Researchers from the University of Michigan Rogel Cancer Center have conducted clinical trials with a new drug targeting pancreatic cancer and the initial results are promising. The results of their study titled, “Dose Escalation Trial of the Wee1 Inhibitor Adavosertib (AZD1775) in Combination With Gemcitabine and Radiation for Patients With Locally Advanced Pancreatic Cancer,” was published in the latest issue of the Journal of Clinical Oncology.
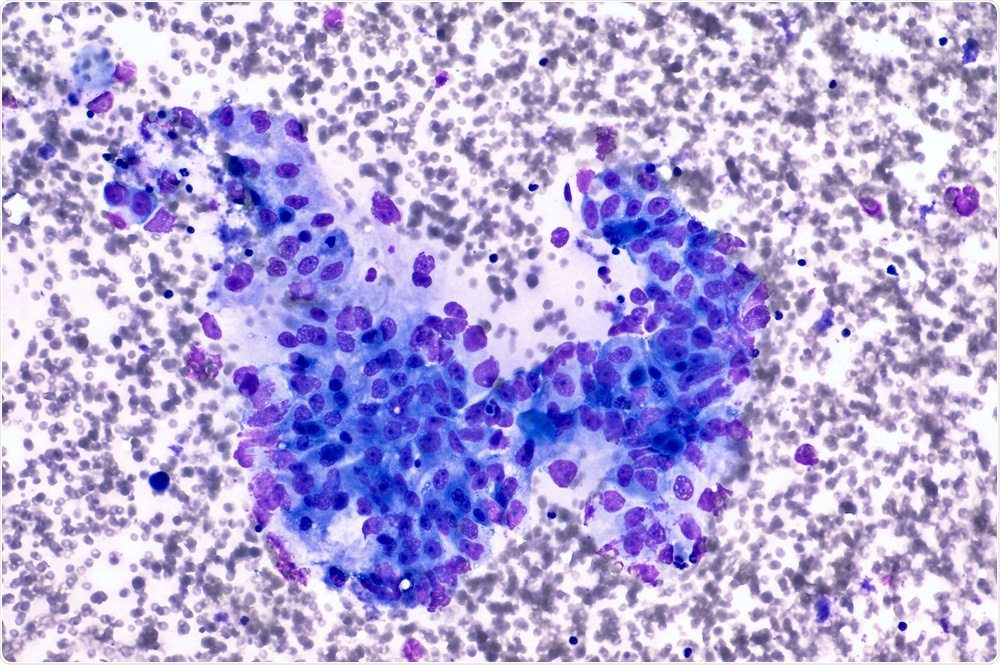 David Litman | Shutterstock
David Litman | Shutterstock
Pancreatic cancer is one of the deadliest cancers, with the average five-year survival rate at a dismal 9 percent. It is commonly known to spread to distant parts of the body and is usually resistant to chemotherapy and radiation therapy. Over the past two decades, researchers at this institute have been studying the various ways in which pancreatic cancer could be tackled.
According to the Centre for Disease Prevention and Control (CDC), persons over the age of 65 are more at risk of pancreatic cancer. Males, tobacco users, obese and overweight individuals, diabetics, those with chronic pancreatitis and those who have a family history of pancreatic cancer are at greatest risk of this cancer, says the CDC.
The phase 1 clinical trial was conducted using the molecule named AZD1775. The drug works by inhibiting the enzyme Wee1 kinase. Wee1 kinase has been shown to play a significant role in repair of damaged DNA. Cancer cells are particularly susceptible to fatal DNA damage as their genomes are unstable, compared to healthy cells.
The researchers explained that chemotherapy with Gemcitabine, a standard chemotherapy drug, and radiation therapy used for pancreatic cancer can lead to damage to the DNA. Pancreatic cancer cells can repair damaged DNA and thus reduce the efficacy of the treatment. Study leader, Meredith Morgan, Ph.D., explained that the new molecule was able to prevent the pancreatic cancer cells from protecting themselves from chemotherapy induced DNA damage. This increased the efficacy of Gemcitabine and radiotherapy. The treatment had minimal effects on normal cells, she explained.
If we can disable the DNA damage response in pancreatic cancer cells, it might eliminate treatment resistance and sensitize the cancer to the effects of both radiation and chemotherapy.”
Kyle Cuneo, M.D., Lead Author
The study involved 34 patients with locally advanced pancreatic cancer. The patients had received radiation, gemcitabine and AZD1775. The dose of the AZD1775 was escalated using “a time-to-event continual reassessment method”. This meant that the dose was increased based on the toxicities seen within the first 15 weeks of the treatment.
Overall survival improved in patients following this treatment regime, compared to those who received chemotherapy and radiation alone. Average duration of survival without the new drug was around 12 to 14 months. With the addition of the new drug the survival increased to an average of 22 months and the disease-free state was seen for an average of 9 months with the new drug.
If we're ever going to cure pancreatic cancer, we're going to need effective systemic treatment as well as local therapy. Our data suggests that AZD1775 can do both.”
Ted Lawrence, M.D., Ph.D., Co-Author
Cuneo said, “Adding AZD1775 to radiation and gemcitabine was relatively well tolerated with encouraging survival results. Further studies with this promising combination are needed.”
Authors concluded, “AZD1775 in combination with gemcitabine and radiation therapy was well tolerated at a dose that produced target engagement in a surrogate tissue. The overall survival is substantially higher than prior results combining gemcitabine with radiation therapy and warrants additional investigation.”
The experts have added that this new drug is also being tested for other cancer types such as breast and ovarian cancer as an addition to the standard chemotherapy and radiation therapy.
The molecule is yet to receive an FDA approval. The phase 1 trial was funded by the National Cancer Institute grants and the drug AZD1775 is manufactured by AstraZeneca.
Journal reference:
Cuneo, K., et al. (2019). Dose Escalation Trial of the Wee1 Inhibitor Adavosertib (AZD1775) in Combination With Gemcitabine and Radiation for Patients With Locally Advanced Pancreatic Cancer. Journal of Clinical Oncology. https://ascopubs.org/doi/10.1200/JCO.19.00730.