People with diabetes suffer from chronic and non-healing wounds, often leading to severe infection and, eventually, amputation of the limb. The essential treatment for these wounds is the continuous application of medicines and the regular changing of bandages to prevent infection. Now thanks to biomedical engineers, -there's a remote control or "smart" bandage that can help treat chronic wounds.
The new device can be controlled wirelessly via a smartphone-sized platform to deliver the medications to the wound with independent dosing without the need to see the patient.
The breakthrough bandage, developed by Dr. Ali Tamayol, associated professor at the University of Connecticut School of Dental Medicine, School of Medicine, and School of Engineering, and researchers from the University of Nebraska-Lincoln and Harvard Medical School, is equipped with miniature needles that deliver the drugs to the wound.
"This is an important step in engineering advanced bandages that can facilitate the healing of hard to treat wounds. The bandage does not need to be changed continuously," Dr. Tamayol said.
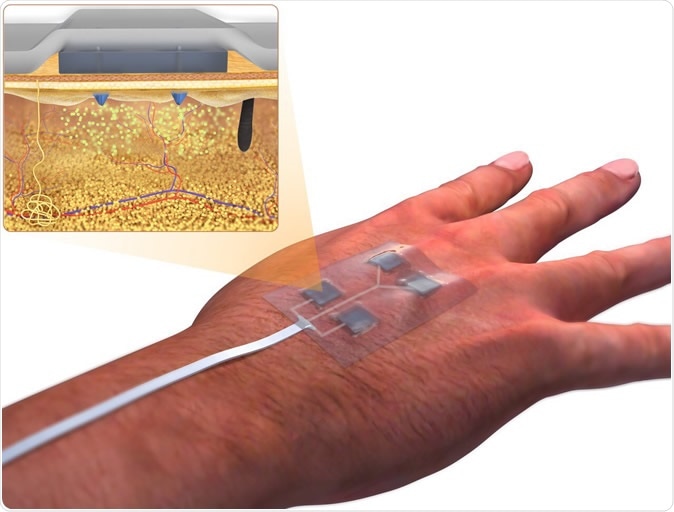
A UConn researcher has helped develop a new "smart bandage" that could improve clinical care. (courtesy of Dr. Ali Tamayol)
No need to remove the bandage
In patients with chronic wounds, mostly as a result of type 2 diabetes, regular bandage change is needed every two days to prevent infection and to apply for the medicines. The new smart bandage, however, doesn't require removal to administer the needed topical agents.
In wound healing, it may take a lot of time and range of processes of treatment. Doctors prescribe different medications needed at various stages of tissue regeneration. With the new bandage, the medicines can be administered with reduced invasiveness.
How does it work?
First, of its kind, the wearable "smart" bandage is a programmable platform that was engineered to actively deliver different drugs through miniature needles into deeper layers of the wound bed. Further, aside from reducing the opening of the bandage to apply for medicines, the device introduces the drugs equally across the wound.
To test the device, they used it on diabetic mice. They found that it helped in hastening wound closure, angiogenesis, re-epithelization, and hair growth compared to standard delivery of drugs.
The device works with a platform, where the provider can control the release of the drugs wirelessly. The drugs are administered via very tiny needles that can penetrate the deeper layers of the wound bed, with reduced and minimal pain and inflammation.
The research, published in the journal Advanced Functional Materials, was the first one to show how wireless delivery of drugs can help treat chronic wounds. First, the scientists tested the device on cells, and then on diabetic mice with full-thickness skin injury.
The new device and technology are promising, which has shown efficacy in promoting wound healing and lack of scar formation in diabetic animals. In humans, the scientists plan to test the device, as it shows promise as a replacement to existing wound care systems and traditional bandages. The scientists believe that the breakthrough device can help reduce mortality associated with chronic wounds, and it would change the way diabetic wounds are treated.
Chronic wounds as a complication of diabetes
Type 2 diabetes is a chronic and long-lasting disease characterized by increased levels of blood sugar. If it's not treated and controlled, it may lead to many complications. One of the most devastating complications is poor healing of wounds, which can lead to amputations.
When a person has diabetes, wounds take longer to head, predisposing him to a higher risk of infections and other complications. In the United States, about 30.3 million are living with a type of diabetes, and about one in four of those will experience a foot ulcer. Moreover, about 15 percent of those with foot ulcers progress to amputation.
Journal reference:
Derakhshandeh, H., Aghabaglou, F., McCarthy, A., Mostafavi, A., Wiseman, C., Bonick, Z., Ghanavati, I., Harris, S., Kreikemeier‐Bower, C., Mousavi, S. M., Rosenbohm, J., Yang, R., Mostafalu, P., Orgill, D., Tamayol, A., A Wirelessly Controlled Smart Bandage with 3D‐Printed Miniaturized Needle Arrays. Adv. Funct. Mater. 2020, 1905544. https://doi.org/10.1002/adfm.201905544