Skip to:
Knee replacement surgery, also called knee arthroplasty (KA), is the surgical process of replacing a damaged knee. The surgery is mainly performed to relieve knee pain and physical disability, and about 80% of patients show good clinical outcomes after KA. However, some people experience acute pain just after surgery, which can develop into chronic pain of moderate-to-severe intensity in 15 to 20% of patients.
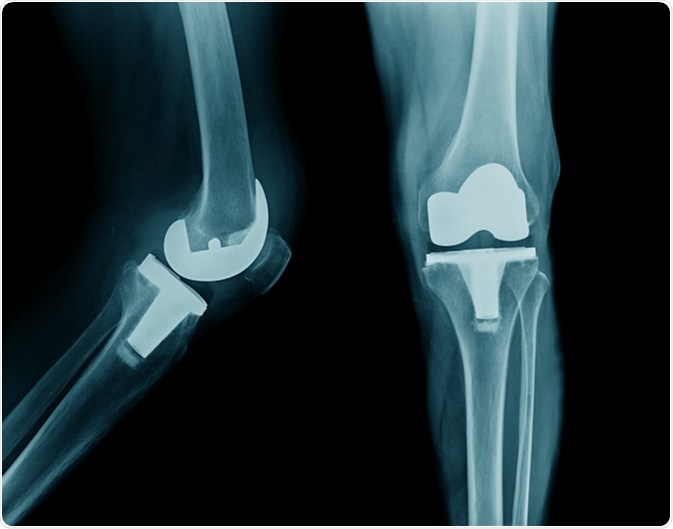
X-ray image total knee arthroplasty. Image credit: Tridsanu Thopet / Shutterstock
What are the risk factors for chronic pain after KA?
Identifying risk factors for postoperative pain is important in order to develop therapeutic interventions and improve postoperative outcomes. The risk factors can be preoperative, intraoperative, and postoperative.
Regarding preoperative risk factors, presence of severe pain, comorbid conditions, or poor psychological status can impact the pain sensation after KA. Several studies have shown that the intensity of preoperative pain is directly proportional to the postoperative level of pain.
Presence of comorbidities that are associated with chronic pain also increases the chance of developing postoperative pain, suggesting that the discomfort may be due to altered pain sensation in the brain. Moreover, pain catastrophizing, which is defined as a tendency to exaggerate the pain intensity, is considered to be an independent risk factor for chronic postoperative pain.
Certain intraoperative factors, such as type and duration of surgery and type of implant, can also influence the pain after KA.
Regarding postoperative risk factors, presence of acute pain just after surgery is occasionally linked to chronic postoperative pain; however, little is known about this association.
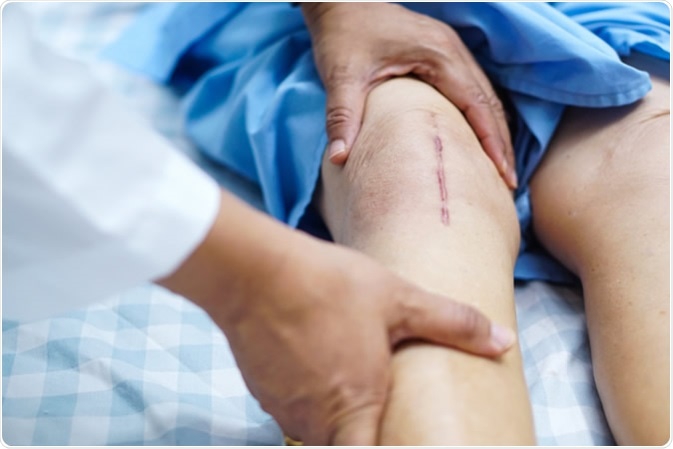
Patient scars from total knee joint replacement arthroplasty. Image Credit: Sasirin Pamai / Shutterstock
How is the pain developed after KA?
Although the exact mechanism of pain development is not fully known, it is believed that multiple factors are associated with postoperative chronic pain. Central sensitization caused by altered function of the central nervous system is believed to be a strong contributor for chronic pain after KA. It reduces the pain threshold and makes individuals more sensitive to pain stimulation.
Presence of prosthetic joint infection is a potential cause of chronic pain after KA, which is often treated with two-stage revision arthroplasty with targeted antibiotic therapy. During the first stage of treatment all lingering sources of infection for example all components, cement and affected soft tissues are removed and replaced with an antibiotic-impregnated spacer. The second stage replaces the prosthetic joint.
Moreover, development of acute knee instability due to a lack of soft tissue balancing is another major cause of postoperative pain. Instability can increase the rate of polyethylene wear, the loss of polyethlene liner height over time along with resorption of bone around the implant and sometimes associated subsidence of the implant components.
Patellofemoral pain, discomfort at the front of the knee and around the kneecap, caused by improper placement of patellar button during patellofemoral resurfacing is associated with chronic pain and stiffness after KA.
Deep vein thrombosis, which is defined as formation of blood clot in deep veins, can be developed as a consequence of KA. It can permanently damage the valves in the vein, leading to postoperative chronic pain.
Other factors that are associated with postoperative pain include soft tissue inflammation, neurological disorders (spinal stenosis, radiculopathy, complex regional pain syndrome), and psychological distress (anxiety and depression).
How does pain after KA affect quality of life?
Since one of the major goals of KA is to cure uncomfortable pain, people who experience intensified pain after the surgery undergo emotional distress, such as anxiety, depression, and overall dissatisfaction and disappointment. Moreover, long-lasting pain can significantly affect the health-related quality of life. It can cause functional difficulties, increased consumption of pain-killers, sleep disturbances, and poor general health.
Because of the physical and psychological challenges, people often experience social isolation and suffer from loneliness. This subsequently affects overall health status and health-related quality of life.
Chronic pain after KA may also place an economic burden on the individual and local healthcare providers; mainly due to an increased number of appointments with healthcare professionals for effective pain diagnosis and management. Moreover, costs associated with purchase of prescribed and over-the-counter medicines considerably affect the health-related economy.
What are the biomarkers for predicting postoperative knee pain?
Presence of certain biomarkers in the body fluid can effectively explain the development and intensity of painful sensation after KA. Studies have found that increased blood levels of some inflammatory markers, such as C-reactive protein (CRP) and interleukin-6 (IL-6), before surgery serves as a sensitive predictor of postoperative pain. Similarly, increased preoperative levels of these biomarkers in the synovial fluid is associated with poor postoperative outcome in terms of increased pain.
Another important biomarker for pain prediction is the level of leptin in the synovial fluid.
In a study following more than 200 women with osteoarthritis undergoing hip and knee replacements , higher concentrations of leptin in synovial fluid were associated with worse postoperative pain.
How to treat postoperative knee pain?
Pain management after KA is essential to improve health-related quality of life. Despite the absolute necessity of pain management strategies, there are no established guidelines to control chronic pain after KA. The intensity of the acute postoperative pain is generally managed by oral anesthesia, intravenous patient-controlled analgesia, nerve blocks, periarticular injections, and epidural analgesia.
Among these interventions, those with fewer side-effects like periarticular injection using local anesthetics, opioids, non-steroidal anti-inflammatory drugs, and corticosteroids are an attractive choice for pain management. However, long-term use of opioids is associated with many adverse side-effects, such as nausea, vomiting, constipation, cardiopulmonary problems, etc.
A multifactorial analysis of pain is essential for managing chronic pain after KA. For example, pain associated with surgery can be treated with physiotherapy and secondary resurfacing. Similarly, nerve injury related pain can be best managed by neuropathic pain medicines, radiofrequency ablation, and denervation. For regional and nociceptive pain, administration of opioids and analgesics can be effective.
Further Reading
Last Updated: Jul 31, 2019