Aug 3 2017
Representatives from the London Assembly and local authorities in the Capital are set to meet with third sector and public health representatives in a roundtable meeting hosted by biopharmaceutical company, AbbVie, on World Hepatitis Day. Meeting delegates will agree priority actions for London, helping the Capital to contribute to the UK Government’s 2030 commitment to eliminate hepatitis C as a public health threat.
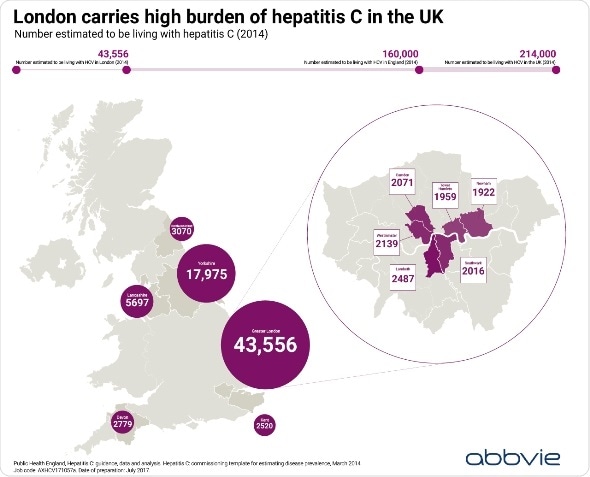
While progress has been made in reducing the number of deaths in those with advanced disease, areas like London still carry a high burden and addressing this requires a clear and consistent local focus. Latest figures from Public Health England estimate that 43,500 people are living with the now curable blood borne virus in London - among the highest prevalence in England - with 40% failing to access treatment support. A significant challenge to eliminating hepatitis C is that many people remain undiagnosed - around 17,500 in London alone. Without treatment, hepatitis C can develop into potentially fatal liver cancer or end stage liver disease.
Local politicians, together with representatives from Public Health England and the British Medical Association, will agree priorities with clinicians, patient advocacy and voluntary sector leads to deliver changes in the way that hepatitis C is prevented, diagnosed, and treated in the Capital.
One innovative model of care being shared at today’s meeting is a peer support scheme run by King’s College Hospital NHS Foundation Trust in partnership with The Hepatitis C Trust. The scheme will operate in the London Borough of Lambeth, which has the highest estimated prevalence of hepatitis C in London. Nearly 2,500 people are thought to be living with the virus in the borough, with an estimated 1,800 either untreated or undiagnosed. Lizzie Smith, Program Manager for Hepatitis C Operational Delivery Network in South London & Kent said:
This new partnership between King’s College Hospital and The Hepatitis C Trust will provide an opportunity for service users within drug and alcohol addiction services to learn from trained peer-educators about risk factors for hepatitis C and the effective new treatments that are available. The project will also enable people with a diagnosis of hepatitis C to directly access appointments with a specialist clinician to discuss treatment, with the option of ongoing peer-support. This work will ultimately improve access to treatment for hepatitis C.
Speaking at the roundtable meeting today, Professor Ashley Brown, Consultant Hepatologist, St Mary’s Hospital, and Deputy Chair of the Hepatitis C Coalition said:
Achieving the national ambition to eliminate hepatitis C as a public health threat by 2030 requires a local focus on the issues we still face. We can’t rely on people to report their symptoms and follow up with their GP to get diagnosed and eventually treated. We need to move faster. Today is about getting agreement on how we deliver a step change in the way that we prevent, diagnose, treat and support people with hepatitis C in London.
Source: http://www.abbvie.co.uk/