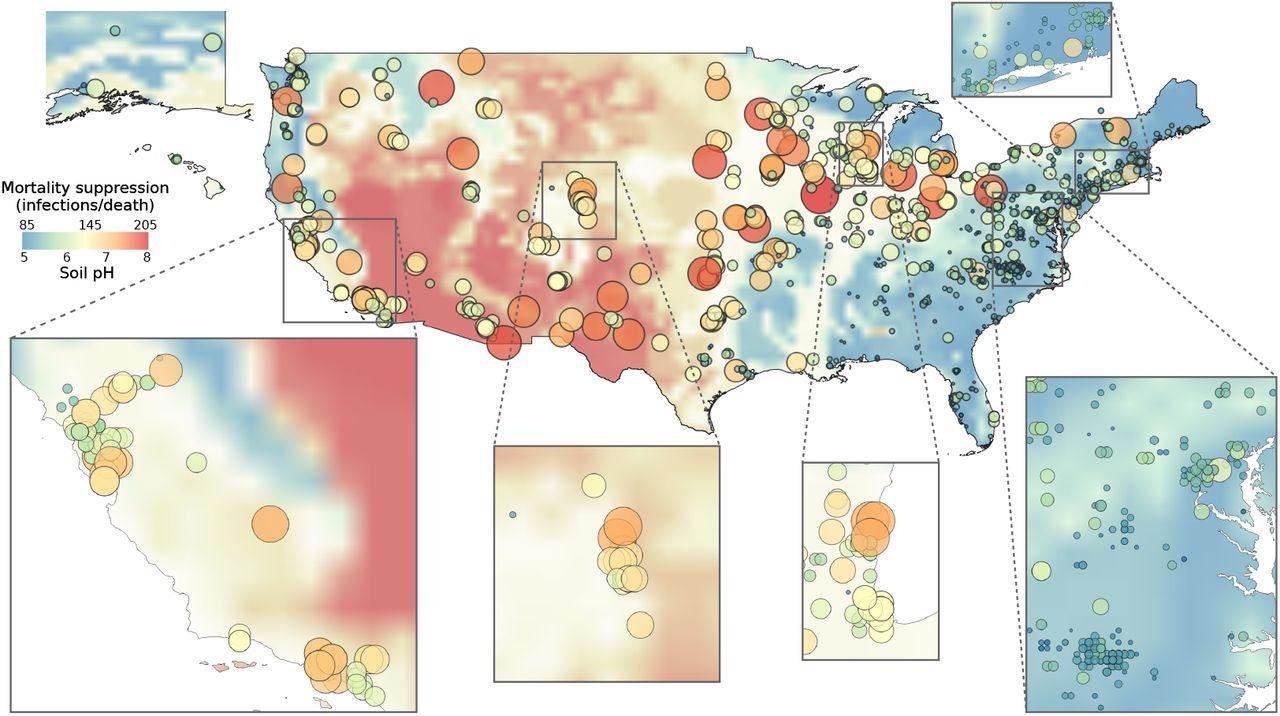 Fungal suppression of COVID-19 mortality varies regionally. In regions where soils tend to be basic (red background shading), indoor-outdoor fungal beta-diversity tends to be low, and fungal suppression of SARS-CoV-2 IFR is high (red dots). By contrast, the opposite trend holds in regions with acidic soils (blue background shading and dots); here, where fungal suppression of SARS-CoV-2 IFR is lessened, SARS-CoV-2 IFR can be high or low depending on whether other factors (e.g., climate, demographics) reduce SARS-CoV-2 IFR.
Fungal suppression of COVID-19 mortality varies regionally. In regions where soils tend to be basic (red background shading), indoor-outdoor fungal beta-diversity tends to be low, and fungal suppression of SARS-CoV-2 IFR is high (red dots). By contrast, the opposite trend holds in regions with acidic soils (blue background shading and dots); here, where fungal suppression of SARS-CoV-2 IFR is lessened, SARS-CoV-2 IFR can be high or low depending on whether other factors (e.g., climate, demographics) reduce SARS-CoV-2 IFR.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
Journal reference:
- Preliminary scientific report.
Ladau, J., Abuabara, K., Walker, A., et al. (2021), “The impact of environmental microbiomes on geographic variation in COVID-19 mortality”, medRxiv preprint, doi: 10.1101/2021.12.14.21267549, https://www.medrxiv.org/content/10.1101/2021.12.14.21267549v1