TB is one of the leading health priorities and a significant cause of death from infectious diseases across the globe. However, the rates of TB detection have been unacceptably low among males, children, and older individuals. Disruptions in TB diagnosis and health services due to the coronavirus disease 2019 (COVID-19) pandemic might have exacerbated the TB-related inequalities.
Study: Inequalities in the impact of COVID-19-associated disruptions on tuberculosis diagnosis by age and sex in 45 high TB burden countries. Image Credit: NIAID
About the study
In the present study, researchers investigated whether COVID-19 impacted the rates of TB case detection and service provision among 45 nations with high TB, high HIV/TB, and high MDR-TB burdens between 2013 and 2019.
Trend-estimated notifications were compared to observed notifications during 2020 to estimate the count of individuals for whom TB diagnosis must have either been delayed or missed or delayed. Risk ratios (RR) of delayed or missed TB diagnosis were calculated for children (aged below 15 years), elders (aged ≥ 65 years), and adults (aged between 15 years and 64 years). Random-effects meta-analysis was performed to comparatively assess the RR values by age and sex at a global level.
Case notifications were obtained from nation-level TB programs and reported to the WHO. The data recorded the number of individuals diagnosed with TB and notified the healthcare system between 2013 and 2020. Poisson regression modeling was used to estimate the number of notifications during 2020 in every nation. For identifying delayed or missed notifications (estimated notifications minus observed notifications), the model-predicted estimates for 2020 were compared to the actual number of notifications.
The risk of undiagnosed TB due to SARS-CoV-2 infection-related disruptions was calculated. Parametric bootstrap sampling was used for RR estimations. Three sensitivity analyses were performed. First, the team separately analyzed nations with elevated burdens of TB, HIV/TB, and MDR-TB. They excluded nations lacking COVID-19-related disruptions in TB diagnosis (described as nations with notifications for ≥1 population group greater than estimated). Lastly, they excluded nations wherein the model was regarded as insufficient or limited data was available (for <5 years before 2020).
Results
In total, 325,964 (seven percent), 4,079,324 (82%),5 95,840 (12%) children, adults, and elders, respectively, were notified during 2020, of which 2,917,005 (62%) and 1,758,159 (38%) were men and women, respectively. In comparison to the observed case notifications, for predicted 195,449, 1,126,133, and 235,402 of 517,168 children (38%), 5,170,592 adult individuals (22%), and 826,563 elders (29%), TB diagnosis was either delayed or missed during 2020 due to the COVID-19 pandemic. The count included 511,546 and 863,916 of the predicted 2,250,097 females and 3,763,363 males, respectively.
In total, 2,334,656 (seven percent of all age-stratified notifications) children, 27,448,386 (82%) adults, and 3,828,418 (11%) elder individuals with TB were notified during the study period across 45 nations, including 19,961,383 (64% of all sex-stratified notifications) men and 11,346,972 (36%) women. In 24 out of 42 nations (57%) with lesser than estimated notifications for adults or children, evidence was found (strong evidence for 21 nations) of delayed o missed TB diagnosis due to the pandemic in association with children.
In 10 nations (24%), evidence was found (hard evidence for eight nations) of delayed or missed TB diagnosis due to SARS-CoV-2 infections associated with adults. In 29 out of 41 nations (70%) with lesser than estimated notifications, evidence was found (hard evidence for 24 nations) of delayed or missed TB diagnosis due to SARS-CoV-2 infections in association with elders. In nine nations (23%), evidence was found (hard evidence for seven nations) of delayed or missed TB diagnosis due to SARS-CoV-2 infections in association with males. Hard evidence was found for the East Mediterranean region (RR 1.8) and European region (RR 1.3) that case notifications were disproportionately impacted for children compared to adults.
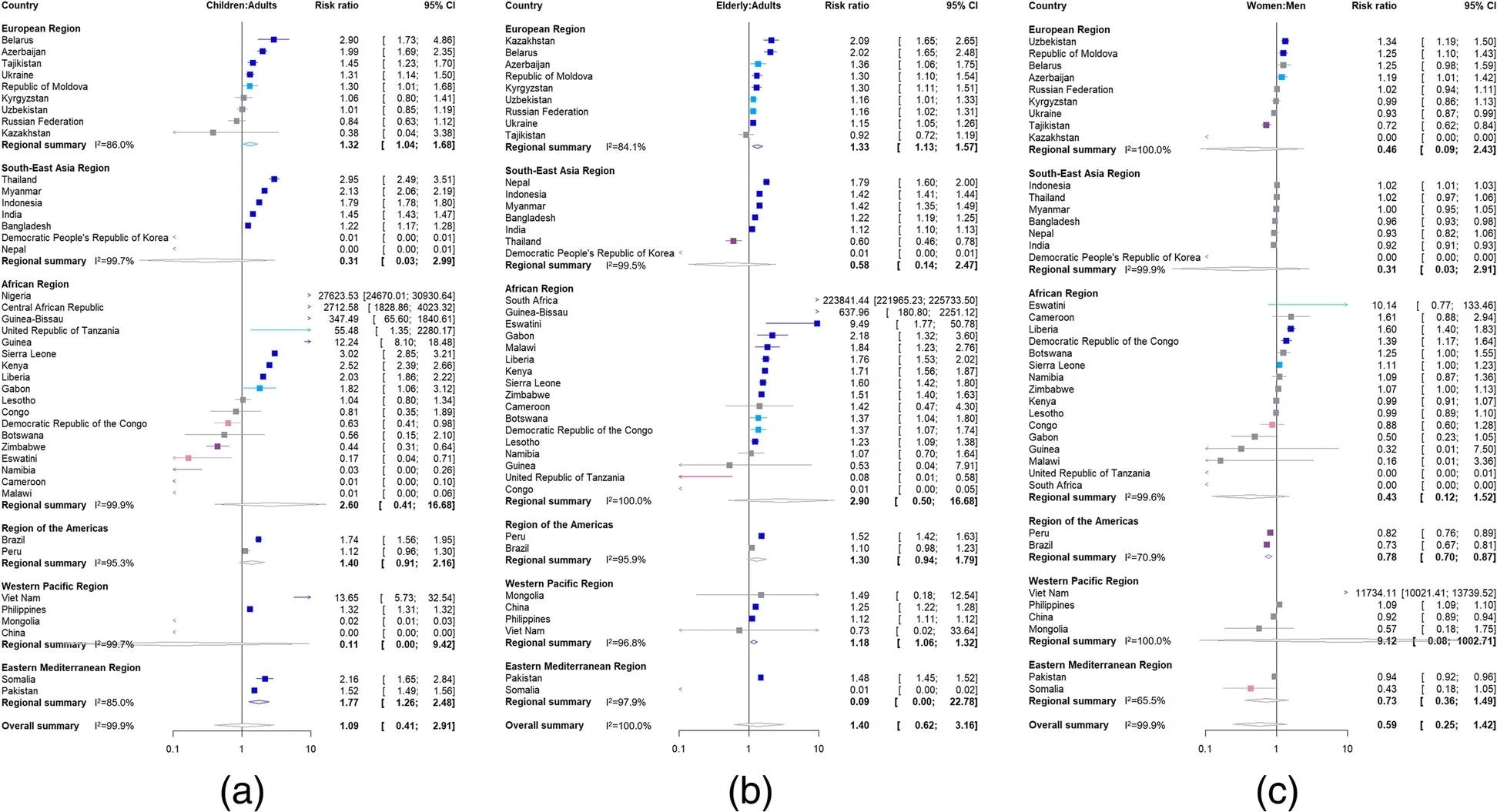
Risk ratios for disruption to tuberculosis notifications due to the pandemic for 45 high TB, TB/HIV and MDR-TB burden countries by WHO region for a children aged < 15 years compared to adults aged 15–64 years, b elderly aged ≥ 65 years compared to adults aged 15–64 years and c women aged ≥ 15 years compared to men aged ≥ 15 years. Risk ratios > 1 imply that the first population (children, the elderly or women) had a larger proportion of diagnoses missed or delayed in 2020 as a result of the pandemic. Risk ratios < 1 imply that the second population (adults or men) had a larger proportion of diagnoses missed or delayed in 2020 as a result of the pandemic. Countries, where there were more notifications in both the comparator and reference groups, were excluded from the meta-analysis. Colors indicate strength of evidence; no evidence for a risk ratio different to 1 (grey), strong evidence for a risk ratio > 1 (dark blue), evidence for a risk ratio > 1 (light blue), weak evidence for a risk ratio > 1 (green), strong evidence for a risk ratio < 1 (purple), evidence for a risk ratio < 1 (dark pink) and weak evidence for a risk ratio < 1 (light pink)
However, no such evidence was found at an international level (RR 1.1) and in other WHO regions. Hard evidence was found for the European region (RR 1.3) and West Pacific region (RR 1.2) that case notifications were disproportionately impacted for elders compared to adults. However, no such evidence was found on a global scale (RR 1.4) and in other WHO regions. Hard evidence indicated that case notifications were disproportionately impacted for males compared to females in WHO’s American region (RR 0.8), with no such evidence at a global scale (RR 0.6). Similar findings were obtained by separately analyzing the nations with elevated burdens of TB, MDR-TB, and HIV/TB.
Overall, and in the majority of sex and age groups, a decrease in TB case notifications during 2020 compared to the predicted numbers was observed. However, in 18 nations, the observed case notifications exceeded the expected notifications in ≥1 sex or age group; Republic of Central Africa, Republic, Cameroon, Congo, China, Eswatini, Democratic People’s Republic of Korea, Guinea-Bissau, Ethiopia, Kazakhstan, Mongolia, Malawi, Nigeria, Nepal, South Africa, Somalia, Vietnam, Zambia and the United Republic of Tanzania. Excluding the 18 nations showed global evidence of notifications disproportionately impacting children more than adults (RR 1.6) and elders more than adults (RR 1.4).
Overall, the study findings showed that international TB notification rates were 22% lesser than estimated for adult individuals (but similar rates for women and men), while for elders and children, the rates were 38% and 29% lesser than estimated, respectively. The findings indicate that a considerable fraction of individuals is likely suffering from undiagnosed TB due to the SARS-CoV-2 pandemic and are at an increased risk of disease transmission. However, high levels of heterogeneity indicated that the risk inequalities were not evident globally.